Albuterol for Pulmonary Edema? (TMC Practice Question)
The video breaks down a sample TMC practice question about using albuterol to treat pulmonary edema. Is this possible?
💥TMC Test Bank [Practice Questions] ➜ ➜ ➜ https://bit.ly/3QNqwLX
💥Daily Practice Questions [via Email] ➜ ➜ ➜ http://bit.ly/2NnXh3C
➡️ Question
A 57-year-old female patient with acute pulmonary edema is dyspneic and shows signs of wheezing. The resident physician has ordered an albuterol breathing treatment via SVN. Which of the following would you recommend?
A. Administer acetylcysteine instead of albuterol
B. Perform the therapy with supplemental oxygen
C. Perform the treatment as ordered
D. Administer a diuretic and oxygen therapy
Once you start your career and begin working as a respiratory therapist, this is something you will run into far too often. A nurse or new physician will hear wheezing while listening to breath sounds and automatically request you to administer an albuterol breathing treatment. This can be frustrating because wheezing in patients with CHF and pulmonary edema is usually due to fluid overload, not bronchospasm. Therefore, in general, acute pulmonary edema is best managed with a diuretic such as Lasix. Oxygen therapy is also usually indicated due to the presence of hypoxemia. And in general, NPPV (e.g., BiPAP) is typically indicated for these patients.
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:37 - Practice Question
1:13 - Explanation
2:03 - Correct Answer
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#respiratorytherapyzone #tmcexam #tmcpracticequestion
32
views
Mechanical Ventilation *MADE EASY* - Basics Explained ❗
Mechanical ventilation is a life-saving intervention for patients who are unable to breathe on their own. This video provides an overview of this topic!
💥Mechanical Ventilation Basics [Full Guide] ➜ ➜ ➜ https://bit.ly/3i4m1v1
➡️ Mechanical Ventilation
Mechanical ventilation involves the use of a machine to help a patient who is unable to breathe spontaneously. Therefore, it is indicated for patients who are unable to maintain adequate ventilation. Ventilation is the process of taking in oxygen during inhalation while removing carbon dioxide during exhalation. When a patient is unable to do this on their own, a ventilator can be used to assist with or completely take over the ventilatory process.
➡️ Indications
-- Insufficient oxygenation
-- Insufficient ventilation
-- Acute lung injury (ALI)
-- Severe asthma
-- Severe hypotension
-- Inability to protect the airway
-- Upper airway obstruction
Contraindications
A patient cannot survive without adequate ventilation and oxygenation. Therefore, there are no true contraindications for mechanical ventilation. However, there may be some circumstances where a patient chooses not to receive mechanical ventilation, such as when they have a DNR (Do Not Resuscitate) order in place. This means that the patient legally wishes not to receive life-saving interventions. In these cases, the patient’s goals of care must be respected.
Principles of Mechanical Ventilation
-- Ventilation
-- Oxygenation
-- Lung compliance
-- Airway resistance
-- Deadspace ventilation
-- Respiratory failure
💥Mechanical Ventilation Basics [Full Guide] ➜ ➜ ➜ https://bit.ly/3i4m1v1
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:40 - Mechanical ventilation
0:53 - Ventilation
1:11 - Indications
1:21 - Insufficient ventilation
1:50 - Acute lung injury (ALI)
2:00 - Severe asthma
2:16 - Severe hypotension
2:27 - Inability to protect the airway
2:40 - Upper airway obstruction
3:13 - Contraindications
3:52 - Principles of Mechanical Ventilation
4:06 - Ventilation
4:11 - Oxygenation
4:17 - Lung Compliance
4:22 - Airway Resistance
4:28 - Deadspace Ventilation
4:36 - Respiratory Failure
4:55 - What is a Mechanical Ventilator?
6:22 - Benefits
7:31 - Complications
8:41 - Types
9:00 - Positive-Pressure Ventilation
9:30 - Negative-Pressure Ventilation
9:57 - Examples
10:25 - Invasive Mechanical Ventilation
10:37 - Primary Types of Artificial Airways
11:08 - Noninvasive Ventilation
11:29 - Types
11:55 - Ventilator Modes
12:10 - Ventilator Control Variables
12:16 - Volume Control (VC)
12:41 - Pressure Control (PC)
13:14 - Types of Ventilator Modes
13:56 - Primary Ventilator Modes
14:06 - Assist/Control (A/C)
14:39 - SIMV
15:11 - Ventilator Settings
16:57 - Initiation of Mechanical Ventilation
17:20 - Initial Ventilator Settings
19:03 - Artificial Airways
19:34 - Other Types of Artificial Airways
20:26 - Drugs Used in Mechanical Ventilation
21:06 - Analgesic Agents
21:34 - Managing Patients on the Ventilator
22:33 - Monitoring Mechanically Ventilated Patients
23:06 - Mechanical ventilation monitoring
23:19 - Ventilator Alarms
23:36 - Several types of ventilator alarms
23:54 - Ventilator Waveforms
24:32 - Ventilator Troubleshooting
26:21 - Ventilator Weaning
26:51 - Type of respiratory disease
27:28 - Weaning Criteria
28:48 - Spontaneous Breathing Trial
29:24 - Extubation
30:11 - Neonatal Mechanical Ventilation
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#mechanicalventilation #ventilator #mechanicalventilator
41
views
Severe Epidemic Enterovirus Respiratory Syndrome (SEERS) | WARNING 2025 ❗️
What is Severe Epidemic Enterovirus Respiratory Syndrome (SEERS)? We created this video to cover the medical definition and provide a brief overview of this topic.
💥What is SEERS? [Full Guide] ➜ ➜ ➜ https://bit.ly/3oW3QPY
➡️ Severe Epidemic Enterovirus Respiratory Syndrome (SEERS)
Severe Epidemic Enterovirus Respiratory Syndrome (SEERS) is a hypothetical disease, as there is no known condition with this specific name. However, it appears to be a combination of terms related to respiratory infections and enteroviruses.
➡️ Enteroviruses
Enteroviruses are a group of RNA viruses that include polioviruses, coxsackieviruses, echoviruses, and others. They can cause a variety of illnesses, such as hand, foot, and mouth disease, meningitis, and encephalitis. Some enteroviruses can also cause respiratory infections, but these are typically not as severe as other respiratory illnesses, such as Severe Acute Respiratory Syndrome (SARS) or Middle East Respiratory Syndrome (MERS). Both SARS and MERS are caused by coronaviruses and can lead to severe respiratory infections, causing symptoms such as fever, cough, and shortness of breath. SARS emerged in 2002–2003, while MERS was first reported in 2012. Both have been associated with high mortality rates and global public health concerns.
➡️ Epidemiology
In our hypothetical scenario, SEERS emerges in a densely populated urban area, rapidly spreading through respiratory droplets and close person-to-person contact. The virus would likely demonstrate a high reproduction number (R0), indicating its ability to spread quickly and efficiently among susceptible populations. As the outbreak escalates, healthcare systems would become strained, with hospitals and clinics overwhelmed by the surge of patients seeking treatment for severe respiratory symptoms.
➡️ Clinical Manifestations
SEERS would present a range of clinical symptoms, ranging from mild, flu-like symptoms to severe respiratory distress. In mild cases, individuals may experience fever, cough, sore throat, and fatigue. However, as the disease progresses, more severe cases would exhibit symptoms such as difficulty breathing, chest pain, and even acute respiratory distress syndrome (ARDS). The virus’s affinity for the respiratory system could potentially lead to an increased risk of pneumonia, particularly in vulnerable populations such as the elderly, immunocompromised individuals, and those with pre-existing respiratory conditions.
➡️ Treatment and Prevention Strategies
Given the novelty of this hypothetical enterovirus, treatment options for SEERS would initially be limited. Supportive care, such as oxygen therapy and mechanical ventilation, might be required for severe cases. As researchers work to develop targeted antiviral therapies and vaccines, public health measures would play a crucial role in mitigating the spread of the virus.
💥What is SEERS? [Full Guide] ➜ ➜ ➜ https://bit.ly/3oW3QPY
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:43 - SEERS
1:59 - Epidemiology
2:33 - Clinical Manifestations
3:21 - Treatment and Prevention Strategies
4:02 - International Collaboration and Proactive Response
4:40 - Enterovirus vs. Coronavirus
5:06 - Genetic Makeup
5:44 - Structure
6:09 - Transmission and Symptoms
7:01 - Treatment and Prevention
7:49 - SEERS vs. COVID-19
8:49 - Or is it?
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#SEERS #SevereEpidemicEnterovirusRespiratorySyndrome #Pandemic
1.12K
views
1
comment
Incentive Spirometry (Medical Definition) | Quick Explainer Video
What is Incentive Spirometry? We created this video to cover the medical definition and provide a brief overview of this topic.
💥Lung Expansion Therapy [Glossary] ➜ ➜ ➜ https://bit.ly/2Lxqeby
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
➡️ Incentive Spirometry
The potential outcomes of incentive spirometry include:
- Decreased atelectasis
- Improved breath sounds
- Improved chest x-ray
- Increased SpO2
- Increased vital capacity
- Stronger cough
- Improved respiratory muscle performance
➡️ Atelectasis
Atelectasis is a term that refers to a collapse in the alveoli of the lungs. It could be a total collapse of an entire lung or a partial collapse in one or more lobes. As you take a breath in, air moves through your mouth and trachea down through the airways of the lungs until it reaches the tiny air sacs that are known as alveoli. This is where the gas exchange of oxygen and carbon dioxide takes place. Therefore, if air fails to reach this region, it can result in many different problems within the body. When this occurs, the alveoli that are not filled with air cannot expand, and this is what’s known as atelectasis.
➡️ Incentive Spirometer
Incentive spirometry is the most common type of lung expansion therapy used to treat and prevent atelectasis. It only requires the use of a small, disposable, handheld device that helps patients take deeper breaths. The incentive spirometer has a mouthpiece, breathing tube, one-way valve, inhalation chamber, and an adjustable scale that allow you to set an individualized inspiratory goal for each patient. This goal is a predetermined volume of air that is initially set by a respiratory therapist. They should instruct the patient to take 10 deep inspirations through the device every hour while awake to promote lung expansion. These deep breaths are often referred to as sustained maximal inspirations (SMI).
➡️ Technique
This technique can help improve lung function and prevent atelectasis by:
- Mimicking natural sighing
- Stimulating deep breathing
- Expanding the lungs
- Increasing alveolar ventilation
- Improving inspiratory muscle performance
Incentive spirometry is used to help the patient to take slow, deep breaths, increasing their tidal volume and maximizing alveolar inflation. The visual feedback provided by the spirometer helps the patient gauge their progress and motivates them to improve their breathing performance.
💥Lung Expansion Therapy [Glossary] ➜ ➜ ➜ https://bit.ly/2Lxqeby
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:47 - Potential Outcomes
1:02 - Atelectasis
1:45 - Incentive spirometry
2:00 - Incentive Spirometer
2:30 - Sustained Maximal Inspirations
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#respiratorytherapy #incentivespirometer #incentivespirometry
30
views
Intracranial Pressure (ICP) *Quick Explainer Video* 🧠
What is Intracranial Pressure (ICP)? We created this video to cover the medical definition and provide a brief overview of this topic.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
➡️ Intracranial Pressure (ICP)
Intracranial pressure (ICP) is the pressure within the skull, which involves the brain, cerebrospinal fluid (CSF), and blood. It is a critical parameter in the assessment of neurological conditions and brain health. The balance between the volume of the brain, CSF, and blood determines ICP, which typically ranges from 7 to 15 mm Hg in adults. Maintaining an appropriate ICP is crucial for normal brain function, as imbalances can lead to severe neurological complications or even death.
➡️ An increase in ICP may be caused by several factors, including the following:
- Brain swelling (edema)
- Hemorrhage
- Tumors
- Excess CSF production
Elevated ICP can compress and damage brain tissue, impair blood flow, and lead to life-threatening conditions, including brain herniation. Monitoring and managing ICP is essential for patients with traumatic brain injuries, intracranial hemorrhage, or other neurological disorders.
➡️ Symptoms
Symptoms of increased ICP may include:
- Headaches
- Nausea
- Vomiting
- Vision changes
- Seizures
- Altered level of consciousness
➡️ Treatment
Treatment for increased ICP typically involves addressing the underlying cause, such as surgical removal of a tumor or draining excess CSF in cases of hydrocephalus. Medications such as diuretics may also be used to reduce swelling and fluid accumulation in the brain. In severe cases, a procedure called a decompressive craniectomy may be necessary to relieve pressure on the brain. Monitoring and managing ICP is important in preventing and minimizing brain damage in various neurological conditions.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
022 - Increased ICP
045 - Elevated ICP
122 - Symptoms
131 - Treatment
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#respiratorytherapy #respiratorytherapist #Intracranialpressure
118
views
Inspiratory Capacity (IC) | Quick Explainer Video
What is Inspiratory Capacity (IC)? We created this video to cover the medical definition and provide a brief overview of this topic.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
💥PFT Basics [Full Guide] ➜ ➜ ➜ https://bit.ly/2A8ZuvQ
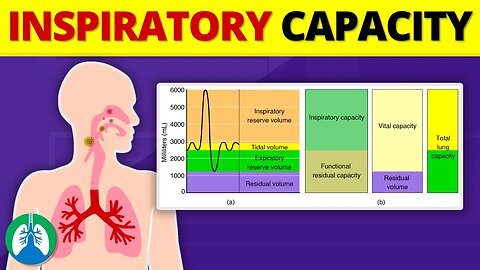
➡️ Inspiratory Capacity (IC)
Inspiratory capacity is the sum of two lung volumes
- Tidal volume (VT)
- Inspiratory reserve volume (IRV)
Tidal volume (VT) is the amount of air that is inhaled and exhaled during normal, quiet breathing. Inspiratory Reserve Volume (IRV) is the additional volume of air that can be inhaled forcefully after a normal, quiet inhalation. Combining the two results is the inspiratory capacity. Inspiratory capacity can be measured using spirometry, which is a non-invasive pulmonary function test that records the volume of air inhaled and exhaled over time. During the test, the patient breathes into a spirometer, which measures airflow and volume. The patient is then instructed to take a normal breath, followed by a forceful inhalation.
The difference between the total volume inhaled, and the tidal volume is the inspiratory reserve volume, which, when added to the tidal volume, gives you the inspiratory capacity. Inspiratory capacity is an essential parameter for evaluating lung function and diagnosing respiratory disorders.
➡️ Conditions that may affect inspiratory capacity include:
-- Restrictive lung diseases: These conditions, such as pulmonary fibrosis, sarcoidosis, and obesity-related hypoventilation, reduce lung compliance and may lead to a decrease in inspiratory capacity.
-- Obstructive lung diseases: Conditions like asthma, chronic bronchitis, and emphysema can cause airway obstruction, leading to difficulty in inhaling the maximum amount of air and, consequently, a reduced inspiratory capacity.
-- Neuromuscular diseases: Conditions such as muscular dystrophy, amyotrophic lateral sclerosis (ALS), and myasthenia gravis can impair respiratory muscle function, reducing the ability to inhale forcefully and resulting in a decreased inspiratory capacity.
Inspiratory capacity is a vital parameter in assessing lung function and can help healthcare professionals diagnose and manage various respiratory disorders. Spirometry is the primary method for measuring inspiratory capacity, providing valuable information for understanding a patient's lung mechanics and guiding the most appropriate methods of treatment.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
💥PFT Basics [Full Guide] ➜ ➜ ➜ https://bit.ly/2A8ZuvQ
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:39 - Tidal volume (VT)
0:46 - Inspiratory Reserve Volume (IRV)
0:58 - Inspiratory Capacity
1:22 - Difference Between the Total Volume
1:41 - Restrictive Lung Diseases
2:01 - Obstructive Lung Diseases
2:18 - Neuromuscular Diseases
2:46 - Spirometry
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#spirometry #inspiratorycapacity #pulmonaryfunctiontesting
25
views
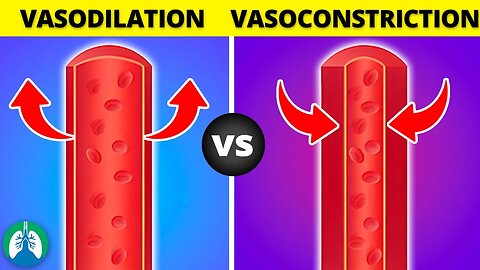
Vasoconstriction vs. Vasodilation *EXPLAINED*
What is the difference between Vasoconstriction and Vasodilation? We created this video to cover the medical definition and provide a brief overview of this topic.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
➡️ Vasoconstriction
Vasoconstriction is the narrowing of blood vessels due to the contraction of the smooth muscle cells in the arterial walls. This process reduces blood flow to certain areas and increases blood pressure. Vasoconstriction is primarily a response to various physiological and pathological conditions, such as:
-- Maintaining body temperature: In cold environments, vasoconstriction helps conserve heat by restricting blood flow to the skin and extremities, thus reducing heat loss.
-- Managing blood pressure: The body may trigger vasoconstriction to increase blood pressure during times of stress or shock.
-- Limiting blood loss: Vasoconstriction is a natural response to injury, as it minimizes blood loss by constricting damaged blood vessels.
-- Sympathetic nervous system activation: Stress, anxiety, and other factors can cause the release of hormones such as norepinephrine and epinephrine, which promote vasoconstriction.
➡️ Vasodilation
Vasodilation is the opposite of vasoconstriction, as it involves the widening of blood vessels due to the relaxation of smooth muscle cells in the arterial walls. This process increases blood flow to specific regions and decreases blood pressure. Vasodilation serves several important purposes, such as:
-- Temperature regulation: In hot environments, vasodilation helps dissipate heat by increasing blood flow to the skin, which promotes sweating and cools the body.
-- Oxygen delivery: During exercise, vasodilation improves oxygen delivery to working muscles by increasing blood flow.
-- Nutrient delivery and waste removal: Vasodilation facilitates the delivery of essential nutrients to tissues and aids in the removal of waste products.
-- Reducing blood pressure: Vasodilation is often a response to the release of hormones and chemicals, such as nitric oxide, which help lower blood pressure.
Vasoconstriction and vasodilation are two opposing processes that regulate blood flow and blood pressure by altering the diameter of blood vessels. Vasoconstriction constricts blood vessels and increases blood pressure, while vasodilation widens blood vessels and reduces blood pressure. Both processes play crucial roles in maintaining homeostasis and supporting the body's various physiological functions.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:43 - Vasoconstriction
1:05 - Maintaining Body Temperature
1:14 - Managing Blood Pressure
1:46 - Vasodilation
2:09 - Temperature Regulation
2:20 - Oxygen Delivery
2:31 - Nutrient Delivery and Waste Removal
2:40 - Reducing Blood Pressure
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#Vasoconstriction #Vasodilation #respiratorytherapyzone
12
views
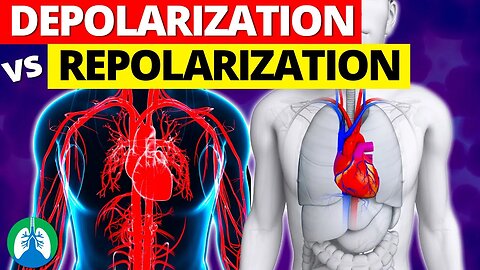
Depolarization vs. Repolarization of the Heart *EXPLAINED*
What is the difference between depolarization and repolarization of the heart? Watch this quick video to find out!
💥Depolarization vs. Repolarization [Full Guide] ➜ ➜ ➜ http://bit.ly/3IJHUz7
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
The heart is composed of specialized cells that work together to maintain a rhythmic heartbeat. The conduction system of the heart is responsible for generating electrical signals that cause the heart to contract and relax. The depolarization and repolarization of these cells play a crucial role in this process.
➡️ Depolarization
Depolarization is the process by which the cells of the heart become less negative and contract. When the cells are at rest, they are negatively charged or polarized. However, when an electrical impulse is generated, the cells become depolarized. This occurs when the concentration of ions changes, specifically when sodium ions rush into the cells. The sodium ions move into the cells through ion channels, which are specialized proteins embedded in the cell membrane. Once the sodium ions enter the cells, they cause the cells to become positively charged, which results in the depolarization of the cells. This causes the cells to contract and push blood through the heart. After depolarization and contraction, the cells need to relax, which is referred to as repolarization.
➡️ Repolarization
Repolarization is the process by which the cells return to their negatively charged state. This occurs when the cell membrane becomes more permeable to potassium ions, which exit the cell. The loss of positive ions causes the cells to become negatively charged again, leading to relaxation. The process of depolarization and repolarization creates the electrical activity of the heart, which is represented as a PQRST waveform on an electrocardiogram (EKG).
➡️ Electrical Activity
The sinoatrial node, also known as the pacemaker, is responsible for setting the heart’s rhythm. The wave of depolarization that originates from the SA node is responsible for causing the atria to contract. This is known as the P wave on an EKG reading. The impulse is received by the AV node, which causes a short delay. This delay is interpreted as the PR intervalon an EKG reading. Then the stimulus moves through the bundle of His, through the left and right bundle branches, and into the Purkinje fibers. This produces ventricular depolarization, and contraction occurs, which can be seen as the QRS complex. Then, the heart enters into a short period of repolarization, which is a period where no electrical activity can be detected. This is known as the ST segmenton an EKG reading. Finally, the heart enters a period of recovery where the SA node is recharged, and another cycle can begin.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:55 - Depolarization
1:47 - Repolarization
2:22 - Sinoatrial Node
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#Depolarization #Repolarization #EKG #heart
51
views
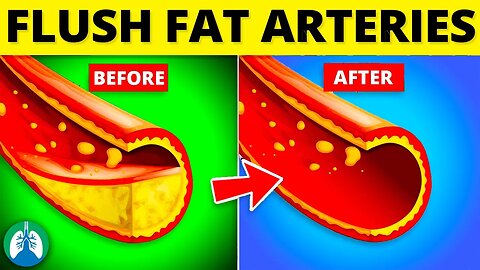
Top 10 Ways to Flush Fat Out of Your Arteries ❤️🔥
What are the best ways to flush fat from your arteries to prevent a heart attack or stroke? Watch this video to find out!
💥Flush Fat From Arteries [Full Guide] ➜ ➜ ➜ https://bit.ly/3OqOayQ
🟦 More Videos You Might Like:
▪ Best Spices to Clean Your Arteries ➜ https://youtu.be/Wz-lSGYV_yI
▪ Best Herbs to Clean Your Arteries ➜ https://youtu.be/5hQXG7nmd90
▪ Herbs to Clear Mucus ➜ https://youtu.be/Dv_P9YdnuJA
▪ Best Foods for Your Lungs ➜ https://youtu.be/vTO7cq9YnuY
➡️ Eat Foods High in Omega-3 Fatty Acids
Omega-3 fatty acids, particularly eicosapentaenoic acid (EPA) and docosahexaenoic acid (DHA), are known for their anti-inflammatory and anti-atherosclerotic properties.
➡️ Exercise Regularly
Engaging in physical activity helps increase blood circulation, which in turn enhances the elasticity and overall function of the arteries. This improved blood flow helps prevent plaque formation by minimizing the opportunity for fat deposits to adhere to the arterial walls.
➡️ Eat More Walnuts
Walnuts are a rich source of heart-healthy nutrients such as Omega-3 fatty acids, particularly alpha-linolenic acid, which has been shown to reduce inflammation and lower the risk of atherosclerosis.
➡️ Quit Smoking
Smoking has been consistently linked to an increased risk of atherosclerosis, heart attacks, and strokes.
➡️ Eat More Citrus Fruits
Citrus fruits, such as oranges, grapefruits, lemons, and limes, are packed with essential nutrients, including vitamin C, potassium, and essential flavonoids.
➡️ Manage Stress
Managing stress effectively plays a critical role in maintaining healthy arteries and reducing the risk of cardiovascular disease.
When the body experiences stress, it releases stress hormones such as cortisol and adrenaline, which trigger the "fight or flight" response. This reaction causes an increase in heart rate and blood pressure, as well as the constriction of blood vessels.
➡️ Eat More Berries
Berries are packed with essential nutrients and antioxidants such as anthocyanins that give them their vibrant colors. This includes strawberries, blueberries, raspberries, and blackberries,
➡️ Control Blood Pressure
High blood pressure, or hypertension, exerts excessive force on the arterial walls, causing them to become damaged, less elastic, and more prone to the accumulation of fatty deposits.
➡️ Eat More Beans
Beans are a powerhouse of nutrients that are known to benefit arterial health. They are rich in soluble fiber, which helps lower LDL cholesterol levels. This process aids in reducing the amount of cholesterol available for plaque formation in the arteries.
➡️ Limit Alcohol Consumption
While moderate alcohol intake, particularly red wine, has been associated with some heart-healthy benefits due to its antioxidant content, excessive alcohol consumption can have detrimental effects on your arterial health.
💥Flush Fat From Arteries [Full Guide] ➜ ➜ ➜ https://bit.ly/3OqOayQ
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:53 - Eat Foods High in Omega-3 Fatty Acids
2:01 - Exercise Regularly
2:51 - Eat More Walnuts
3:50 - Quit Smoking
4:54 - Eat More Citrus Fruits
6:02 - Manage Stress
7:13 - Eat More Berries
8:11 - Control Blood Pressure
9:13 - Eat More Beans
10:04 - Limit Alcohol Consumption
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#arteries #heartattack #stoke
42
views
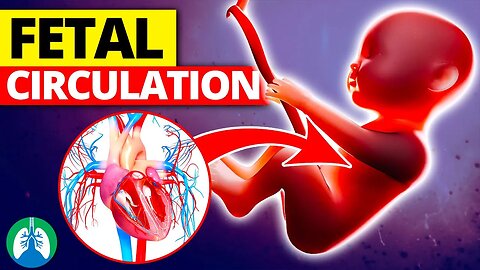
Fetal Circulation *Quick Explainer Video*
What is Fetal Circulation? We created this video to cover the medical definition and provide a brief overview of this topic.
💥Fetal Lung Development [Full Guide] ➜ ➜ ➜ https://bit.ly/2YDRi0c
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
➡️ Fetal Circulation
The process of fetal circulation is different from that of an adult because the fetus is not yet capable of breathing air and obtaining oxygen through the lungs. Instead, oxygen and nutrients are supplied to the fetus by the placenta via the umbilical cord. Oxygenated blood from the placenta enters the fetal body through the umbilical vein and flows into the hepatic circulatory system.
Approximately one-third of this blood goes to the lower trunk and extremities, while the other two-thirds flow through the ductus venosus and directly into the inferior vena cava. This blood in the inferior vena cava is well-oxygenated, but it mixes with venous blood returning from the lower extremities entering the right atrium. Around 50% of this mixed blood is shunted from the right atrium into the left atrium through the foramen ovale, which is a small opening in the interatrial septum. The left atrial blood then flows into the left ventricle and eventually into the ascending aorta, supplying the brain, brachiocephalic trunk, and descending aorta.
Venous blood from the superior vena cava is directed downward into the right atrium, then into the right ventricle, and finally into the main pulmonary artery. However, the relatively low PaO2 and the presence of prostaglandins in the fetal blood result in pulmonary vasoconstriction and increased pulmonary vascular resistance. This leads to a higher pulmonary artery pressure than aortic blood pressure. This causes approximately 90% of the blood entering the pulmonary artery to shunt through the ductus arteriosus, which is a muscular vessel connecting the trunk of the pulmonary artery to the aorta, into the systemic circulation.
Only the remaining 10% of blood actually flows into the lungs. The mixed blood flowing through the ductus arteriosus is routed into the systemic circulation, supplying some of it to the gut, lower extremities, and placenta. The exchange of gases and nutrients between the fetus and the mother takes place through the two umbilical arteries, which carry blood from the fetal abdominal aorta to the placenta. Fetal circulation is a crucial aspect of development and survival, providing the fetus with the oxygen and nutrients necessary for growth and development until it can breathe air and take in oxygen through the lungs.
➡️ Recap
During fetal circulation, 90% of blood bypasses the pulmonary circulation through the foramen ovale and ductus arteriosus (right-to-left shunting). Shunting that continues after birth is considered to be abnormal and may require medical intervention.
💥Fetal Lung Development [Full Guide] ➜ ➜ ➜ https://bit.ly/2YDRi0c
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:28 - Fetal Circulation
0:45 - Oxygenated Blood
1:38 - Venous Blood
2:27 - Mixed Blood
3:11 - Reminder
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#respiratorytherapy #respiratorytherapist #fetalcirculation
40
views
Electrical Impedance Tomography (EIT) | Quick Explainer Video
What is Electrical Impedance Tomography (EIT)? We created this video to cover the medical definition and provide a brief overview of this topic.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
➡️ Electrical Impedance Tomography (EIT)
Electrical Impedance Tomography (EIT) is a noninvasive imaging technique that allows for the assessment of ventilation distribution in real-time. It requires the placement of electrodes around the chest, typically between the fourth and fifth intercostal spaces. The electrodes are connected to a computing device with a monitor, and a small alternating current is sent from a reference electrode to each electrode around the chest. Impedance is measured between adjacent electrodes as the reference point rotates around the chest in a circular motion and repeats measurements approximately 50 times per second. This captures images that are reconstructed into a real-time animated graphic on the screen, referred to as the dynamic image. The images displayed represent a cross-section, similar in perspective to a CT scan, looking from the foot of the bed toward the head of the bed.
➡️ Monitoring
EIT allows for the monitoring of various forms of asynchrony, such as changes in end-expiratory lung impedance, the impact of adjusting the PEEP setting, and lung perfusion at the bedside. The integration of flow, volume, and pressure readings from the ventilator provides diagnostic tools to determine the PEEP level where overdistension and collapse are balanced. With EIT, the impact of changing ventilator settings on the distribution of ventilation can be assessed by comparing images before and after an adjustment is made. Trends can also be utilized to see the stability of ventilator adjustments over time, which is particularly helpful in determining the impact of changing PEEP in patients with certain lung diseases.
➡️ Devices
Modern devices have been equipped with the ability to measure the impedance of fluid distribution throughout the lungs, allowing assessment of lung perfusion at the bedside. It can also detect the effects of excessive spontaneous efforts, which reveals the potentially harmful consequences of spontaneous breathing in patients with severe ARDS. The capacity to monitor ventilation distribution, PEEP response, asynchrony, the impact of excessive spontaneous effort, and lung perfusion at the bedside has ushered in a new era of bedside monitoring focused on the individualization of mechanical ventilation. EIT is a valuable tool for monitoring the impact of mechanical ventilation on the lungs, leading to better patient outcomes and a reduction in the length of stay in intensive care units.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:26 - Electrical Impedance Tomography
0:43 - Electrodes
0:54 - Impedance
1:27 - EIT Monitoring
2:04 - Trends
2:17 - Modern Devices
2:58 - Valuable Tool
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
Andy Adler, CC BY 3.0 -- https://creativecommons.org/licenses/by/3.0 -- via Wikimedia Commons
https://eidors3d.sourceforge.net/tutorial/netgen/extrusion/thoraxmdl06a.jpg
#respiratorytherapy #respiratorytherapist #respiratorytherapyschool
17
views
Kerley B Lines (Medical Definition) | Quick Explainer Video
What are Kerley B Lines? We created this video to cover the medical definition and provide a brief overview of this topic.
💥Kerley B lines [Full Guide] ➜ ➜ ➜ http://bit.ly/3lwod50
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
➡️ Kerley B Lines
Kerley B lines are named after an Irish radiologist by the name of Peter Kerley, who first described these findings in 1933. These are short, thin, horizontal lines located at the periphery of the lungs, usually towards the lung bases. These lines measure around 1-2 centimeters in length and are typically less than 1 millimeter in thickness. The orientation of these lines is perpendicular to the nearby pleura, which is the membrane that covers the lungs. The characteristic appearance of Kerley B lines is due to the fluid-filled interlobular septa, the connective tissue structures that separate the lung's lobules.
➡️ Causes
Interstitial pulmonary edema is the primary cause of Kerley B lines, which occurs when fluid accumulates in the interstitial space of the lungs, leading to increased pressure on the surrounding tissues. Several factors can contribute to the development of interstitial pulmonary edema and the subsequent appearance of Kerley B lines.
➡️ Congestive Heart Failure (CHF)
The heart's ability to pump blood efficiently is compromised, leading to a buildup of fluid in the lungs. The increased pressure in the pulmonary capillaries forces fluid into the interstitial space, causing edema and the formation of Kerley B lines.
➡️ Fluid Overload
Excessive intravenous fluid administration, especially in patients with compromised renal or cardiac function, can lead to fluid accumulation in the lungs. This fluid overload can manifest as Kerley B lines on imaging studies.
➡️ Kidney Failure
Impaired kidney function can result in fluid retention, which can contribute to pulmonary edema and the appearance of Kerley B lines.
➡️ Other Causes
- High altitude pulmonary edema (HAPE)
- Lymphatic obstruction
- Acute respiratory distress syndrome (ARDS)
- Pneumonia
- Pulmonary veno-occlusive disease (PVOD)
➡️ Clinical Significance
Kerley B lines are a valuable diagnostic tool, as they can provide important information about a patient's underlying condition. While the presence of Kerley B lines does not confirm a specific diagnosis, it does indicate the presence of interstitial pulmonary edema, which can help narrow down the list of potential causes. In the context of clinical symptoms and other diagnostic tests, the identification of Kerley B lines can help guide treatment decisions. For example, if a patient with congestive heart failure presents with Kerley B lines, the medical team may adjust the patient's medications or implement other interventions to manage fluid overload and improve heart function. Similarly, in cases of fluid overload due to excessive intravenous fluid administration, recognizing the presence of Kerley B lines can prompt clinicians to reevaluate the patient's fluid management strategy.
💥Kerley B lines [Full Guide] ➜ ➜ ➜ http://bit.ly/3lwod50
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:29 - Kerley B Lines
1:14 - Causes
1:37 - Congestive Heart Failure (CHF)
2:02 - Fluid Overload
2:22 - Kidney Failure
2:34 - Other Causes
2:47 - Clinical Significance
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#respiratorytherapy #respiratorytherapist #KerleyBLines
96
views
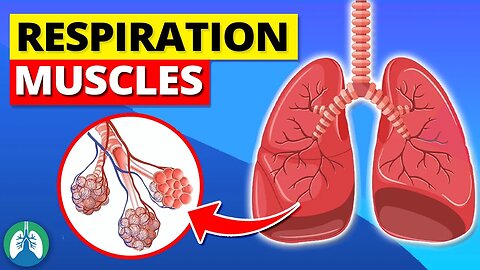
Muscles of Respiration *EXPLAINED* 🫁
What are the muscles of respiration? We created this video to cover the medical definition and provide a brief overview of this topic.
💥Normal Breathing [Full Guide] ➜ ➜ ➜ https://bit.ly/3OXxEU9
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
The process of breathing involves several muscles that work together to facilitate the movement of air in and out of the lungs. The primary muscles of respiration include the following:
➡️ Diaphragm
The diaphragm is the primary muscle responsible for breathing. It's a large, dome-shaped muscle that separates the chest cavity from the abdominal cavity. When the diaphragm contracts, it flattens and moves downward, increasing the volume of the chest cavity and drawing air into the lungs. When it relaxes, the diaphragm moves upward, decreasing the volume of the chest cavity and forcing air out of the lungs.
➡️ Intercostal Muscles
There are two types of intercostal muscles:
- External
- Internal
The external intercostal muscles are involved in inspiration, while the internal intercostal muscles are involved in expiration. During inspiration, the external intercostal muscles contract, lifting the ribs and expanding the chest cavity. During expiration, the internal intercostal muscles contract, pulling the ribs downward and reducing the chest cavity volume, forcing air out of the lungs.
➡️ Accessory Muscles of Breathing
These are used mainly during heavy breathing or when the body needs additional help to move air in and out of the lungs. This includes the following:
-- Sternocleidomastoid: These muscles are located on either side of the neck and help to lift the sternum and the upper ribs, further expanding the chest cavity during inspiration.
-- Scalene Muscles: Located in the neck, these muscles help to elevate the upper ribs during a deep inhalation.
-- Pectoralis Minor: This muscle, located in the chest, also assists in elevating the ribs during a forceful inhalation.
-- Abdominal Muscles: These include the rectus abdominis, transversus abdominis, and the internal and external oblique muscles.
They help in forceful expiration by compressing the abdominal cavity, which pushes the diaphragm upward, reducing the volume of the chest cavity and forcing air out of the lungs.
➡️ Other Accessory Muscles
Additional muscles, such as the serratus anterior and latissimus dorsi, may also assist in deep breathing, particularly during exercise or other activities that require increased respiration.
💥Normal Breathing [Full Guide] ➜ ➜ ➜ https://bit.ly/3OXxEU9
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:48 - Diaphragm
1:16 - Intercostal Muscles
1:55 - Accessory Muscles of Breathing
2:08 - Sternocleidomastoid
2:20 - Scalene Muscles
2:30 - Pectoralis Minor
2:38 - Abdominal Muscles
3:00 - Other Accessory Muscles
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#respirationmuscles #breathing #respiration
39
views
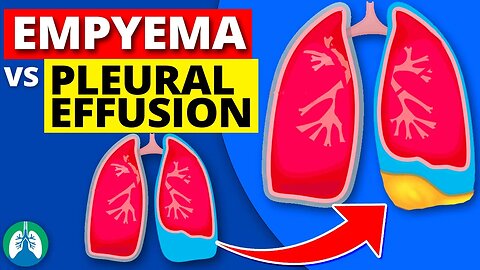
Empyema vs. Pleural Effusion *EXPLAINED*
What is the difference between an Empyema and Pleural Effusion? We created this video to explain the difference and provide a brief overview of this topic.
💥Pleural Effusion [Full Guide] ➜ ➜ ➜ https://bit.ly/3FyS2r8
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
➡️ Pleural Effusion
A pleural effusion refers to the abnormal accumulation of fluid in the pleural space. It can occur for various reasons, including heart failure, pneumonia, cancer, liver or kidney disease, and other inflammatory or infectious conditions. Pleural effusions can be classified as either transudative or exudative, based on the nature of the fluid and the underlying cause.
-- Transudative effusions occur when there is an imbalance in the production and absorption of pleural fluid, often due to increased hydrostatic pressure or decreased oncotic pressure.
-- Exudative effusions, on the other hand, result from inflammation, infection, or injury to the pleura, leading to increased capillary permeability and leakage of proteins, cells, and other solutes into the pleural space. Exudative effusions are often caused by conditions such as pneumonia, lung cancer, tuberculosis, autoimmune disorders, and pulmonary embolism.
➡️ Empyema
An empyema is a specific type of pleural effusion that involves the accumulation of pus in the pleural space due to a bacterial, fungal, or, less commonly, parasitic infection. It is often a complication of pneumonia, chest surgery, or a lung abscess. Empyema is characterized by the presence of a large number of white blood cells, dead cells, and microorganisms, leading to a thick, purulent fluid. This fluid may become loculated, forming septations or pockets that can further complicate treatment.
➡️ Diagnosis and Treatment
The diagnosis of pleural effusion and empyema typically involves a combination of medical history, physical examination, imaging studies, such as chest x-rays or CT scans, and analysis of pleural fluid obtained through thoracentesis. The distinction between the two conditions is important, as the management and treatment differ significantly. Treatment for pleural effusion depends on the underlying cause and severity. Transudative effusions often resolve with treatment of the primary condition, such as using diuretics for congestive heart failure. In contrast, exudative pleural effusions may require more invasive interventions, such as thoracentesis or chest tube placement, to drain the fluid and relieve symptoms.
➡️ Summary
Both empyema and pleural effusion involve the accumulation of fluid in the pleural space, but they have distinct causes, characteristics, and implications for treatment. Pleural effusion can be a result of various medical conditions, leading to either transudative or exudative fluid accumulation. Empyema is a specific type of pleural effusion caused by an infection, resulting in the buildup of pus within the pleural space. Proper diagnosis and distinction between these conditions are essential to ensure appropriate and effective management.
💥Pleural Effusion [Full Guide] ➜ ➜ ➜ https://bit.ly/3FyS2r8
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:32 - Pleural Effusion
0:56 - Transudative Effusions
1:23 - Exudative Effusions
1:57 - Empyema
2:35 - Diagnosis and Treatment
3:58 - Summary
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#respiratorytherapy #pleuraleffusion #empyema
95
views
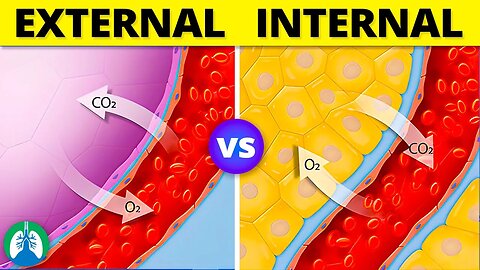
Internal vs. External Respiration *EXPLAINED* 🫁
What are internal and external respiration? We created this video to cover the medical definition and provide a brief overview of this topic.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
💥Depth of Respiration [Full Guide] ➜ ➜ ➜ https://bit.ly/3KSkTsQ
➡️ External Respiration
External respiration is the process of gas exchange between the body and the external environment. It takes place within the lungs, specifically in the tiny sacs called alveoli. During inhalation, oxygen-rich air enters the lungs, while during exhalation, carbon dioxide is removed from the body.
The primary steps that occur during external respiration include:
-- Inhalation: The diaphragm and intercostal muscles contract, increasing the volume of the thoracic cavity and reducing the pressure within. This causes air to flow into the lungs.
-- Gas exchange: In the alveoli, oxygen diffuses from the air into the blood, and carbon dioxide diffuses from the blood into the air. This occurs due to the concentration gradient between the air and blood.
-- Exhalation: The diaphragm and intercostal muscles relax, decreasing the volume of the thoracic cavity and increasing the pressure within. This forces air and carbon dioxide out of the lungs.
➡️ Internal Respiration
Internal respiration, also known as cellular respiration or tissue respiration, is the process of gas exchange between the body's cells and the blood. It occurs at the level of the capillaries, which are small blood vessels that connect the arteries and veins. The main purpose of internal respiration is to deliver oxygen to the cells for use in energy production and to remove carbon dioxide produced during cellular metabolism.
The primary steps that occur during internal respiration include:
-- Oxygen transport: Oxygen-rich blood is delivered to the body's tissues and cells via the circulatory system.
-- Gas exchange: In the capillaries, oxygen diffuses from the blood into the cells, and carbon dioxide diffuses from the cells into the blood.
-- Carbon dioxide transport: Carbon dioxide-rich blood is carried back to the lungs via the circulatory system, where it is removed from the body during external respiration.
➡️ Recap
External respiration involves the exchange of gases between the lungs and the surrounding environment, whereas internal respiration deals with the gas exchange at the cellular level within the body's tissues. Both processes are essential for maintaining proper oxygen and carbon dioxide levels and ensuring the body's cells can function efficiently.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:24 - External Respiration
0:48 - Inhalation
1:01 - Gas Exchange
1:15 - Exhalation
1:29 - Internal Respiration
2:10 - Oxygen Transport
2:16 - Gas Exchange
2:25 - Carbon Dioxide Transport
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#respiration #internalrespiration #externalrespiration
58
views
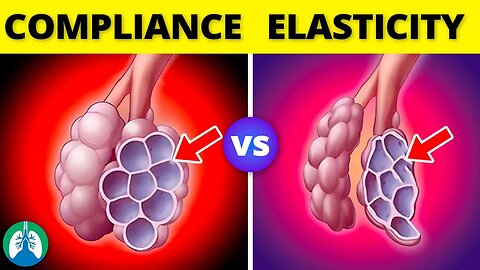
Lung Compliance vs. Elasticity *EXPLAINED*
What is the different between lung compliance and elasticity? This video breaks it down and provides an overview of this topic.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
➡️ Lung Compliance
Lung compliance refers to the ease with which the lungs can expand and contract in response to changes in pressure. Compliance is a measurement of the lung's ability to stretch. Lung compliance is influenced by several factors, including the elasticity of the lung tissue, the surface tension of the alveoli, and the resistance of the airways. A high lung compliance means that the lungs can expand and contract easily, while a low lung compliance means that the lungs are stiff and resistant to changes in pressure.
➡️ Elasticity
Elasticity, on the other hand, refers to the tendency of the lung tissue to return to its original shape after it has been stretched or compressed. Lung tissue contains elastic fibers that allow it to stretch and then recoil back to its original size and shape. Elasticity is important for maintaining lung function during the breathing cycle. Without elasticity, the lungs would not be able to expel air during exhalation and would be unable to fill with air during inhalation.
➡️ Balance
In healthy lungs, there is a balance between lung compliance and elasticity, which allows for efficient gas exchange between the air and the blood. During inhalation, the lungs expand as air flows into the lungs, and the alveoli expand to accommodate the incoming air. During exhalation, the lungs recoil as air flows out, and the alveoli shrink back to their original size. In patients with respiratory diseases, such as emphysema or pulmonary fibrosis, this balance between lung compliance and elasticity is disrupted.
➡️ Example
For example, when emphysema is present, the elastic fibers of the lung tissue are destroyed, resulting in a loss of elasticity. As a result, the lungs become overinflated and can't expel air properly during exhalation. Pulmonary fibrosis, on the other hand, is characterized by the scarring of lung tissue. This results in stiff lungs and decreased lung compliance. Lung compliance and elasticity are essential components of the respiratory system that work together to facilitate efficient gas exchange. Lung compliance refers to the ease with which the lungs can expand and contract, while elasticity refers to the ability of the lung tissue to recoil back to its original shape after being stretched. In healthy lungs, there is a balance between compliance and elasticity, but in respiratory diseases, this balance is disrupted, leading to breathing difficulties and impaired gas exchange.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
—————
📗 BEST STUDY GUIDES FOR YOU
▪ TMC Test Bank 👉 http://bit.ly/2IGeqSu
▪ Hacking the TMC Exam 👉 http://bit.ly/2XBc8do
▪ TMC Exam Bundle (Save $) 👉 https://bit.ly/34pqEsV
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
💙MORE FROM RTZ
▪ Free TMC Practice Exam 👉 http://bit.ly/2XlwASL
▪ Free RRT Cheat Sheet 👉 http://bit.ly/2IbmOKB
▪ Resources for RT's 👉 http://bit.ly/2WVV5qo
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:21 - Lung Compliance
0:55 - Elasticity
2:18 - Pulmonary Fibrosis
—————
🖼CREDIT FOR MUSIC AND GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#RespiratoryTherapy #lungcompliance #elasticity
53
views
Castor Oil | What Does the Science Say? 🧬
What is castor oil? What are the benefits? Can it have adverse effects on the body? Watch this video to find out!
💥Health Essentials [Full Guides] ➜ ➜ ➜ https://bit.ly/3BdR2pl
💥Top Castor Oil (Affiliate Link) ➜ ➜ ➜ https://amzn.to/3oArkdk
🟦 Other Videos You Might Enjoy
▪ Castor Oil Uses ➜ https://youtu.be/zBHcJBYJ6a0
▪ Most Powerful Medicinal Herbs ➜ https://youtu.be/1Uq_7Gm6zQk
▪ Ginger Secret Benefits ➜ https://youtu.be/JVaeoVDPdQ4
▪ Golden Honey Benefits ➜ https://youtu.be/JCQe12xUlvs
➡️ Indications
Castor oil is most commonly used as a stimulant laxative, offering relief in constipation and aiding in medical procedures such as colonoscopies.
➡️ Mechanism of Action
The active component in castor oil responsible for its laxative property is ricinoleic acid. Upon ingestion, lipase in the intestine breaks down castor oil into ricinoleic acid, which activates EP3 and EP4 prostanoid receptors in smooth muscle cells.
🟦 Uses of Castor Oils
Castor oil can be used for various purposes, including medicinal, cosmetic, and industrial applications. Here are some common ways to use castor oil:
🔲 Laxative
To relieve constipation, take castor oil orally as per the recommended dosage on the label or as advised by a healthcare professional. Typically, the dosage for adults is 15-60 ml (1-4 tablespoons) and should be taken on an empty stomach. It is essential to follow the guidelines, as excessive use can lead to diarrhea and other side effects. Drinking plenty of water can also help prevent dehydration.
🔲 Hair Care
Castor oil can be used to promote hair growth, strengthen hair, and alleviate dry, itchy scalp conditions. To use it on your hair, apply a small amount of castor oil directly to your scalp and massage it in gently.
🔲 Skincare
Castor oil can be applied directly to the skin to moisturize and treat various skin conditions, such as acne or dry skin. You can apply a small amount of castor oil to the affected area and massage it gently.
🔲 Eyelashes and Eyebrows
To promote the growth of eyelashes and eyebrows, apply a small amount of castor oil to a clean mascara wand or a cotton swab, and gently apply it to your lashes and brows before bedtime.
🔲 Massage Oil
Castor oil can be used for massages, particularly to address joint or muscle pain. Again, be sure to mix it with a carrier oil and apply it to the affected area, massaging it gently.
➡️ Adverse Effects
Common adverse effects of castor oil include abdominal cramping, vomiting, bloating, and dizziness. These side effects contribute to the decline in its use within conventional medicine.
➡️ Contraindications
Castor oil should be avoided during pregnancy due to its potential to induce premature contractions. Other contraindications include gastrointestinal obstruction, appendicitis, perforation, and inflammatory bowel disease.
➡️ Monitoring
Patients taking castor oil should be monitored for electrolyte disturbances and acid-base disorders, which can occur due to the loss of bicarbonate, water, and electrolytes. Healthcare professionals should also monitor for laxative abuse.
➡️ Toxicity
Castor oil itself is not toxic. It is derived from the seeds of the castor bean plant and is generally considered safe for topical and internal use when used appropriately.
💥Health Essentials [Full Guides] ➜ ➜ ➜ https://bit.ly/3BdR2pl
💥Top Castor Oil (Affiliate Link) ➜ ➜ ➜ https://amzn.to/3oArkdk
—————
💙MORE FROM RTZ
▪ Free TMC Practice Exam 👉 http://bit.ly/2XlwASL
▪ Free RRT Cheat Sheet 👉 http://bit.ly/2IbmOKB
▪ Resources for RT's 👉 http://bit.ly/2WVV5qo
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:41 - Indications
1:17 - Mechanism of Action
1:49 - Administration
1:59 - Laxative
2:34 - Hair Care
3:07 - Skincare
3:42 - Eyelashes and Eyebrows
4:01 - Massage Oil
4:27 - Adverse Effects
4:46 - Contraindications
5:07 - Monitoring
5:30 - Toxicity
—————
🖼CREDIT FOR MUSIC AND GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#castoroil #castoroilbenefits #castoroiluses
1.29K
views
Glasgow Coma Scale (GCS) *MADE EASY* 🧠
What is the Glasgow Coma Scale (GCS)? This video covers the medical definition and provides a brief overview of this topic.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
➡️Glasgow Coma Scale
The GCS is used to measure the patient's responsiveness in three areas:
1. Eye opening: The patient's ability to open their eyes spontaneously or in response to verbal or physical stimuli.
2. Verbal response: The patient's ability to speak or make sounds in response to questions or commands.
3. Motor response: The patient's ability to move in response to stimuli, such as withdrawing from painful stimuli or following simple commands.
Each of these areas is scored on a scale from 1 to 5 or 6, depending on the specific assessment method being used, with a total possible score of 15. The GCS score can help healthcare providers assess the severity of a patient's condition and determine the appropriate course of treatment.
Glasgow Coma Scale (GCS)
➡️ Eye Opening
-- Spontaneous: 4
-- To verbal stimuli: 3
-- To pain only: 2
-- No eye opening: 1
➡️ Verbal Response
-- Oriented: 5
-- Confused: 4
-- Inappropriate words: 3
-- Incomprehensible sounds: 2
-- No verbal response: 1
➡️ Motor Response
-- Obeys commands: 6
-- Movement to painful stimuli: 5
-- Withdrawal from pain: 4
-- Abnormal flexion to pain: 3
-- Abnormal extension to pain: 2
-- No motor response: 1
The lowest possible score is 3, which occurs in patients who are completely unresponsive, while the maximum score of 15 occurs in patients who are fully responsive. If the patient's score falls anywhere in the middle, you can use the score to classify the severity of their brain injury.
➡️ For example:
-- Mild: GCS 13–15
-- Moderate: GCS 9–12
-- Severe: GCS 8 or less
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
—————
📗 BEST STUDY GUIDES FOR YOU
▪ TMC Test Bank 👉 http://bit.ly/2IGeqSu
▪ Hacking the TMC Exam 👉 http://bit.ly/2XBc8do
▪ TMC Exam Bundle (Save $) 👉 https://bit.ly/34pqEsV
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
💙MORE FROM RTZ
▪ Free TMC Practice Exam 👉 http://bit.ly/2XlwASL
▪ Free RRT Cheat Sheet 👉 http://bit.ly/2IbmOKB
▪ Resources for RT's 👉 http://bit.ly/2WVV5qo
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:21 - GCS
1:19 - Eye Opening
1:45 - Verbal Response
2:08 - Motor Response
—————
🖼CREDIT FOR MUSIC AND GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#RespiratoryTherapy #RespiratoryTherapist #RespiratoryTherapySchool
32
views
Gastroesophageal Reflux Disease (GERD) *Explained*
What is Gastroesophageal Reflux Disease (GERD)? This video covers the medical definition and provides a brief overview of this topic.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
➡️ Causes
GERD occurs when the lower esophageal sphincter, a ring of muscle at the bottom of the esophagus, fails to close properly, allowing stomach acid to flow back into the esophagus.
This can be caused by a variety of factors, including:
- Obesity
- Hiatal hernia
- Pregnancy
- Connective tissue disorders
- Smoking
- Taking certain medications
- Certain foods and drinks
➡️ Symptoms
The symptoms can vary from person to person but typically include:
- Heartburn
- Regurgitation
- Difficulty swallowing
- Chronic cough
- Chest pain
➡️ Treatment
The treatment of GERD typically involves a combination of lifestyle changes, medications, and in some cases, surgery. Lifestyle changes can include losing weight, avoiding trigger foods and drinks, eating smaller meals, and avoiding lying down after meals. Medications used to treat GERD can include antacids, H2 blockers, and proton pump inhibitors (PPIs), which reduce the amount of acid produced by the stomach. In some cases, surgery may be recommended to strengthen the lower esophageal sphincter and prevent acid reflux. GERD is a common medical condition, but it can cause significant discomfort and, in some cases, serious complications. Recognizing the causes and symptoms is essential for getting the right diagnosis and treatment. With proper management, most people can experience relief from their symptoms and avoid long-term complications. If you are experiencing persistent acid reflux or related symptoms, it's important to talk to your doctor to determine the best course of treatment for you.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
—————
📗 BEST STUDY GUIDES FOR YOU
▪ TMC Test Bank 👉 http://bit.ly/2IGeqSu
▪ Hacking the TMC Exam 👉 http://bit.ly/2XBc8do
▪ TMC Exam Bundle (Save $) 👉 https://bit.ly/34pqEsV
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
💙MORE FROM RTZ
▪ Free TMC Practice Exam 👉 http://bit.ly/2XlwASL
▪ Free RRT Cheat Sheet 👉 http://bit.ly/2IbmOKB
▪ Resources for RT's 👉 http://bit.ly/2WVV5qo
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:27 - Causes
0:57 - Symptoms
1:36 - Treatment
—————
🖼CREDIT FOR MUSIC AND GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#GERD #gastroesophagealrefluxdisease #respiratorytherapyzone
32
views
Lung Pleura (Anatomy) | Pleural Cavity | Overview
What are the lung pleura? This video covers the medical definition and provides a brief overview of this topic.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
💥Pleural Diseases [Full Guide] ➜ ➜ ➜ https://bit.ly/2YEIcQE
➡️ Structure of the Pleura
-- Visceral pleura: The visceral pleura is the innermost layer and covers the surface of the lungs.
-- Parietal pleura: The parietal pleura is the outermost layer and lines the inside of the chest wall.
These two layers are separated by a small amount of pleural fluid. The visceral pleura is closely adherent to the surface of the lungs and follows all of their contours, while the parietal pleura is separated from the lungs by the pleural cavity.
➡️ Function of the Pleura
The pleura play a crucial role in the process of breathing. During inhalation, the diaphragm contracts, and the chest expands. The pleural fluid reduces friction between the layers of pleura, allowing them to slide easily over one another during a breathing cycle. Exhalation occurs passively as the diaphragm relaxes and the chest wall returns to its resting position.
➡️ Disorders of the Pleura
Disorders of the pleura can affect the function of the respiratory system and lead to serious health problems.
➡️Types:
-- Pleurisy: A condition in which the pleura become inflamed, causing chest pain and difficulty breathing.
-- Pneumothorax: A condition in which air enters the pleural cavity, causing the lung to collapse.
-- Pleural effusion: A condition in which excess fluid accumulates in the pleural cavity, putting pressure on the lungs and making it difficult to breathe.
The treatment for these conditions depends on the underlying cause. Pleurisy may be treated with anti-inflammatory medications or antibiotics, while pneumothorax may require the insertion of a chest tube to remove the air from the pleural cavity. Pleural effusion may also require drainage of the fluid with a chest tube or thoracentesis. The pleural cavity is an essential component of the respiratory system, playing a crucial role in the process of breathing.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
💥Pleural Diseases [Full Guide] ➜ ➜ ➜ https://bit.ly/2YEIcQE
—————
📗 BEST STUDY GUIDES FOR YOU
▪ TMC Test Bank 👉 http://bit.ly/2IGeqSu
▪ Hacking the TMC Exam 👉 http://bit.ly/2XBc8do
▪ TMC Exam Bundle (Save $) 👉 https://bit.ly/34pqEsV
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
💙MORE FROM RTZ
▪ Free TMC Practice Exam 👉 http://bit.ly/2XlwASL
▪ Free RRT Cheat Sheet 👉 http://bit.ly/2IbmOKB
▪ Resources for RT's 👉 http://bit.ly/2WVV5qo
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:23 - Structure of the Pleura
0:26 - Visceral Pleura
0:42 - Parietal Pleura
0:56 - Function of the Pleura
1:21 - Disorders of the Pleura
1:29 - Pleurisy
1:36 - Pneumothorax
1:44 - Pleural Effusion
—————
🖼CREDIT FOR MUSIC AND GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#lungpleura #pleuralcavity #pleura
25
views
Graham's Law of Diffusion *EXPLAINED*
What is Graham's Law of Diffusion? This video covers the medical definition and provides a brief overview of this topic.
💥Pulmonary Diffusion ➜ ➜ ➜ https://bit.ly/3bBcJ4Q
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
➡️ Diffusion
Diffusion is the process by which particles move from an area of high concentration to an area of lower concentration. This movement occurs until a state of equilibrium is reached, where the concentration of particles is the same throughout the space.
➡️ Graham's Law
According to Graham's Law, the rate of diffusion of a gas is inversely proportional to the square root of its molecular weight. In other words, the lighter the gas molecule, the faster it will diffuse or effuse through a membrane. The solubility coefficient of a gas also plays a role in its diffusion rate. This is a measure of how easily a gas dissolves in a liquid. The more soluble a gas is, the slower it will diffuse. This is because the gas molecules are more likely to dissolve in the liquid rather than move through a membrane.
➡️ Formula
Mathematically, Graham's Law can be expressed as follows:
- Rate1 is the rate of diffusion for gas 1.
- Rate2 is the rate of diffusion for gas 2.
- M1 is the molar mass of gas 1
- M2 is the molar mass of gas 2.
This equation shows that the rate of diffusion is inversely proportional to the square root of the molecular weight. So, if two gases have the same solubility coefficient, the lighter gas will diffuse faster than the heavier gas. However, if two gases have the same molecular weight, their diffusion rates will be the same regardless of their solubility coefficients.
➡️ Conditions
It's important to note that Graham's Law is based on ideal conditions, which assume that the gas molecules are non-interacting and that there are no temperature or pressure differences between the two sides of the membrane. In reality, there are many factors that can affect the diffusion rate of a gas, such as temperature, pressure, and the presence of other molecules. Despite its limitations, Graham's Law remains a useful tool for understanding the diffusion of gases. It has applications in many areas of science, such as in the study of atmospheric chemistry, the behavior of gases in the human body, and the diffusion of gases in industrial processes. It's a simple yet powerful concept that helps us understand the behavior of gases in a wide range of contexts.
💥Pulmonary Diffusion ➜ ➜ ➜ https://bit.ly/3bBcJ4Q
—————
📗 BEST STUDY GUIDES FOR YOU
▪ TMC Test Bank 👉 http://bit.ly/2IGeqSu
▪ Hacking the TMC Exam 👉 http://bit.ly/2XBc8do
▪ TMC Exam Bundle (Save $) 👉 https://bit.ly/34pqEsV
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
💙MORE FROM RTZ
▪ Free TMC Practice Exam 👉 http://bit.ly/2XlwASL
▪ Free RRT Cheat Sheet 👉 http://bit.ly/2IbmOKB
▪ Resources for RT's 👉 http://bit.ly/2WVV5qo
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:28 - Diffusion
1:21 - Graham's Law as Tool
—————
🖼CREDIT FOR MUSIC AND GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#RespiratoryTherapy #GrahamsLaw #RespiratoryTherapySchool
13
views
Indirect Calorimetry (Medical Definition) | Quick Explainer Video
What is indirect calorimetry? This video covers the medical definition and provides a brief overview of this topic.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
➡️ Indirect Calorimetry
Indirect calorimetry is typically performed using a specialized machine called a metabolic cart, which measures the concentration of oxygen and carbon dioxide during a breathing cycle. This information is then used to calculate the individual's metabolic rate, which can be expressed in terms of calories or joules per unit of time. It looks at the patient's resting energy expenditure (REE) to figure out how much to feed the patient and the respiratory quotient (RQ) to validate the results. These calculations involve formulas, but we're not going to cover that in this brief video.
➡️ Importance in Healthcare
Indirect calorimetry is important for determining how much to feed patients in the healthcare setting because it provides a direct measurement of their metabolic rate, which is a key factor in determining their energy needs. By measuring the amount of oxygen consumed and carbon dioxide produced, indirect calorimetry can provide an accurate estimate of the patient's energy expenditure, which can then be used to calculate their caloric needs.
➡️ Reasons
If a patient is not receiving enough calories, they may become malnourished, which can lead to a variety of negative health outcomes, including muscle wasting, immune dysfunction, impaired wound healing, and prolonged hospital stays. On the other hand, if a patient is receiving too many calories, they may become overweight or obese, which can increase their risk of developing a variety of chronic diseases, such as diabetes, heart disease, and cancer. Indirect calorimetry is an important tool for healthcare professionals in determining the optimal nutrition therapy for their patients. By providing a direct measurement of the patient's energy needs, it allows healthcare professionals to individualize their nutrition therapy and optimize patient outcomes.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
—————
📗 BEST STUDY GUIDES FOR YOU
▪ TMC Test Bank 👉 http://bit.ly/2IGeqSu
▪ Hacking the TMC Exam 👉 http://bit.ly/2XBc8do
▪ TMC Exam Bundle (Save $) 👉 https://bit.ly/34pqEsV
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
💙MORE FROM RTZ
▪ Free TMC Practice Exam 👉 http://bit.ly/2XlwASL
▪ Free RRT Cheat Sheet 👉 http://bit.ly/2IbmOKB
▪ Resources for RT's 👉 http://bit.ly/2WVV5qo
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:44 - Indirect Calorimetry
1:24 - Importance
—————
🖼CREDIT FOR MUSIC AND GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#RespiratoryTherapy #IndirectCalorimetry #RespiratoryTherapySchool
19
views
Kyphoscoliosis (Medical Definition) | Quick Explainer Video
What is Kyphoscoliosis? This video covers the medical definition and provides a brief overview of this topic.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
➡️ What is Kyphoscoliosis?
Kyphoscoliosis can occur at any age, and approximately 80% of cases are idiopathic, meaning there is no known cause. However, it is believed to be caused by prolonged bad posture, degenerative diseases, neuromuscular diseases, connective tissue diseases, tuberculosis, or congenital factors.
➡️ Symptoms
The symptoms of kyphoscoliosis may vary, ranging from a slouch or abnormal hunch to negative effects on the lungs, heart, and muscles of respiration. In severe cases, it can result in symptoms such as disfigurement, back pain, paralysis, respiratory failure, and neurological issues.
➡️ Treatment
The treatment methods for kyphoscoliosis depend on the severity of the condition and include noninvasive options such as checkups, scoliosis bracing, pain management, and physical therapy, as well as surgical options such as spinal fusion or the installation of an adjustable rod.
➡️ Complications
Complications may arise, and the outlook depends on early detection and treatment. Living with kyphoscoliosis can be challenging; however, the symptoms can usually be managed with appropriate medical treatment. If you suspect that you or a loved one may have kyphoscoliosis, it's important to seek medical attention. A doctor can perform a physical examination, imaging tests, and other diagnostic tests to determine the extent and severity of the condition.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
—————
📗 BEST STUDY GUIDES FOR YOU
▪ TMC Test Bank 👉 http://bit.ly/2IGeqSu
▪ Hacking the TMC Exam 👉 http://bit.ly/2XBc8do
▪ TMC Exam Bundle (Save $) 👉 https://bit.ly/34pqEsV
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
💙MORE FROM RTZ
▪ Free TMC Practice Exam 👉 http://bit.ly/2XlwASL
▪ Free RRT Cheat Sheet 👉 http://bit.ly/2IbmOKB
▪ Resources for RT's 👉 http://bit.ly/2WVV5qo
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:31 - Kyphoscoliosis
0:52 - Symptoms
1:12 - Treatment
—————
🖼CREDIT FOR MUSIC AND GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#RespiratoryTherapy #RespiratoryTherapist #Kyphoscoliosis
26
views
Wet Drowning vs. Dry Drowning *Explained*
What is the science behind drowning? What is the difference between wet drowning and dry drowning? Watch this video to find out!
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
💥Respiratory Management of Drowning [Glossary] ➜ ➜ ➜ https://bit.ly/3dzDmZ2
➡️ Wet vs. Dry Drowning
The inhalation of water initiates the cough response, which results in fluid being either inhaled or swallowed. This can result in laryngospasm with closure of the glottis, which prevents the aspiration of fluid into the lungs. This is known as dry drowning because the glottic closure stops water from entering the lungs. Wet drowning occurs when fluid is aspirated into the lungs. Water submersion can result in unconsciousness, which lessens the amount of laryngospasm. Therefore, water is able to enter the lungs. The causes of drowning are usually accidental and preventable and occur more often in children than adults. Drowning in adults is often related to alcohol consumption, trauma, or medical emergencies.
➡️ Treatment
The treatment of a near-drowning patient requires immediate intervention to establish an airway, ensure breathing, and promote circulation. This means that cardiopulmonary resuscitation (CPR) with rescue breaths and chest compressions must be initiated as quickly as possible to increase the chances of survival. The patient should also be placed in the prone position because it's the best for clearing water from the airways of the lungs. Body temperature is another important consideration, especially if the victim was submerged in cold water. In this case, they may require body temperature control techniques to limit or prevent hypothermia. Near-drowning patients almost always develop ARDS. It's a respiratory disorder characterized by fluid in the alveoli. It causes refractory hypoxemia, decreased lung compliance, and severe oxygen insufficiency. Patients with ARDS often require treatment with mechanical ventilation and high levels of PEEP.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
💥Respiratory Management of Drowning [Glossary] ➜ ➜ ➜ https://bit.ly/3dzDmZ2
—————
📗 BEST STUDY GUIDES FOR YOU
▪ TMC Test Bank 👉 http://bit.ly/2IGeqSu
▪ Hacking the TMC Exam 👉 http://bit.ly/2XBc8do
▪ TMC Exam Bundle (Save $) 👉 https://bit.ly/34pqEsV
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
💙MORE FROM RTZ
▪ Free TMC Practice Exam 👉 http://bit.ly/2XlwASL
▪ Free RRT Cheat Sheet 👉 http://bit.ly/2IbmOKB
▪ Resources for RT's 👉 http://bit.ly/2WVV5qo
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:19 - Dry Drowning
0:44 - Wet Drowning
1:23 - Treatment
—————
🖼CREDIT FOR MUSIC AND GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#Drowning #Wetdrowning #Drydrowning
352
views
1
comment
Gasping *Explained* | Abnormal Breathing Pattern
What is gasping? This video covers the medical definition and provides a brief overview of this abnormal breathing pattern.
💥Abnormal Breathing Patterns [Full Guide] ➜ ➜ ➜ http://bit.ly/2pZP7VG
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
➡️ Gasping
Gasping is a type of labored breathing with sudden, forced inspirations that often indicates shortness of breath or dyspnea. It's an abnormal breathing pattern that can be a symptom of a wide range of underlying medical conditions.
➡️ Breathing Patterns Associated with Gasping
1. Apneustic breathing
2. Agonal breathing
➡️ Apneustic Breathing
Apneustic breathing is an abnormal respiratory pattern characterized by a deep and gasping inspiration with a pause at full inspiration, followed by a brief, partial expiration. This pattern is often seen in patients who’ve experienced severe brain damage to the upper medulla or pons caused by a stroke or trauma. It is also seen in patients with a hypoglycemic coma or those with profound hypoxemia. Apneustic breathing is caused by basilar artery occlusion and usually has a poor prognosis.
➡️ Agonal Breathing
Agonal breathing is an abnormal respiratory pattern characterized by intermittent gasping and labored breathing. It is caused by a preterminal brainstem reflex and eventually progresses to complete apnea. This breathing pattern often occurs during the final breaths before death.
Some of the most common causes of agonal breathing include:
- Cerebral ischemia
- Extreme hypoxemia
- Anoxia
Agonal breathing may also occur during cardiac arrest or cardiogenic shock, where labored respirations may persist after the cessation of the patient’s heartbeat. This type of respiration occurs in approximately 40% of cardiac arrest cases that take place outside of the hospital setting. The treatment for agonal breathing is focused on resuscitation and support. Gasping can be frightening and uncomfortable for the person experiencing it. Therefore, identifying the underlying cause and seeking proper medical care is essential in managing this symptom.
💥Abnormal Breathing Patterns [Full Guide] ➜ ➜ ➜ http://bit.ly/2pZP7VG
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
—————
📗 BEST STUDY GUIDES FOR YOU
▪ TMC Test Bank 👉 http://bit.ly/2IGeqSu
▪ Hacking the TMC Exam 👉 http://bit.ly/2XBc8do
▪ TMC Exam Bundle (Save $) 👉 https://bit.ly/34pqEsV
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
💙MORE FROM RTZ
▪ Free TMC Practice Exam 👉 http://bit.ly/2XlwASL
▪ Free RRT Cheat Sheet 👉 http://bit.ly/2IbmOKB
▪ Resources for RT's 👉 http://bit.ly/2WVV5qo
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:23 - Gasping
0:40 - Apneustic Breathing
1:16 - Agonal Breathing
—————
🖼CREDIT FOR MUSIC AND GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#gasping #respiratorypatterns #breathingpatterns
48
views