Synapse Orthopedic Group | Doctors You Can Trust
Meet Ann Parkes.
She has been a patient of Edwin Haronian MD for a couple years due to a work related injury. Under Doctor Haronian's care she has made great improvements. She tells us she has 3 masters degrees, is a registered nurse and public health nurse. This knowledge and experience had made her more observant of Synapse Orthopedic Group. She confidently says this is an extremely professional and knowledgeable office. She is so glad to be a patient here and wants to continue seeing Doctor Haronian.
Call us to schedule an appointment: (818) 788-2400
Locations in Pomona, Sherman Oaks, and Los Angeles
Spinal surgeons have concluded that neurological deficit such as motor weakness or sensory loss is caused by neural compression. However, pain is produced only after the mechanical compression on the nerve has produced inflammation around the nerve. In turn, the inflammation causes swelling of the nerve which causes relative decrease in the space available for the nerve and the process continues and worsens. Since the inflammatory reaction is the basic underlying process, its blockade is of primary concern for the patient and the treating spinal surgeon. This process is begun by prescription of oral anti-inflammatory medications such as Motrin, Naprosyn, or the newer COX-2 inhibitors such as Vioxx and Celebrex. More powerful medications include the oral steroids which are used in more sever cases of inflammation and pain. In cases which oral medication has not produced the desire effect, your surgeon has the ability to deliver steroidal medication directly to the area of inflammation with an Epidural Steroid Injection. The 2 areas of the spine that steroid injections are placed are the cervical (neck) and lumbar (low back) area. Please refer to these pages for more specific information.
Routinely 3 injections are performed one week apart to produce maximal results. They are done in a procedure room under live X-ray guidance (Fluoroscopy) which guides the injection needle precisely to the are in question. Some physicians still make injections without fluoroscopy guidance but it has been shown that fluoroscopic guided injections produce consistent superior results. The skin is anesthetized with a numbing medication by utilizing a very small needle. Then a slightly larger needle is placed and advanced until it reaches the area of inflammation around the spinal cord. Care is taken not to penetrate the envelope surround the spinal cord. At that time a dye (fluid that can be seen under X-ray) is injected to confirm the position of the needle. If the position is confirmed to be satisfactory the steroidal medication is then injected in the area. Frequently patients will complain of increased pain for one day after the injection due to the placement of the needle.
The concentration of the medication has been measured previously and last for about 2 weeks in the area. Even though the medication is absorbed by the body, its effects can remain up to one year. Some patient benefit greatly from these medication and the symptoms may never recur. Approximately 50% of patients benefit from these injections. Patients with Herniated discs, Spinal Stenosis, degenerative disc disease, and Spondylolisthesis may benefit from these injections. The effects of steroids are twofold. First it may reduce the inflammation directly, secondly it may reduce the symptoms to a point that will allow the patient to progress more efficiently in a rehabilitation program.
Even though most surgeons agree regarding the benefits of Epidural Steroid Injections, no research studies have concluded the most efficient program in regards to frequency of injection (the number of injections, and the time between each injections. It has been accepted in the medical community that 3 injections are acceptable within one year. However, this regime could be tailored according to patient’s response.
For more information please visit our website at: http://www.synapsedoctor.com
You can also follow our social media pages at:
http://www.facebook.com/synapsedoctor
http://www.instagram.com/synapsedoctor
http://www.twitter.com/synapsedoctor
87
views
Carpal Tunnel Patient is Left Scar less After Surgery
Meet Evelyn.
She has been a patient of Synapse Orthopedic Group for a couple years. She has been treated with injections and surgery performed by Edwin Haronian MD. She is extremely happy with her Carpal Tunnel Surgery, her hand is fully functional again.
Call us to schedule an appointment: (818) 788-2400
Locations in Pomona, Sherman Oaks, and Los Angeles
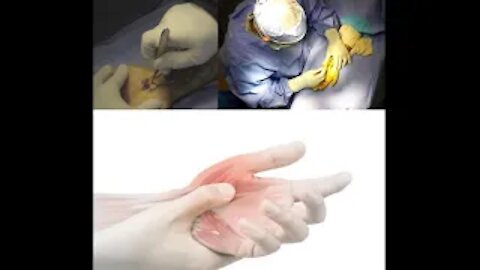
Carpal tunnel syndrome is a common condition that causes pain, numbness, and tingling in the hand and arm. The condition occurs when one of the major nerves to the hand — the median nerve — is squeezed or compressed as it travels through the wrist.
In most patients, carpal tunnel syndrome gets worse over time, so early diagnosis and treatment are important. Early on, symptoms can often be relieved with simple measures like wearing a wrist splint or avoiding certain activities.
If pressure on the median nerve continues, however, it can lead to nerve damage and worsening symptoms. To prevent permanent damage, surgery to take pressure off the median nerve may be recommended for some patients.
During open carpal tunnel release surgery , the transverse carpal ligament is cut, which releases pressure on the median nerve and relieves the symptoms of carpal tunnel syndrome. An incision is made at the base of the palm of the hand. This allows the doctor to see the transverse carpal ligament.
For more information please visit our website at: http://www.synapsedoctor.com
You can also follow our social media pages at:
http://www.facebook.com/synapsedoctor
http://www.instagram.com/synapsedoctor
http://www.twitter.com/synapsedoctor
24
views
Non-Surgical Patient Able to Return to Work
Meet Reggie.
He suffered from 2 work related injuries and has since been visiting Edwin Haronian MD at Synapse Orthopedic Group. Doctor Haronian has been able to minimize the pain from these work injuries and get Reggie back to work without having to turn to surgery.
Lets wish Reggie the best during his recovery.
Call us to schedule an appointment: (818) 788-2400
Locations in Pomona, Sherman Oaks, and Los Angeles
For more information please visit our website at: http://www.synapsedoctor.com
You can also follow our social media pages at:
http://www.facebook.com/synapsedoctor
http://www.instagram.com/synapsedoctor
http://www.twitter.com/synapsedoctor
3
views
Shoulder Surgery Patient Experience
Meet Janet.
Janet came to Edwin Haronian because she injured her back, knee and shoulder. So far, she's had a should surgery performed by Edwin Haronian MD and she has recovered greatly. She is extremely happy to come to Synapse Orthopedic Group because the care she's received from both the staff and Doctor has been wonderful.
Call us to schedule an appointment: (818) 788-2400
Locations in Pomona, Sherman Oaks, and Los Angeles
For more information please visit our website at: http://www.synapsedoctor.com
You can also follow our social media pages at:
http://www.facebook.com/synapsedoctor
http://www.instagram.com/synapsedoctor
http://www.twitter.com/synapsedoctor
4
views
Patient Experiences Loss of Feeling from Neck to Hands
Meet Ruth.
Ruth has been under the care of Edwin Haronian MD since her work-related injury occurred. Due to heavy typing she has lost sensitivity of her neck, arm, wrists and hands. She is very happy with the care she has been receiving here at Synapse Orthopedic Group and recommends it to anyone who is dealing with the same injury that she has.
Call us to schedule an appointment: (818) 788-2400
Locations in Pomona, Sherman Oaks, and Los Angeles
For more information please visit our website at: http://www.synapsedoctor.com
You can also follow our social media pages at:
http://www.facebook.com/synapsedoctor
http://www.instagram.com/synapsedoctor
http://www.twitter.com/synapsedoctor
3
views
Non-Surgical Treated Patient
Meet Will.
He has been coming to see Edwin Haronian MD at Synapse Orthopedic Group for about a year. He really likes the staff and how he is treated at Synapse Orthopedic Group. He is in the process of having his right shoulder and right elbow treated, do due an injury he was involved in.
He is in the process of getting better with physical therapy and proper medication to rid his pain. We wish him the best during his recovery.
For more information please visit our website at: http://www.synapsedoctor.com
You can also follow our social media pages at:
http://www.facebook.com/synapsedoctor
http://www.instagram.com/synapsedoctor
http://www.twitter.com/synapsedoctor
1
view
Jonathan Nassos MD Makes Patients Comfortable
Meet Gerard.
He recently switched over to Dr. Nassos for an injury he suffered from. He was not happy with his previous Doctor which led him to Synapse Orthopedic Group. Since the switch, he is really happy with how he has been treated here. We look forward to Gerard's recovery.
Call us to schedule an appointment: (818) 788-2400
Locations in Pomona, Sherman Oaks, and Los Angeles
Dr. Jonathan Nassos is a board-certified, fellowship-trained orthopaedic surgeon who specializes in the surgical and non-surgical treatment of musculoskeletal disorders and injuries, including arthroscopic surgery, joint replacement, and orthopaedic trauma. He greatly values the individual needs of each patient and is dedicated to prove the highest quality of care for his patients. He received his bachelor’s degree from the University of Illinois at Urbana-Champaign, his M.D. from Loyola University Chicago Stritch School of Medicine, and completed his residency in orthopaedic surgery at Loyola University Medical Center.
Following residency, he completed an orthopaedic sports medicine fellowship at a prestigious Kerlan-Jobe Orthopaedic Clinic in Los Angeles, California. During that time , he worked as an assistant team physician for the Los Angeles Lakers, Dodgers, Kings, Sparks, Anaheim Ducks, and Loyola Marymount University. He is active in research which he has been presented both at national and international scientific meetings. He is currently an Associate Master Instructor of Arthroscopy for the Arthroscopy Association of North America, teaching other orthopaedic surgeons about cutting-edge arthroscopic surgical procedures. He is a Fellow of the American Academy of Orthopaedic Surgeons. Dr. Nassos lives in Los Angeles with his wife Jenni, daughter, and two dogs. His hobbies include running, basketball, and golf.
For more information please visit our website at:
http://www.drnassos.com/
http://www.synapsedoctor.com
You can also follow our social media pages at:
http://www.facebook.com/synapsemedicalgroup
http://www.instagram.com/synapsedoctor
http://www.twitter.com/synapsedoctor
20
views
Cervical Spinal Fusion Surgery Patient Experience
Meet Douglas Deleon.
He was recently operated on his neck by Edwin Haronian MD. He underwent a Cervical Spinal Fusion and is currently recovering. He tells us he is so happy he's been in the care and in the hands of Doctor Haronian and the staff at Synapse Orthopedic Group.
Call us to schedule an appointment: (818) 788-2400
Locations in Pomona, Sherman Oaks, and Los Angeles
For more information please visit our website at: http://www.synapsedoctor.com
You can also follow our social media pages at:
http://www.facebook.com/synapsedoctor
http://www.instagram.com/synapsedoctor
http://www.twitter.com/synapsedoctor
2
views
Knee Arthroscopy for Patient Who Falls 15 Stairs
Meet Kelli.
Kelli was injured at work, she fell down a flight of 15 stairs. She injured her knee and had been suffering from excruciating pain since. She underwent a knee surgery performed by Edwin Haronian MD and Pain Management treatment with Jonathan Kohan MD. She has made enormous improvements under the care of Synapse Orthopedic Group and is back at Work.
Call us to schedule an appointment: (818) 788-2400
Locations in Pomona, Sherman Oaks, and Los Angeles
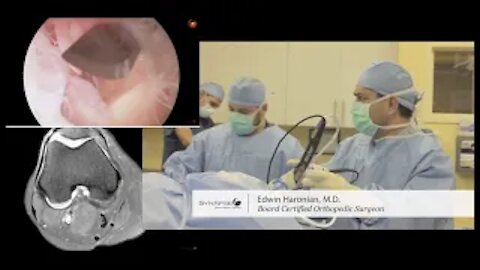
Knee arthroscopy is surgery that uses a tiny camera to look inside your knee. Small cuts are made to insert the camera and small surgical tools into your knee for the procedure.
Three different types of pain relief (anesthesia) may be used for knee arthroscopy surgery:
Local anesthesia. Your knee may be numbed with pain medicine. You may also be given medicines that relax you. You will stay awake.
Spinal anesthesia. This is also called regional anesthesia. The pain medicine is injected into a space in your spine. You will be awake but will not be able to feel anything below your waist.
General anesthesia. You will be asleep and pain-free.
Femoral nerve block. This is another type of regional anesthesia. The pain medicine is injected around the nerve in your groin. You will be asleep during the operation. This type of anesthesia will block out pain so that you need less general anesthesia.
A cuff-like device may be put around your thigh to help control bleeding during the procedure.
The surgeon will make two or three small cuts around your knee. Salt water (saline) will be pumped into your knee to inflate the knee.
A narrow tube with a tiny camera on the end will be inserted through one of the cuts. The camera is attached to a video monitor that lets the surgeon see inside the knee.
The surgeon may put other small surgery tools inside your knee through the other cuts. The surgeon will then fix or remove the problem in your knee.
At the end of your surgery, the saline will be drained from your knee. The surgeon will close your cuts with sutures (stitches) and cover them with a dressing. Many surgeons take pictures of the procedure from the video monitor, You may be able to view these pictures after the operation so that you can see what was done.
Arthroscopy may be recommended for these knee problems:
Torn meniscus. Meniscus is cartilage that cushions the space between the bones in the knee. Surgery is done to repair or remove it.
Torn or damaged anterior cruciate ligament (ACL) or posterior cruciate ligament (PCL). Torn or damaged collateral ligament
Swollen (inflamed) or damaged lining of the joint. This lining is called the synovium. Kneecap (patella) that is out of position (misalignment). Small pieces of broken cartilage in the knee joint
Removal of Baker's cyst. This is a swelling behind the knee that is filled with fluid. Sometimes the problem occurs when there is swelling and pain (inflammation) from other causes, like arthritis.
Repair of defect in cartilage. Some fractures of the bones of the knee.
Before the Procedure
Always tell your health care provider what medicines you are taking, even drugs, supplements, or herbs you bought without a prescription.
During the 2 weeks before your surgery:
You may be told to stop taking medicines that make it harder for your blood to clot. These include aspirin, ibuprofen (Advil, Motrin), naproxen (Naprosyn, Aleve), and other blood thinners.
Ask which medicines you should still take on the day of your surgery.
Tell your provider if you have been drinking a lot of alcohol (more than 1 or 2 drinks a day).
If you smoke, try to stop. Ask your provider for help. Smoking can slow down wound and bone healing. Always let your doctor know about any cold, flu, fever, herpes breakout, or other illness you have before your surgery.
On the day of your surgery:
You will most often be asked not to drink or eat anything for 6 to 12 hours before the procedure.
Take the medicines you been told you to take with a small sip of water.
You will be told when to arrive at the hospital.
After the Procedure:
You will have an ace bandage on your knee over the dressing. Most people go home the same day they have surgery. Your provider will give you exercises to do.
For more information please visit our website at: http://www.synapsedoctor.com
You can also follow our social media pages at:
http://www.facebook.com/synapsedoctor
http://www.instagram.com/synapsedoctor
http://www.twitter.com/synapsedoctor
102
views
A Week After Carpal Tunnel Surgery
Meet Michelle.
Michelle is a patient of Edwin Haronian MD. She came to Synapse Orthopedic Group unable to use her hand and arm due to Carpal Tunnel Syndrome. Doctor Haronian performed carpal tunnel release surgery on her and after 5 days she is beginning to feel sensitivity in her fingers. Thanks to Doctor Haronian and the Synapse Orthopedic Group staff she is doing much better and is in the process of recovering.
Call us to schedule an appointment: (818) 788-2400
Locations in Pomona, Sherman Oaks, and Los Angeles
For more information please visit our website at: http://www.synapsedoctor.com
You can also follow our social media pages at:
http://www.facebook.com/synapsedoctor
http://www.instagram.com/synapsedoctor
http://www.twitter.com/synapsedoctor
3
views
Patient Feels No Pain After Shoulder Surgery
Meet Rosa.
Rosa fractured her elbow and was operated by Edwin Haronian MD from Synapse Orthopedic Group. She is extremely happy with the outcome of her surgery and is astonished that she feels no pain. She is still on the road to recovery, we are wishing her well.
Call us to schedule an appointment: (818) 788-2400
Locations in Pomona, Sherman Oaks, and Los Angeles
For more information please visit our website at: http://www.synapsedoctor.com
You can also follow our social media pages at:
http://www.facebook.com/synapsedoctor
http://www.instagram.com/synapsedoctor
http://www.twitter.com/synapsedoctor
1
view
Double Carpal Tunnel Release Surgery Patient Experience
Meet Grace.
She is a patient of Edwin Haronian MD and had carpal tunnel release surgery on both of her hands. Grace has healed beautifully and she is now able to use her hands again. Before her surgery, she couldn't even use her computer due to the pain she had from her injury. Thanks to Dr. Haronian, she is able to create arts and crafts and she is extremely happy with all the treatment she's received from Synapse Orthopedic Group.
Lets wish Grace the best.
Call us to schedule an appointment: (818) 788-2400
Locations in Pomona, Sherman Oaks, and Los Angeles
For more information please visit our website at: http://www.synapsedoctor.com
You can also follow our social media pages at:
http://www.facebook.com/synapsedoctor
http://www.instagram.com/synapsedoctor
http://www.twitter.com/synapsedoctor
1
view
Torn Meniscus Patient and Surgery Recovery
Meet Shirley.
Shirley came to Synapse Orthopedic Group with and was diagnosed with fractured hand and a torn meniscus. Edwin Haronian MD performed knee surgery on Shirley and since then everyday she is getting better.
Call us to schedule an appointment: (818) 788-2400
Locations in Pomona, Sherman Oaks, and Los Angeles
For more information please visit our website at: http://www.synapsedoctor.com
You can also follow our social media pages at:
http://www.facebook.com/synapsedoctor
http://www.instagram.com/synapsedoctor
http://www.twitter.com/synapsedoctor
6
views
Update | 2 Weeks After Lumbar Fusion Surgery
Meet Tony.
Tony is a patient at Synapse Orthopedic Group. He had suffered from a work-related injury leaving him with 5 herniated discs in his neck and lower back, in addition to other injuries.
We first spoke to Tony two months, prior to surgery, he expressed how comfortable he felt going into surgery with Edwin Haronian MD as his surgeon.
This is now two months later, and Tony is visibly much better and excited about his recovery.
Call us to schedule an appointment: (818) 788-2400
Locations in Pomona, Sherman Oaks, and Los Angeles
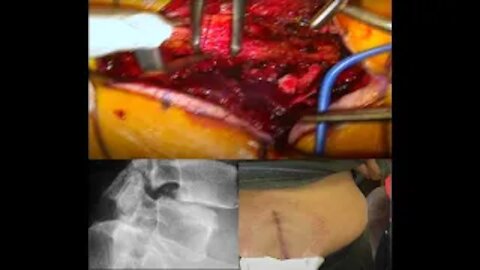
Spinal fusion, also called spondylodesis or spondylosyndesis, is a neurosurgical or orthopedic surgical technique that joins two or more vertebrae. Surgeons use supplementary bone tissue—either from the patient (autograft) or a donor (allograft)—or artificial bone substitutes in conjunction with the body's natural bone growth (osteoblastic) processes to fuse two or more adjoining vertebrae.
Spinal fusion treats a variety of pathological conditions to eliminate abnormal motion of the vertebrae that causes pain, neurological deficit, or spinal deformity. Common conditions incorporating spinal fusion in their surgical treatment are spinal stenosis, spondylolisthesis, cervical discopathy, spinal fractures, scoliosis, and kyphosis.
For more information please visit our website at: http://www.synapsedoctor.com
You can also follow our social media pages at:
https://www.facebook.com/synapsedoctor
http://www.instagram.com/synapsedoctor
http://www.twitter.com/synapsedoctor
16
views
Cervical Discectomy and Fusion by Edwin Haronian MD
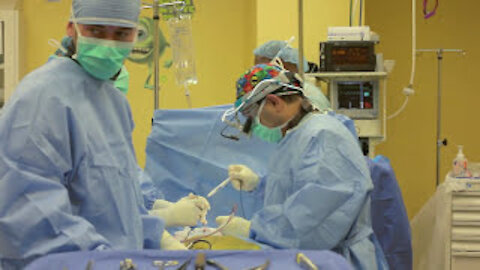
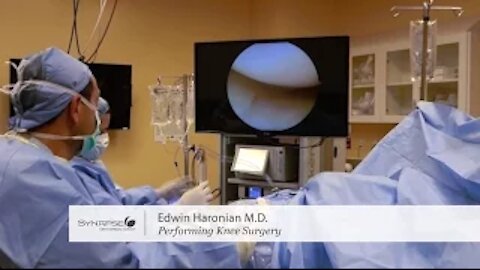
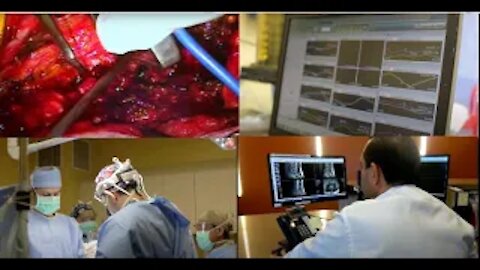
Synapse Orthopedic Group's Dr. Edwin Haronian performs a Cervical Discectomy and Fusion. This video will take you through each step from opening up the skin to skin closure and after in the recovery room. It is a detailed approach to how Dr. Haronian performs a Cervical Discectomy and Fusion.
If you are dealing with neck, back, or other chronic pain, please give us a call at (818) 788-2400. We will put you in touch with a specialist dedicated to providing you the correct diagnosis.
For more information please visit our website at: http://www.synapsedoctor.com
Anterior cervical discectomy and fusion (ACDF) is a surgical procedure to treat nerve root or spinal cord compression by decompressing the spinal cord and nerve roots of the cervical spine with a discectomy in order to stabilize the corresponding vertebrae. This procedure is used when other non-surgical treatments have failed.
The neurosurgeon or orthopedic surgeon enters the space between two discs through a small incision in front (= anterior) of and at the right or left side of the neck. The disc is completely removed, as well as arthritic bone spurs. The disc material, pressing on the spinal nerve or spinal cord, is then completely removed. The intervertebral foramen, the bone channel through which the spinal nerve runs, is then enlarged with a drill giving the nerve more room to exit the spinal canal.
To prevent the vertebrae from collapsing and to increase stability, the open space is often filled with bone graft, taken from the pelvis or cadaveric bone. The slow process of the bone graft joining the vertebrae together is called "fusion". Sometimes a titanium plate is screwed on the vertebrae or screws are used between the vertebrae to increase stability during fusion, especially when there is more than one disc involved.
The surgery requires a short stay in the clinic (1 to 3 days) and a gradual recovery between 1 and 6 weeks. However, the technology has advanced and it can be performed by 'Endoscopic Micro Discectomy" with the patient able to continue their normal life in two days. The patient may be advised to wear a neck brace or collar (for up to 8 weeks) that serves to ensure proper spinal alignment. Wearing the brace heightens one's awareness of posture and positioning and helps prevent movements (e.g., sudden and/or excessive bending or twisting of the neck) that may aggravate or slow down the healing process. It is especially advisable to wear a protective neck brace when traveling (e.g., by car), sleeping, showering, or any other activities in which the patient may not be able to be ensure proper spinal alignment. In addition, physical therapy and related healing modalities (e.g., massage, acupuncture) may be recommended in order to promote proper healing, as well as to strengthen the surrounding muscles that can take over the neck brace's 'job' of ensuring proper spinal alignment when the patient starts (around 4 to 6 weeks after surgery) to wean off the neck brace.
You can follow our social media pages at:
https://www.facebook.com/synapsedoctor
http://www.twitter.com/synapsedoctor
http://www.instagram.com/synapsedoctor
65
views
Knee Surgery Patient Experience
Meet Ruben.
Ruben came to Edwin Haronian MD after injuring his knee where he performed knee surgery for the injury. Post-op, he has been recovering quickly and looks forward to future therapy at Synapse Orthopedic Group. Lets wish Ruben a great recovery.
Call us to schedule an appointment: (818) 788-2400
Locations in Pomona, Sherman Oaks, and Los Angeles
For more information please visit our website at: http://www.synapsedoctor.com
You can also follow our social media pages at:
http://www.facebook.com/synapsedoctor
http://www.instagram.com/synapsedoctor
http://www.twitter.com/synapsedoctor
1
view
Edwin Haronian MD Patient Testimonial 2015 Recap
Happy New Year from everyone at Synapse Orthopedic Group.
We wish you all the best in your 2016 year and we look forward to providing excellent care to each and every one of our patients. We would like to thank the patients who participated. Your thoughts are important to us.
Call us to schedule an appointment: (818) 788-2400
Locations in Pomona, Sherman Oaks, and Los Angeles
For more information please visit our website at: http://www.synapsedoctor.com
You can also follow our social media pages at:
http://www.facebook.com/synapsedoctor
http://www.instagram.com/synapsedoctor
http://www.twitter.com/synapsedoctor
1
view
Lumbar Fusion to Treat 2 Ruptured Discs
Meet Thelma.
Thelma suffered from two ruptured discs. Synapse Orthopedic Group's Edwin Haronian MD performed a lumbar fusion surgery on her. Post-op, she has improved greatly she is finally able to feel her toes again and walk comfortably. She now has her life back and feels blessed that Doctor Haronian took great care of her.
Call us to schedule an appointment: (818) 788-2400
Locations in Pomona, Sherman Oaks, and Los Angeles
One of the most common procedures performed in spine surgery is lumbar fusion. Many disease processes affect the spine as a result of the motion that occurs between each bony segment. In the normal spine, each segment has 6 different motion directions (6 degrees of motion) and when there is dysfunction, pain is produces which leads to dysfunction. The primary structure allowing this motion is the inter vertebral disc. The bio-mechanical structure of the disc is so complicated that current medical technology can not duplicate the disc and it can not be replaced by any synthetic material. For this reason, the most reliable replacement is placement of bone in place of the disc which fuses the segments and eliminates the motion at that segment which will ultimately resolve the pain. The downfall of fusion is loss of motion in that segment (which may be very small for each fused level) and increased stress in the adjacent levels. Common diagnosis that fusion surgery is used for is internal disc derangement, discogenic pain, spondylolysis, spondylolisthesis, post-laminectomy spondylolisthesis, spinal deformity like scoliosis and kyphosis, and others.
Common to all fusion surgeries is the use of bone graft which can be obtained from several different sources. The discussion of bone grafting is an important one since controversy exists regarding this issue which includes the source of the graft as well as the techniques for its use.. Even though many new advances have been made in recent years, harvesting the patients own bone from areas of unused bone is still the best accepted technique. The most common area that bone is taken from is the pelvis. Since the pelvis has areas of bone that are unused it is a good source for bone graft. Another area is the Fibula (little shin bone).
The use of patients own (autologus) bone graft results in the highest rates of fusion. The downfall of autologus bone grafting is donor site morbidity, or in other words, the problems that arise in the area that the bone graft was taken from. The harvesting process creates another and separate incision with its own associated risks. In addition, there is pain at that site that must be controlled after the operation. The other option for bone grafting is the use of cadaveric bone that has been processed prior to use in surgical procedures. In some cases the use of cadaveric bone leads to slightly lower fusion rates but this technique avoids the possible complications from bone harvesting. In recent years, bone processing techniques have been developed that concentrate the chemicals stimulating bone healing and fusion. These chemicals are called BMP (bone Morphogenic Protein) and are found in high concentrations in preparations such as Grafton which are supplied by the American Red Cross. Other preparations by other companies are also available. The discussion of bone grafting is complicated and no perfect answer is yet available. This subject should be discussed thoroughly with your physician including risks, benefits, and alternatives of each choice.
Generally the best success rates of fusion occur with one level fusion. Most patients will not notice any decrease in motion since the other segments compensate for the loss of motion and most bending occur at the hip joints. Still, the fusion of 2 motion segments is very common with mostly good results. More uncommonly, 3 or even 4 levels must be fused but the expected results are lower than 1 or 2 level fusions. In cases of deformity even more segments may require fusion to achieve and maintain correct alignment. Surgical fusion of the bony segment could be approached from different sides of the spine. Again, there are risks and benefits to different approaches and your surgeon will advise you based on experience, judgment, and science to arrive at a suitable decision in each case. The spine can be approached from the front of the patient, the back, or a combined front and back procedure. Approaches from the back can further be divided into several different techniques. These include the Postero-lateral Fusion, and Posterior Lumbar Inter-body Fusion (PLIF).
For more information please visit our website at: http://www.synapsedoctor.com
You can also follow our social media pages at:
http://www.facebook.com/synapsedoctor
http://www.instagram.com/synapsedoctor
http://www.twitter.com/synapsedoctor
40
views
Back On The Bass Again After Carpal Tunnel Surgery
Meet Constant.
Constant is being treated at Synapse Orthopedic Group by Edwin Haronian MD for carpal tunnel and trigger thumb. He figured out a way of strengthening his fingers by practicing his bass.
Since he has been practicing, his fingers have gotten stronger. He really loves the staff at Synapse Orthopedic Group because they always treat him with respect. We wish Constant a great recovery.
Call us to schedule an appointment: (818) 788-2400
Locations in Pomona, Sherman Oaks, and Los Angeles
Carpal tunnel syndrome is numbness, tingling, weakness, and other problems in your hand because of pressure on the median nerve in your wrist.
The median nerve and several tendons run from your forearm to your hand through a small space in your wrist called the carpal tunnel. The median nerve controls movement and feeling in your thumb and first three fingers (not your little finger).
Pressure on the median nerve causes carpal tunnel syndrome. This pressure can come from swelling or anything that makes the carpal tunnel smaller. Many things can cause this swelling, including:
Illnesses such as hypothyroidism, rheumatoid arthritis, and diabetes.
Making the same hand movements over and over, especially if the wrist is bent down (your hands lower than your wrists), or making the same wrist movements over and over and or pregnancy.
Carpal tunnel syndrome can cause tingling, numbness, weakness, or pain in the fingers or hand. Some people may have pain in their arm between their hand and their elbow.
Symptoms most often occur in the thumb, index finger, middle finger, and half of the ring finger. If you have problems with your other fingers but your little finger is fine, this may be a sign that you have carpal tunnel syndrome. A different nerve gives feeling to the little finger.
You may first notice symptoms at night. You may be able to get relief by shaking your hand.
Mild symptoms usually can be treated with home care. You can:
Stop activities that cause numbness and pain. Rest your wrist longer between activities.
Ice your wrist for 10 to 15 minutes 1 or 2 times an hour.
Try taking nonsteroidal anti-inflammatory drugs (NSAIDs) to relieve pain and reduce swelling.
Wear a wrist splint at night. This takes pressure off your median nerve.
The sooner you start treatment, the better your chances of stopping symptoms and preventing long-term damage to the nerve.
You also may need medicine for carpal tunnel syndrome or for a health problem that made you likely to get carpal tunnel syndrome.
Surgery is an option. But it's usually used only when symptoms are so bad that you can't work or do other things even after several weeks to months of other treatment.
To keep carpal tunnel syndrome from coming back, take care of your basic health. Stay at a healthy weight. Don't smoke. Exercise to stay strong and flexible. If you have a long-term health problem, such as arthritis or diabetes, follow your doctor's advice for keeping your condition under control.
You can also try to take good care of your wrists and hands:
Try to keep your wrist in a neutral position.
Use your whole hand—not just your fingers—to hold objects.
When you type, keep your wrists straight, with your hands a little higher than your wrists. Relax your shoulders when your arms are at your sides.
If you can, switch hands often when you repeat movements.
For more information please visit our website at: http://www.synapsedoctor.com
You can also follow our social media pages at:
http://www.facebook.com/synapsedoctor
http://www.instagram.com/synapsedoctor
http://www.twitter.com/synapsedoctor
46
views
Complex Meniscus Tear Patient Recovery after Knee Surgery
Meet Ted.
Ted came to Edwin Haronian after an injury where he suffered from a complex tear of his meniscus. Since the surgery, he has been coming to Synapse Orthopedic Group for physical therapy which is helping him get better from his injury. We wish him the best during his recovery.
Call us to schedule an appointment: (818) 788-2400
Locations in Pomona, Sherman Oaks, and Los Angeles
A meniscus tear is a common knee injury. The meniscus is a rubbery, C-shaped disc that cushions your knee. Each knee has two menisci (plural of meniscus)-one at the outer edge of the knee and one at the inner edge. The menisci keep your knee steady by balancing your weight across the knee. A torn meniscus can prevent your knee from working right.
A meniscus tear is usually caused by twisting or turning quickly, often with the foot planted while the knee is bent. Meniscus tears can occur when you lift something heavy or play sports. As you get older, your meniscus gets worn. This can make it tear more easily.
There are three types of meniscus tears. Each has its own set of symptoms.
With a minor tear, you may have slight pain and swelling. This usually goes away in 2 or 3 weeks.
A moderate tear can cause pain at the side or center of your knee. Swelling slowly gets worse over 2 or 3 days. This may make your knee feel stiff and limit how you can bend your knee, but walking is usually possible. You might feel a sharp pain when you twist your knee or squat. These symptoms may go away in 1 or 2 weeks but can come back if you twist or overuse your knee. The pain may come and go for years if the tear isn't treated.
In severe tears, pieces of the torn meniscus can move into the joint space. This can make your knee catch, pop, or lock. You may not be able to straighten it. Your knee may feel "wobbly" or give way without warning. It may swell and become stiff right after the injury or within 2 or 3 days.
If you are older and your meniscus is worn, you may not know what you did to cause the tear. You may only remember feeling pain after you got up from a squatting position, for example. Pain and slight swelling are often the only symptoms.
Your doctor will ask about past injuries and what you were doing when your knee started to hurt. A physical exam will help your doctor find out if a torn meniscus is the cause of your pain. Your doctor will look at both knees and check for tenderness, range of motion, and how stable your knee is. X-rays are also usually done.
You may need to meet with an orthopedic surgeon for more testing. These tests may include an MRI, which can give a clear picture of where a tear is and how serious it is.
For more information please visit our website at: http://www.synapsedoctor.com
You can also follow our social media pages at:
http://www.facebook.com/synapsedoctor
http://www.instagram.com/synapsedoctor
http://www.twitter.com/synapsedoctor
36
views
Spondylolisthesis Patient Walks 2 Weeks After Spine Surgery
Meet Johnny.
Johnny came to Synapse Orthopedic Group and met with Edwin Haronian MD. He was diagnosed with Spondyloisthesis, which caused him to be unable to walk. A week after surgery he was able to walk, at 2 weeks he is walking a mile a day.
Edwin Haronian MD is a Spine Specialist and also the author of the book, "Back Surgery: Is It Right For You?" If you're considering Back Surgery, this book walks you through your concerns.
Call us to schedule an appointment: (818) 788-2400
Locations in Pomona, Sherman Oaks, and Los Angeles
Spondylolisthesis is the forward displacement of a vertebral bone in relation to the natural curve of the spine, most commonly occurring after a fracture, and most often the fifth lumbar vertebra. Backward displacement is referred to as retrolisthesis. When occurring in conjunction with scoliosis, the shortened term "olisthesis," may sometimes be used instead.
A hangman's fracture is a specific type of spondylolisthesis where the second cervical vertebra (C2) is displaced anteriorly relative to the C3 vertebra due to fractures of the C2 vertebra's pedicles. This is the cause of death in hanging.
Spinal fusion (such as a TLIF) is a surgical technique to stabilize the spinal vertebra and the disc or shock absorber between the vertebra. Lumbar fusion surgery is designed to create solid bone between the adjoining vertebra, eliminating any movement between the bones. The goal of the surgery is to reduce pain and nerve irritation.
Spinal fusion may be recommended for conditions such as spondylolisthesis, degenerative disc disease or recurrent disc herniations. Surgeons perform lumbar fusion using several techniques. This article describes the transforaminal lumbar interbody fusion (TLIF) fusion technique.
For more information please visit our website at: http://www.synapsedoctor.com
You can also follow our social media pages at:
http://www.facebook.com/synapsedoctor
http://www.instagram.com/synapsedoctor
http://www.twitter.com/synapsedoctor
17
views
Spinal Fusion: Recovery A Year Later
Meet Roberta.
Roberta injured herself at work in 2007. She went through several treatments prior to being approved her surgery. She came to Synapse Orthopedic Group and Edwin Haronian MD performed a Spinal Fusion. After her surgery, she completed all her following treatment, she is now just about fully recovered. She is excited and ready to bowl again!
Call us to schedule an appointment: (818) 788-2400
Locations in Pomona, Sherman Oaks, and Los Angeles
Spinal fusion is a surgical procedure used to correct problems with the small bones of the spine (vertebrae). It is essentially a "welding" process. The basic idea is to fuse together the painful vertebrae so that they heal into a single, solid bone.
Spine surgery is usually recommended only when your doctor can pinpoint the source of your pain. To do this, your doctor may use imaging tests, such as x-rays, computed tomography (CT), and magnetic resonance imaging (MRI) scans.
Spinal fusion may relieve symptoms of many back conditions, including:
Degenerative disk disease
Spondylolisthesis
Spinal stenosis
Scoliosis
Fracture
Infection
Tumor
Spinal fusion eliminates motion between vertebrae. It also prevents the stretching of nerves and surrounding ligaments and muscles. It is an option when motion is the source of pain, such as movement that occurs in a part of the spine that is arthritic. The theory is if the painful vertebrae do not move, they should not hurt.
If you have leg pain in addition to back pain, your surgeon may also perform a decompression (laminectomy). This procedure involves removing bone and diseased tissues that can put pressure on spinal nerves.
Fusion will take away some spinal flexibility, but most spinal fusions involve only small segments of the spine and do not limit motion very much.
Lumbar spinal fusion has been performed for decades. There are several different techniques that may be used to fuse the spine. There are also different "approaches" your surgeon can take for your procedure.
Your surgeon may approach your spine from the front. This is an anterior approach and requires an incision in the lower abdomen.
A posterior approach is done from your back. Or your surgeon may approach your spine from the side, called a lateral approach.
Minimally invasive techniques have also been developed. These allow fusions to be performed with smaller incisions.
The right procedure for you will depend on the nature and location of your disease.
Bone Grafting
All spinal fusions use some type of bone material, called a bone graft, to help promote the fusion. Generally, small pieces of bone are placed into the space between the vertebrae to be fused.
A bone graft is primarily used to stimulate bone healing. It increases bone production and helps the vertebrae heal together into a solid bone. Sometimes larger, solid pieces are used to provide immediate structural support to the vertebrae.
In the past, a bone graft harvested from the patient's hip was the only option for fusing the vertebrae. This type of graft is called an autograft. Harvesting a bone graft requires an additional incision during the operation. It lengthens surgery and can cause increased pain after the operation.
One alternative to harvesting a bone graft is an allograft, which is cadaver bone. An allograft is typically acquired through a bone bank.
Today, several artificial bone graft materials have also been developed.
Demineralized bone matrices (DBMs). Calcium is removed from cadaver bone to create DBMs. Without the mineral, the bone can be changed into a putty or gel-like consistency. DBMs are usually combined with other grafts, and may contain proteins that help in bone healing.
Bone morphogenetic proteins (BMPs). These very powerful synthetic bone-forming proteins promote a solid fusion. They are approved by the U.S. Food and Drug Administration for use in the spine in certain situations. Autografts may not be needed when BMPs are used.
Ceramics. Synthetic calcium/phosphate materials are similar in shape and consistency to autograft bone.
Your surgeon will discuss with you the type of bone graft material that will work best for your condition and procedure.
Immobilization
After bone grafting, the vertebrae need to be held together to help the fusion progress. Your surgeon may suggest that you wear a brace.
In many cases, surgeons will use plates, screws, and rods to help hold the spine still. This is called internal fixation, and may increase the rate of successful healing. With the added stability from internal fixation, most patients are able to move earlier after surgery.
For more information please visit our website at: http://www.synapsedoctor.com
You can also follow our social media pages at:
http://www.facebook.com/synapsedoctor
http://www.instagram.com/synapsedoctor
http://www.twitter.com/synapsedoctor
54
views
Knee Surgery for a Meniscus Tear
Meet Doretha.
Doretha came to Synapse Orthopedic Group after being injured in a bus accident. Edwin Haronian MD performed knee surgery to repair her torn meniscus., she is now recovering from her injury. She is now in the process of doing further therapy to strengthen her knee. Let's wish her a great recovery.
Call us to schedule an appointment: (818) 788-2400
Locations in Pomona, Sherman Oaks, and Los Angeles
A meniscus tear is a common injury to the cartilage that stabilizes and cushions the knee joint. The type of the tear can determine whether your tear can be repaired. Radial tears sometimes can be repaired, depending on where they are located. Horizontal, flap, long-standing, and degenerative tears-those caused by years of wear and tear-generally cannot be repaired.
Your doctor will likely suggest the treatment that he or she thinks will work best for you based on the zone where the tear is , the pattern of the tear, and how big it is. Your age, your health, and your activity level may also affect your treatment options. In some cases, the surgeon makes the final decision during surgery, when he or she can see the how strong the meniscus is, where the tear is, and how big the tear is.
If you have a small tear at the outer edge of the meniscus (in what doctors call the red zone), you may want to try home treatment. These tears often heal with rest.
If you have a moderate to large tear at the outer edge of the meniscus (red zone), you may want to think about surgery. These kinds of tears tend to heal well after surgery.
If you have a tear that spreads from the red zone into the inner two-thirds of the meniscus (called the white zone), your decision is harder. Surgery to repair these kinds of tears may not work.
If you have a tear in the white zone of the meniscus, repair surgery usually isn't done, because the meniscus may not heal. But partial meniscectomy may be done if torn pieces of meniscus are causing pain and swelling.
Surgical repair may be done by open surgery, in which a small incision is made and the knee is opened up so that the surgeon can see inside the knee and the meniscus can be repaired. Increasingly, surgeons use arthroscopic surgery to repair the meniscus. The surgeon inserts a thin tube (arthroscope) containing a camera and a light through small incisions near the knee and is able to see inside the knee without making a large incision. Surgical instruments can be inserted through other small incisions. The surgeon repairs the meniscus using sutures (stitches) or anchors.
Other knee injuries-most commonly to the anterior cruciate ligament (ACL)-may occur at the same time as a torn meniscus. In these cases, the treatment plan is altered. Typically, your orthopedist will repair your torn meniscus, if needed, at the same time ACL surgery is done. In this case, the ACL rehabilitation plan is followed. To learn more, see the topic Anterior Cruciate Ligament (ACL) Injuries.
What To Expect After Surgery
Your surgeon may recommend that you do not move your knee more than absolutely necessary (immobilization) for 2 weeks after surgery. This may be followed by 2 weeks of limited motion before you are able to resume daily activities. Physical therapy should begin right after surgery. But heavy stresses, such as running and squats, should be postponed for some months. You must follow your doctor's rehabilitation (rehab) plan for optimum healing. Afterwards, you may still continue to have pain and require more physical therapy or, sometimes, additional surgery.
The timetable for returning to walking, driving, and more vigorous activities will depend on your success in rehab.
Why It Is Done
How your doctor treats a meniscus tear depends upon the size and location of the tear, your age, your health and activity level, and when the injury occurred. Treatment options include nonsurgical treatment with rest, ice, compression, elevation, and physical therapy; surgical repair; surgical removal of the torn section (partial meniscectomy); and surgical removal of the entire meniscus (total meniscectomy). In general, surgical repair is favored over partial or total meniscectomy. If the meniscus can be repaired successfully, saving the injured meniscus by doing a meniscal repair-rather than partial or total removal-reduces the occurrence of knee-joint degeneration.
Small tears located at the outer edge of the meniscus often heal on their own. Larger tears located toward the center of the meniscus may not heal well, because blood supply to that area is poor. In a young person, surgery to repair the tear may be the first choice, because it may restore function.
For more information please visit our website at: http://www.synapsedoctor.com
You can also follow our social media pages at:
http://www.facebook.com/synapsedoctor
http://www.instagram.com/synapsedoctor
http://www.twitter.com/synapsedoctor
83
views
Spine Stimulator Implant Patient
Donald Hockett had been experiencing pain for years and was misdiagnosed with arthritis. Continuing in pain, Donald was referred to Synapse Orthopedic Group. Edwin Haronian MD performed a second opinion and discovered that Donald had a 9mm protusion of the L4 L5. After discussing several routes, Jonathan Kohan MD provided him a Spine Stimulator Implant to reduce his pain. Since receiving the implant, he is mobile and playing with his grandchildren again. He has his life back.
Call us to schedule an appointment: (818) 788-2400
Locations in Pomona, Sherman Oaks, and Los Angeles
Spine Stimulator:
People whose back or neck pain has not been relieved by back surgery or other treatments may have another option to consider: spinal cord stimulation.
Around the world, some 14,000 patients undergo spinal cord stimulator implants each year. Spinal cord stimulation (SCS) delivers mild electrical stimulation to nerves along the spinal column, modifying or blocking nerve activity in a non-medicinal way to minimize the sensation of pain reaching the brain.
Spinal cord stimulation was first used to treat pain in 1967. Spinal cord stimulation was approved by the Food and Drug Administration (FDA) in 1989 to relieve pain from nerve damage in the trunk, arms, or legs, and now accounts for about 90 percent of all neuromodulation treatments. That number is expected to grow to manage chronic disease states as the population ages and as spinal cord stimulation is expanded to treat other diseases.
Spinal cord stimulation, also called neurostimulation, directs mild electrical pulses to interfere with pain messages reaching the brain. A small device implanted near the spine generates these pulses. The implanted generator used in spinal cord stimulation has similarities to a cardiac pacemaker, leading some to call the device a pacemaker for pain.
A spinal cord stimulator is a device used to exert pulsed electrical signals to the spinal cord to control chronic pain. Further applications are in motor disorders. The lumbar spinal cord is a preferred target for the control of spinal spasticity or augmentation of standing and stepping capabilities. Spinal cord stimulation (SCS), in the simplest form, consists of stimulating electrodes, implanted in the epidural space, an electrical pulse generator, implanted in the lower abdominal area or gluteal region, conducting wires connecting the electrodes to the generator, and the generator remote control. SCS has notable analgesic properties and, at the present, is used mostly in the treatment of failed back surgery syndrome, complex regional pain syndrome and refractory pain due to ischemia.
The most common use of SCS is failed back surgery syndrome (FBSS) in the United States and peripheral ischemic pain in Europe.
FBSS, classified as mixed pain syndrome (neuropathic and nociceptive), is the persistent or recurrent pain, mainly involving the lower back and/or legs after successful spinal surgery. It affects about 40% of patients who undergo spinal surgeries. Several studies showed overall efficacy of the SCS for FBSS.
SCS is also indicated in the treatment of inoperable ischemic limb pain.Furthermore, this technique is studied in various applications. For instance, it has been shown to modulate the function of sympathetic nervous system and increase norepinephrine release in refractory angina pectoris, decreasing the probability of angina attack. SCS units have been used to treat patients with frequent migraines. The electrodes are implanted in the bilateral suboccipital region.
For more information please visit our website at: http://www.synapsedoctor.com
You can also follow our social media pages at:
http://www.facebook.com/synapsedoctor
http://www.instagram.com/synapsedoctor
http://www.twitter.com/synapsedoctor
85
views