What Causes Shortness of Breath After Eating? 💨
What causes shortness of breath after eating? Have you ever experienced this unwanted symptom? Watch this video to find out the most common causes.
💥Shortness of Breath After Eating [Full Guide] ➜ ➜ ➜ https://bit.ly/3P7EMju
Experiencing shortness of breath after eating can result from several factors, including overeating, food allergies, or gastroesophageal reflux disease (GERD). More serious conditions like heart or lung diseases can also manifest this unwanted sensation. Therefore, it’s essential to identify the cause and consult a medical professional if symptoms persist or are recurrent.
🟦 Causes of Shortness of Breath After Eating
■ Overeating: Consuming large meals can put pressure on the diaphragm, restricting lung expansion and causing shortness of breath.
■ Gastroesophageal Reflux Disease (GERD): Acid reflux can lead to shortness of breath when stomach acid flows back into the esophagus, irritating its lining.
■ Food Allergies: An allergic reaction to specific foods can cause an array of symptoms, including difficulty breathing. This is particularly true in the case of anaphylaxis, a severe allergic reaction.
■ Hiatal Hernia: A part of the stomach pushes up into the diaphragm, which can lead to breathing problems after eating.
■ Asthma: Some individuals have asthma that is triggered by certain foods or by eating in general.
■ Heart Problems: Conditions such as congestive heart failure can result in shortness of breath after consuming a meal.
■ Chronic Obstructive Pulmonary Disease (COPD): In people with COPD, the airways are blocked or damaged, making it hard to get enough oxygen.
■ Obesity: Carrying excess weight, especially around the midsection, can put pressure on the diaphragm and lungs, leading to breathing difficulties after meals.
■ Anxiety: Panic attacks or anxiety can sometimes be triggered by meals and manifest as shortness of breath.
■ Carbohydrate-Rich Meals: Consuming foods high in carbohydrates can increase the production of carbon dioxide, which, in turn, might cause shortness of breath in some people.
It is important to pinpoint the exact cause of shortness of breath after eating because the remedies and treatments vary considerably based on the underlying reason. If someone consistently experiences this symptom, consulting a healthcare professional is crucial to ensure an accurate diagnosis and appropriate care.
💥Shortness of Breath After Eating [Full Guide] ➜ ➜ ➜ https://bit.ly/3P7EMju
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
1:04 - Overeating
1:12 - Gastroesophageal Reflux Disease (GERD)
1:26 - Food Allergies
1:42 - Hiatal Hernia
1:51 - Asthma
1:59 - Heart Problems
2:07 - COPD
2:15 - Obesity
2:27 - Anxiety
2:35 - Carbohydrate-Rich Meals
3:15 - Eat Moderate Portion Sizes
3:30 - Manage Acid Reflux
3:46 - Identify and Avoid Food Allergens
4:00 - Maintain a Healthy Weight
4:10 - Avoid Triggers for Asthma and COPD
4:22 - Manage Anxiety
4:33 - Limit Carbonated Drinks
4:44 - Limit High-carbohydrate Meals
4:55 - Stay Upright After Eating
5:07 - Wear Loose Clothing
5:14 - Avoid Smoking
5;21 - Limit Alcohol Intake
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#dyspnea #cantbreathe #shortnessofbreath
76
views
What is a Calcified Granuloma in the Lungs? 🫁
What is a Calcified Granuloma in the Lungs? This video covers the medical definition and provides a brief overview of this topic.
💥Calcified Granuloma in the Lungs [Full Guide] ➜ ➜ ➜ https://bit.ly/3qvK3YE
➡️ Calcified Granuloma in the Lungs
A calcified granuloma in the lungs is a small, benign nodule that forms as a result of the body’s attempt to isolate and contain an old infection or foreign substance. Over time, calcium deposits can accumulate within the granuloma, making it visible on an X-ray. Calcified granulomas in the lungs are primarily caused by infections or immune responses to foreign substances.
Infections that can trigger granuloma formation include tuberculosis (TB), caused by the Mycobacterium tuberculosis bacterium, and fungal infections, such as histoplasmosis or coccidioidomycosis. These infections often result in the body’s immune cells clustering to form nodules within the lung tissue. In addition to infections, inflammatory conditions, and autoimmune diseases can also lead to the development of granulomas.
➡️ Symptoms and Complications
The symptoms of calcified lung granulomas can vary and may be mild or absent in some cases. Individuals with lung granulomas may experience a cough, which can be either dry or productive. In some cases, the cough might become chronic and persist for a long time. Patients may also report shortness of breath and difficulty in performing routine activities. Wheezing is another symptom that can be observed in some individuals, especially when the granuloma obstructs the airways. Chest pain is another possible symptom, which can range from mild discomfort to severe, depending on the location and size of the granuloma.
Infections, such as histoplasmosis, can cause additional symptoms like fever and general malaise. When lung granulomas progress or are left untreated, complications could arise. One such complication is the development of fibrosis, which is the thickening and scarring of lung tissue. In severe cases, extensive fibrosis can lead to a condition called pulmonary fibrosis, in which the lungs lose their ability to efficiently exchange oxygen and carbon dioxide. This can lead to respiratory failure and other serious health problems.
💥Calcified Granuloma in the Lungs [Full Guide] ➜ ➜ ➜ https://bit.ly/3qvK3YE
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:30 - Calcified Granuloma
0:55 - Infections
1:21 - Symptoms and Complications
2:35 - Diagnosis
4:21 - Treatment Options
5:47 - Outlook and Prevention
6:04 - Steps to Help Prevent
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#lungs #granuloma #calcifiedgranuloma
58
views
Lung Volumes & Capacities 🫁
Full video: https://youtu.be/X4oYypVIak4?si=958Ipedy3rbm2MWu
#lungvolume #lungcapacity
19
views
Better Posture = Better Lungs 🫁
Full video: https://youtu.be/BX3BhKTyaJg?si=R7wCNlBUUULnoMEF
#lungs #respiratorytract #respiratorysystem
12
views
Importance of Your Upper Respiratory Tract 🫁
Full video: https://youtu.be/BX3BhKTyaJg?si=R7wCNlBUUULnoMEF
#lungs #respiratorytract #respiratorysystem
13
views
Boost Lung Capacity with Breathing Exercises 🫁
Full Video: https://youtu.be/aVdUpwLxyUU?si=qScd-EcMJCRBQTDT
#lungs #lungcapacity
16
views
Lung Capacity for Better Health? 🫁
Full Video: https://youtu.be/aVdUpwLxyUU?si=qScd-EcMJCRBQTDT
#lungs #lungcapacity
8
views
What is FEV1? 🫁
Full video here: https://youtu.be/ow5THCmmLLc?si=He89k3NWNzW_XYfs
#FEV1 #pulmonaryfunctiontesting
6
views
Lung Volumes vs. Capacities *Quick Explainer Video*
What is the difference between Lung Volumes and Capacities? This video covers the medical definitions and provides a brief overview of this topic.
💥PFT Basics [Full Guide] ➜ ➜ ➜ https://bit.ly/2A8ZuvQ
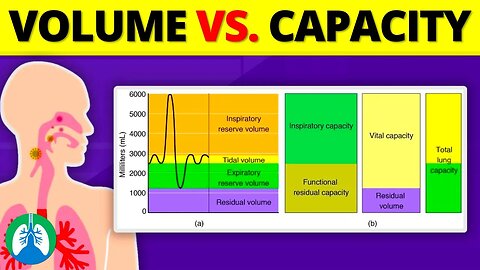
➡️ Lung Volumes
Lung volumes refer to discrete, measurable segments of air that can be associated with a specific phase of the breathing cycle. The four primary lung volumes include:
-- Tidal Volume (VT): The volume of air inhaled or exhaled during a normal, resting breath.
-- Inspiratory Reserve Volume (IRV): The additional volume of air that can be forcefully inhaled after a normal inhalation.
-- Expiratory Reserve Volume (ERV): The additional volume of air that can be forcefully exhaled after a normal exhalation.
-- Residual Volume (RV): The amount of air remaining in the lungs after a maximal exhalation. This volume ensures that gas exchange can continue between breaths and maintains lung elasticity.
➡️ Lung Capacities
Lung capacities are combinations of two or more lung volumes. The primary lung capacities include:
-- Inspiratory Capacity (IC) The total volume of air that can be inhaled after a normal exhalation.
-- Functional Residual Capacity (FRC): The volume of air exhaled after a normal tidal volume breath in addition to the volume remaining in the lungs after maximum exhalation.
-- Vital Capacity (VC): The total volume of air that can be forcefully exhaled after a maximal inhalation. This capacity gives insight into the overall health and function of the respiratory muscles.
-- Total Lung Capacity (TLC): The total volume of the lungs when fully expanded; the sum of all lung volumes.
Lung volumes and capacities are fundamental concepts in respiratory physiology, offering deep insights into the function and potential of the human lungs. While volumes provide discrete measures during different phases of respiration, capacities represent combined functional segments.
💥PFT Basics [Full Guide] ➜ ➜ ➜ https://bit.ly/2A8ZuvQ
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:32 - Lung Volumes
0:46 - Tidal Volume (VT)
0:53 - Inspiratory Reserve Volume (IRV)
1:02 - Expiratory Reserve Volume (ERV)
1:10 - Residual Volume (RV)
1:25 - Lung Capacities
1:35 - Inspiratory Capacity (IC)
1:50 - Functional Residual Capacity (FRC)
2:09 - Vital Capacity (VC)
2:33 - Total Lung Capacity (TLC)
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#lungvolume #lungcapacity #pulmonaryfunctiontesting
21
views
Boost Lung Capacity with Lung Exerciser Devices 🫁
Full Video: https://youtu.be/aVdUpwLxyUU?si=qScd-EcMJCRBQTDT
#lungs #lungcapacity
8
views
What is the FEV1/FVC Ratio? 🫁
Full video: https://youtu.be/ow5THCmmLLc?si=He89k3NWNzW_XYfs
#FEV1 #pulmonaryfunctiontesting
8
views
Infection Control: Disinfection vs. Sterilization 🦠
Full video: https://youtu.be/pKH8HQMzM3U?si=X85DtO03ruagMwuu
#infectioncontrol #Disinfection #Sterilization
30
views
What is Winters' Formula? *EXPLAINED* 💡
What is Winters' Formula? This video explains how this formula is used to calculate a patient’s predicted PaCO2 based on their arterial blood gas (ABG) results.
💥Winters' Formula [Full Guide] ➜ ➜ ➜ https://bit.ly/3QaBzgK
➡️ Equation
The formula uses the following equation: Expected PaCO2 = (1.5 x HCO3-) + 8 ± 2
The patient’s bicarbonate value (HCO3-) is obtained by collecting and analyzing a sample of arterial blood. Then you can use Winters’ formula to determine the expected PaCO2 simply by inserting the HCO3- value into the equation.
➡️ How to Use Winters’ Formula
You can estimate a patient’s PaCO2 simply by inserting the measured HCO3- value into the equation. Then you can compare the estimated PaCO2 value to the patient’s actual measured PaCO2. This can result in three possible scenarios:
-- Measured PaCO2 = Estimated PaCO2
-- Measured PaCO2 greater than Estimated PaCO2
-- Measured PaCO2 less than Estimated PaCO2
➡️ Measured PaCO2 = Estimated PaCO2
If the patient’s PaCO2 is within the expected PaCO2 range, it indicates that respiratory compensation is taking place. This is considered to be pure metabolic acidosis. However, if the patient’s PaCO2 is not within the expected range, it means that a mixed disorder is present.
➡️ Measured PaCO2 greater than Estimated PaCO2
If the patient’s measured PaCO2 is greater than the estimated PaCO2, it indicates that the patient has respiratory acidosis in addition to metabolic acidosis. This is because the patient’s respiratory system is not compensating enough for metabolic acidosis, resulting in an increased PaCO2.
➡️ Measured PaCO2 less than Estimated PaCO2
If the patient’s measured PaCO2 is less than the estimated PaCO2, it indicates that the patient has respiratory alkalosis in addition to metabolic acidosis. This is because the patient’s respiratory system is overcompensating for metabolic acidosis, resulting in a decreased PaCO2.
💥Winters' Formula [Full Guide] ➜ ➜ ➜ https://bit.ly/3QaBzgK
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
043 - Winter's Formula
122 - How to Use Winters’ Formula
157 - Measured PaCO2 = Estimated PaCO2
223 - Measured PaCO2 greater than Estimated PaCO2
251 - Measured PaCO2 less than Estimated PaCO2
326 - Parts of the Winters’ Formula Equation
403 - Expected PaCO2
436 - HCO3-
501 - 1.5 Constant
515 - 8 Constant
530 - ± 2 Constant
557 - Types of Acid-Base Disorders
635 - Metabolic Acidosis
710 - Metabolic Alkalosis
734 - Respiratory Alkalosis
759 - Respiratory Acidosis
828 - Respiratory Compensation
913 - Example #1
1050 - Example #2
1216 - Example #3
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#paco2 #abg #wintersformula
80
views
Infection Control TMC Practice Question ❓
The video breaks down a sample TMC practice question about infection control and surface disinfection. Can you guess the correct answer?
💥TMC Test Bank [Practice Questions] ➜ ➜ ➜ https://bit.ly/3QNqwLX
💥Daily Practice Questions [via Email] ➜ ➜ ➜ http://bit.ly/2NnXh3C
➡️ Question
A BiPAP machine that was used in the emergency department has been returned for cleaning. Which of the following agents would you recommend for surface disinfection?
A. Ethylene oxide
B. 70% ethyl alcohol
C. Alkaline glutaraldehyde
D. Acetic acid
To get this one correct, you needed to know which substance in the answer choices can be used as a disinfectant. The first answer choice, ethylene oxide, is used for sterilization in heat or moisture-sensitive items, such as plastics in respiratory care equipment. We're looking for a method of disinfection, not sterilization; so we can rule out 'A' because we know it's not the correct answer. Alkaline glutaraldehyde is used for high-level disinfection and sterilization and requires the object to be submerged in the solution for a period of time. This is not possible with a BiPAP machine; therefore, we can rule out 'C' as well. Acetic acid is a disinfectant; however, it is typically recommended for use in a patient’s home, not in the hospital, which means that we can rule out answer-choice 'D.' Remember: Alcohol-based solutions are typically used to disinfect surfaces in the hospital setting. Therefore, that is what’s recommended to clean the surface of a BiPAP machine, which should be performed before use on a new patient.
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
035 - Practice Question
1:00 - Explanation
2:13 - Correct Answer
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#respiratorytherapyzone #tmcexam #tmcpracticequestion
26
views
Febrile (Medical Definition) | Quick Explainer Video
What does Febrile mean? This video covers the medical definition and provides a brief overview of this topic.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
➡️ Febrile
Febrile states are typically part of the body's defense mechanism against infection or other medical conditions. When a person is in a febrile condition, it signifies that the body's immune system has been activated in response to a potential threat such as a virus, bacteria, or other pathogenic agents. The hypothalamus, the body's temperature control center, raises the body's set point for temperature in response to these threats, resulting in a fever.
➡️ Febrile Seizures
Febrile seizures, for instance, are a specific type of seizure event that can occur in children aged six months to five years during a febrile episode. These seizures are usually associated with a rapid increase in body temperature, and while they can be frightening for parents to witness, they're typically harmless and often don't indicate a serious underlying condition. However, any febrile seizure should be evaluated by a healthcare professional.
The term febrile is also used in medicine to describe conditions or reactions that are accompanied by fever. For example, a febrile illness is a broader term that covers any illness or condition that causes a fever. Similarly, a febrile response is the body's response to an illness that results in a fever. Febrile neutropenia, another term where "febrile" is used, is a condition that often occurs in people receiving cancer treatments. It's marked by a fever and a low number of a type of white blood cells called neutrophils, making the individual extremely susceptible to infections.
In clinical settings, monitoring a patient's febrile state is crucial as it provides significant information about the patient's condition. An unexplained, persistent febrile state may indicate a serious underlying condition such as an infection, malignancy, or autoimmune disease. Therefore, it is critical to determine the cause of a febrile state, especially when it is prolonged or recurrent, in order to properly treat the underlying condition. In therapeutic settings, a controlled febrile state might be induced for certain treatments, such as in the case of hyperthermia or pyrotherapy.
These therapies leverage the body's natural defense mechanism, where the elevation in body temperature enhances the effectiveness of certain treatments, particularly in oncological care. The term "febrile" refers to anything relating to or characterized by fever. A febrile state is a signal that the body's immune system is working to combat an infection or disease. Understanding and managing febrile conditions properly is crucial in patient care, as it provides key insights into the body's response to a potential health threat. Despite being a symptom, it is a critical part of the body's natural defense mechanism.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:35 - Febrile
1:06 - Febrile Seizures
1:58 - Febrile Neutropenia
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#febrile #fever #medicaldefinition
29
views
Ventilatory Threshold Measurement ❓💨 #respiratorytherapyzone
➡️ Measuring Ventilatory Threshold
Various methods can be employed to measure the ventilatory threshold, including gas exchange measurements, lactate analysis, and the ventilatory equivalent method. Gas exchange measurements involve monitoring the rates of oxygen consumption and carbon dioxide production during an incremental exercise test, typically performed on a treadmill or cycle ergometer. Lactate analysis involves measuring blood lactate concentrations at different exercise intensities to determine the points where lactate accumulation begins to rise significantly. The ventilatory equivalent method involves monitoring the ventilatory equivalent for oxygen and carbon dioxide and identifying breakpoints or deflections in the plotted data.
14
views
FEV1 (Medical Definition) | Quick Explainer Video
What is FEV1? This video covers the medical definition and provides a brief overview of this topic.
💥PFT Basics [Full Guide] ➜ ➜ ➜ https://bit.ly/2A8ZuvQ
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
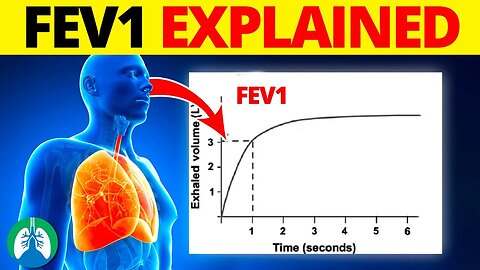
The value of FEV1 is primarily used to assess the presence and severity of pulmonary diseases, including asthma and chronic obstructive pulmonary disease (COPD). The procedure for FEV1 is simple and noninvasive. The patient takes a deep breath and then blows out as hard and fast as they can into a device called a spirometer.
The spirometer then records the total volume of air exhaled and the rate at which it is expelled. The FEV1 is the volume measured within the first second of this forced exhalation. In a healthy individual, a large percentage of the lung's total capacity is expelled within this first second. However, in patients with obstructive lung diseases like asthma or COPD, airway obstruction reduces the speed and volume of air that can be exhaled. As a result, a smaller percentage of the total lung volume is expelled in the first second, leading to a reduced FEV1.
FEV1 is commonly interpreted in conjunction with another spirometry measurement, known as the Forced Vital Capacity (FVC). This is the total amount of air that can be forcibly exhaled after taking the deepest breath possible. The ratio of FEV1 to FVC (FEV1/FVC ratio) provides valuable diagnostic information. In healthy adults, the FEV1/FVC ratio is typically above 70%, and a ratio below 70% is indicative of airway obstruction, suggestive of conditions like COPD.
It is important to note that FEV1 values are not absolute. They are often compared to predicted normal values based on the individual's height, age, sex, and ethnicity, as these factors can influence lung volume and capacity. In respiratory care, an FEV1 score of less than 80% of the predicted value generally suggests a lung disease. Monitoring FEV1 over time allows healthcare providers to evaluate the progression of pulmonary diseases and the effectiveness of treatments.
For instance, in patients with asthma, an improved FEV1 following inhaler use can confirm the responsiveness to the treatment. However, while FEV1 is a valuable measurement, it does not provide a comprehensive picture of lung health on its own. It is one aspect of a complete pulmonary function test, which may include other measures such as total lung capacity (TLC) and gas exchange efficiency.
FEV1 is a vital tool in the assessment and monitoring of pulmonary diseases. It offers significant insights into the extent of airway obstruction and response to treatment. Although it's just one component of pulmonary function testing, FEV1 plays a critical role in guiding the diagnosis, treatment, and management of various respiratory conditions.
💥PFT Basics [Full Guide] ➜ ➜ ➜ https://bit.ly/2A8ZuvQ
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:25 - Value of FEV1
0:35 - Procedure for FEV1
0:48 - Spirometer
1:28 - FEV1
2:29 - Monitoring FEV1
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#PFT #FEV1 #pulmonaryfunctiontesting
26
views
Breathing Exercises to Increase Oxygen Levels? 💨
Full video 👉 https://youtu.be/2R_3CqzDjgQ?si=UUkYsSl5C-y_Lx66
24
views
Upper Respiratory Tract - *Quick Explainer Video*
What is the Upper Respiratory Tract? This video covers the medical definition and provides a brief overview of this topic.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
Starting from the most external part of the tract, the nasal cavity is the body's primary entryway for air. It comprises an inner space in the nose, divided by the septum. Its walls are lined with cilia and mucus, which serve as the first line of defense against foreign particles, such as dust and microorganisms.
Moreover, the nasal cavity has a role in warming and humidifying inhaled air, preparing it for the lower respiratory tract. The pharynx, or throat, is a funnel-shaped tube that extends from the base of the skull to the level of the sixth cervical vertebra. It functions as a passageway for air from the nasal cavity to the larynx and for food from the mouth to the esophagus. The pharynx is divided into three parts: the nasopharynx (the uppermost portion), the oropharynx (middle section), and the laryngopharynx (the lower part). Notably, the pharynx hosts clusters of lymphatic tissues, known as tonsils, that protect the body against airborne pathogens.
Further down, the larynx, also known as the voice box, connects the pharynx and the trachea. It contains the vocal cords, which vibrate and produce sound when air passes through them. The larynx also has a critical safety function. A small leaf-shaped flap of cartilage called the epiglottis covers the larynx during swallowing, preventing food or liquid from entering the lungs.
It is noteworthy that the upper respiratory tract also plays a critical role in human speech production. The manipulation of airflow through the tract, along with the movement of the tongue and lips, allows us to produce an array of sounds and words. The upper respiratory tract can be affected by various conditions and diseases, ranging from the common cold and influenza to more severe conditions such as epiglottitis and laryngeal cancer.
These conditions can affect the quality of life, as they can lead to symptoms such as coughing, sneezing, difficulty breathing, and loss of voice. The upper respiratory tract is not just a simple conduit for air to reach our lungs. It is a complex, multifunctional system that provides critical protective and physiological functions. It filters, warms, and humidifies air, helps to produce sounds for speech, and guards us against a variety of pathogens. Understanding the upper respiratory tract is an essential step in learning the intricacies of the human respiratory system.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:25 - Nasal Cavity
0:58 - Pharynx
1:38 - Larynx
2:20 - Upper Respiratory Tract
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#respiratorytract #upperrespiratorytract #respiratorysystem
53
views
Tracheostomy Procedure *Explained* #respiratory #tracheostomy
What is a Tracheostomy? 💥FULL VIDEO ➜ ➜➜ https://youtu.be/4DWgaWj_ceI?si=oORxtdaSrucYJZNM
💥Tracheostomy Tubes [Full Guide] ➜ ➜ ➜ https://bit.ly/33gFyCi
28
views
What is a Tracheostomy?
What is a Tracheostomy?
💥FULL VIDEO ➜ ➜ ➜https://youtu.be/4DWgaWj_ceI?si=oORxtdaSrucYJZNM
💥Tracheostomy Tubes [Full Guide] ➜ ➜ ➜ https://bit.ly/33gFyCi
29
views
The BEST Methods to Increase Lung Capacity Today 📈
How can you increase your lung capacity today? Is it possible? Watch this video to find out! Hint: I think you'll like what you see.
💥How to Increase Lung Capacity [Full Guide] ➜ ➜ ➜ https://bit.ly/43lp4Fb
➡️ Exercise and Physical Activity
Regular physical activity is a powerful tool for enhancing lung capacity. When you exercise, your body’s demand for oxygen increases, prompting your lungs to work harder to supply this vital element. This process, over time, can lead to an increase in lung capacity.
➡️ Quit Smoking
Smoking is a major risk factor for reduced lung capacity and various respiratory diseases. The harmful chemicals in cigarette smoke cause inflammation and damage to lung tissue, leading to a decrease in lung capacity. When you quit smoking, your lungs begin to heal, inflammation reduces, and lung function improves. The benefits of quitting smoking are immediate and significant.
➡️ Breathing Exercises
Breathing exercises are a simple yet effective way to increase lung capacity. These exercises work by strengthening the diaphragm and other muscles involved in respiration, improving lung efficiency and capacity. Techniques such as diaphragmatic breathing and pursed-lip breathing can contribute to improved lung function. Regular practice of these exercises can also help clear the airways, reduce stress, and improve oxygen delivery to the body’s tissues. Watch the video for the rest of the methods.
💥How to Increase Lung Capacity [Full Guide] ➜ ➜ ➜ https://bit.ly/43lp4Fb
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:32 - Exercise and Physical Activity
1:23 - Quit Smoking
2:05 - Breathing Exercises
2:47 - Eat a Lung-Healthy Diet
3:36 - Pulmonary Rehabilitation
4:15 - Use a Lung Exerciser Device
4:55 - Prevent Lung Infections
5:28 - Drink Lung-Healthy Beverages
6:05 - Perform Controlled Coughing
6:41 - Use Chest Percussion
7:13 - Maintain Good Posture
7:48 - Practice Yoga
8:24 - Seek Help
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#lungs #lungcapacity #lunghealth
83
views
Do THIS to Increase Blood OXYGEN Levels Now 🩸
This video breaks down the best methods to increase your blood oxygen levels, from lifestyle adjustments to interventions you can try at home.
💥Increase Blood Oxygen Levels [Full Guide] ➜ ➜ ➜ https://bit.ly/42z2NV4
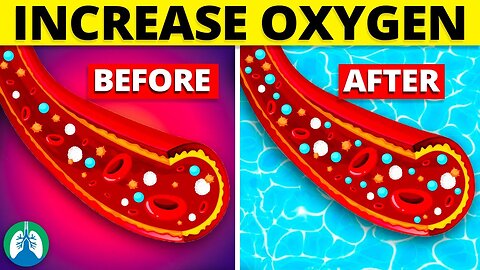
➡️ Oxygen Therapy
Supplemental oxygen therapy is a medical treatment prescribed to individuals with hypoxemia, a condition characterized by low blood oxygen levels. Hypoxemia can result from various conditions, such as COPD, asthma, sleep apnea, or lung infections. Oxygen therapy helps improve blood saturation by providing additional oxygen through various devices, such as nasal cannulas, oxygen masks, or portable oxygen concentrators.
➡️ Hyperbaric Oxygen
Hyperbaric oxygen therapy (HBOT) is a medical treatment that exposes patients to pure oxygen under increased atmospheric pressure within a specialized chamber. This process allows for a higher concentration of oxygen to be dissolved in the bloodstream, thereby increasing blood oxygen levels and promoting faster healing of tissues.
➡️ Plants
Plants can naturally improve indoor air quality and increase oxygen levels by converting carbon dioxide into oxygen through the process of photosynthesis. Incorporating plants like snake plants, areca palms, and spider plants into your living space can help boost the oxygen content in your environment, making it easier to breathe and promoting overall well-being.
➡️ Climate
Climate can significantly impact blood oxygen levels due to various factors such as altitude, humidity, and air quality. Higher altitudes typically have lower air pressure and reduced oxygen content. Watch the video for the remaining tactics!
💥Increase Blood Oxygen Levels [Full Guide] ➜ ➜ ➜ https://bit.ly/42z2NV4
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:47 - Oxygen Therapy
1:35 - Hyperbaric Oxygen
2:11 - Plants
2:41 - Climate
3:44 - Exercise
4:10 - Deep Breathing
4:39 - Posture
5:15 - Stop Smoking
5:49 - Diet
6:32 - Breathing Exercises
7:23 - Hydration
7:56 - Obesity
8:39 - Lung Infections
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#respiratorytherapy #respiratorytherapist #respiratorytherapyschool
125
views
Ventilatory Threshold (Medical Definition) | Quick Explainer Video
What is the Ventilatory Threshold? This video covers the medical definition and provides a brief overview of this topic.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
Two distinct ventilatory thresholds can be identified during incremental exercise: the first ventilatory threshold (VT1) and the second ventilatory threshold (VT2).
➡️ First Ventilatory Threshold (VT1)
Also known as the aerobic threshold, marks the point at which the body starts to rely more on anaerobic metabolism to meet the energy demands of exercise. This shift occurs when lactic acid starts to accumulate in the bloodstream faster than it can be cleared, causing an increase in carbon dioxide production. At this threshold, ventilation becomes slightly disproportionate to the amount of oxygen being consumed, leading to an increased respiratory rate.
➡️ Second Ventilatory Threshold (VT2)
Also known as the anaerobic threshold, is the point at which the reliance on anaerobic metabolism becomes more pronounced. At this stage, lactic acid accumulates rapidly, and the body can no longer maintain a steady state of exercise. This leads to a significant increase in carbon dioxide production, which triggers a marked increase in ventilation to expel the excess carbon dioxide. Exercise intensity at VT2 is considered very high, and it can only be sustained for a short period of time.
➡️ Measuring Ventilatory Threshold
Various methods can be employed to measure the ventilatory threshold, including gas exchange measurements, lactate analysis, and the ventilatory equivalent method. Gas exchange measurements involve monitoring the rates of oxygen consumption and carbon dioxide production during an incremental exercise test, typically performed on a treadmill or cycle ergometer. Lactate analysis involves measuring blood lactate concentrations at different exercise intensities to determine the points where lactate accumulation begins to rise significantly. The ventilatory equivalent method involves monitoring the ventilatory equivalent for oxygen and carbon dioxide and identifying breakpoints or deflections in the plotted data.
Understanding an individual's ventilatory thresholds is crucial for optimizing training programs, particularly for endurance athletes. By training at intensities near or between these thresholds, athletes can improve their aerobic and anaerobic capacities, allowing them to perform at higher intensities for more extended periods.
Additionally, the ventilatory threshold serves as an indicator of an individual's overall fitness level and can be used to monitor the effectiveness of a training program. The ventilatory threshold is a vital physiological concept that provides valuable information about an individual's metabolic response to exercise. Identifying and understanding these thresholds is crucial for optimizing training programs and assessing athletic performance.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:36 - First Ventilatory Threshold (VT1)
1:15 - Second Ventilatory Threshold (VT2)
1:53 - Measuring Ventilatory Threshold
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#respiratorytherapy #respiratorytherapist #ventilatorythreshold
25
views