Tracheostomy (Medical Definition) | Quick Explainer Video
What is a Tracheostomy? This video covers the medical definition and provides a brief overview of this topic.
💥Tracheostomy Tubes [Full Guide] ➜ ➜ ➜ https://bit.ly/33gFyCi
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
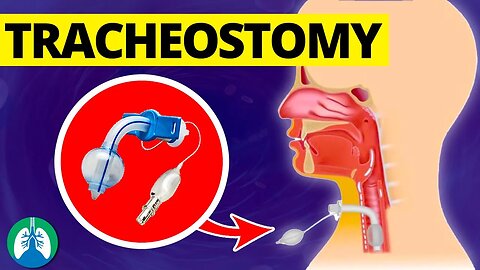
➡️ Tracheostomy
A tracheostomy procedure involves making an incision in the neck, creating an opening in the trachea, and inserting a tracheostomy tube. This tube serves as a conduit for airflow directly into the lungs. It is secured in place with a neck strap and can be cleaned, replaced, or removed as needed under medical supervision. A tracheostomy can be performed as an emergency procedure or as a planned operation, depending on the patient's condition.
Emergency tracheostomies are usually carried out due to sudden and life-threatening conditions such as a blocked airway due to an accident, allergic reaction, or severe infection. Planned tracheostomies are commonly done for patients with neuromuscular conditions or lung diseases who require long-term mechanical ventilatory support, or in cases where certain head or neck surgeries prevent normal breathing.
➡️ Benefits
A tracheostomy can provide several benefits, such as allowing patients to breathe without the use of their nose or mouth, reducing the need for prolonged intubation, which can cause damage to the larynx and other parts of the upper airway, and enabling the removal of lung secretions. Furthermore, a tracheostomy can provide a stable airway for patients who are in a coma or sedated for a long period of time.
A tracheostomy is a major surgical procedure with potential risks and complications. These may include infection, bleeding, damage to the trachea or surrounding tissues, and difficulty speaking or swallowing. Additionally, tracheostomy care, including cleaning and changing the tracheostomy tube, requires training and diligence to prevent complications such as infection or tube obstructions. After a tracheostomy, many patients require rehabilitation to return to their previous lifestyle. This often includes learning to speak and swallow again, as well as training on how to clean and care for the tracheostomy site and tube. Despite the challenges, many people with tracheostomies lead full and active lives.
Advancements in tracheostomy tube design have made them more comfortable and safer for long-term use. A tracheostomy is a significant surgical intervention primarily used to secure the airway in patients who cannot breathe independently or have a blockage in the upper airway. Although it comes with risks, this procedure can significantly improve the quality of life and survival chances for patients in critical conditions or with long-term illnesses.
💥Tracheostomy Tubes [Full Guide] ➜ ➜ ➜ https://bit.ly/33gFyCi
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
030 - Tracheostomy Procedure
1:01 - Emergency Tracheostomies
1:12 - Planned Tracheostomies
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#respiratorytherapy #respiratorytherapist #respiratorytherapyschool
14
views
FEV1/FVC Ratio (Medical Definition) | Quick Explainer Video
What is the FEV1/FVC Ratio? This video covers the medical definition and provides a brief overview of this topic.
💥Pulmnoary Function Testing [Full Guide] ➜ ➜ ➜ https://bit.ly/2A8ZuvQ
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
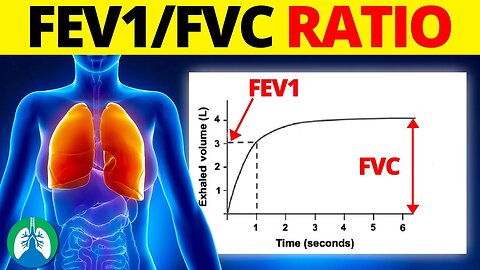
Forced vital capacity (FVC) refers to the maximum volume of air a person can forcibly exhale after a full inhalation. This measure provides a comprehensive assessment of pulmonary capacity, including both large and small airways.
Forced expiratory volume in one second (FEV1) measures the amount of air a person can forcibly exhale in just one second after taking a deep breath. This value is more reflective of the function of the large airways.
➡️ FEV1/FVC Ratio
The FEV1/FVC ratio is calculated by dividing the FEV1 value by the FVC value. It is usually represented as a percentage, and the normal range typically lies between 70% and 80% in adults, though it can vary slightly based on factors like age, sex, ethnicity, and height. If a person's FEV1/FVC ratio is lower than the normal reference range, it may indicate the presence of an obstructive lung disease, such as asthma or chronic obstructive pulmonary disease (COPD). This is because these diseases cause airway obstruction, leading to a reduction in the volume of air that can be expelled in the first second of forced expiration, thereby reducing the FEV1/FVC ratio. Conversely, in restrictive lung diseases like pulmonary fibrosis or sarcoidosis, both FEV1 and FVC may be reduced, but the ratio often remains normal or even increases. This is due to the fact that in restrictive diseases, the lungs are often stiff or smaller, leading to a decrease in total lung capacity, but the airways aren't necessarily obstructed, allowing the FEV1/FVC ratio to remain within the normal range.
It's important to note that the FEV1/FVC ratio is just one measure in pulmonary function testing. While it is valuable, it does not provide a full picture of lung health on its own. Other tests and measures, such as total lung capacity (TLC), residual volume (RV), and diffusing capacity of the lungs for carbon monoxide (DLCO), are often used in conjunction with the FEV1/FVC ratio to provide a comprehensive view of lung function. Furthermore, any abnormal results should be interpreted in conjunction with clinical history and examination findings for accurate diagnosis and management. The FEV1/FVC ratio is a crucial clinical tool in the diagnosis and monitoring of lung diseases. Its usefulness lies not only in its ability to help differentiate between obstructive and restrictive lung diseases but also in the role it plays in the broader context of comprehensive pulmonary function testing.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:30 - Forced Vital Capacity (FVC)
0:47 - Forced Expiratory Volume in One Second (FEV1)
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#FEV1 #FVC #pulmonaryfunctiontesting
37
views
Venous Admixture (Medical Definition) | Quick Explainer Video
What is Venous Admixture? This video covers the medical definition and provides a brief overview of this topic. ✔️
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
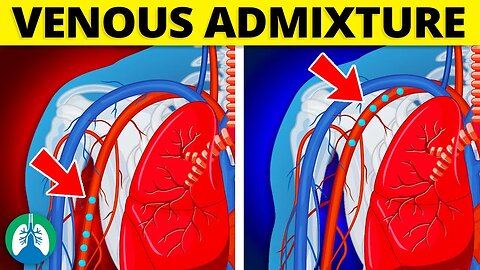
In a healthy individual, blood with low oxygen content flows from the right side of the heart to the lungs, where it picks up oxygen from the inhaled air and releases carbon dioxide. The oxygenated blood then returns to the left side of the heart, from where it is pumped into the systemic circulation to supply the body's tissues with oxygen.
➡️ Venous Admixture
Venous admixture occurs when there are anatomical or functional abnormalities in the pulmonary circulation that allow deoxygenated blood to bypass the lungs and mix with oxygenated blood. This could be due to a variety of causes, including ventilation-perfusion mismatch, intracardiac or intrapulmonary shunts, or lung diseases that compromise the oxygenation process.
Congestive heart failure (CHF) with low cardiac output is another common cause, which is typically related to some type of V/Q mismatch. CHF impairs the heart's ability to pump blood effectively, leading to fluid accumulation in the lungs and other areas of the body.
This fluid accumulation can cause several changes in the lungs, such as:
- Impaired gas exchange
- Hypoxemic vasoconstriction
- Increased pulmonary capillary pressures
These factors combine to promote venous admixture in CHF patients, resulting in hypoxemia and decreased arterial oxygenation. Treatment strategies for CHF typically focus on improving cardiac function, reducing fluid accumulation, and alleviating symptoms, which can help mitigate the impact of venous admixture in these patients. Increased venous admixture leads to a reduction in the overall oxygen content of the arterial blood, which may contribute to hypoxemia (i.e., low blood oxygen levels). This is clinically significant, particularly in patients with pre-existing respiratory or cardiovascular diseases, and requires further investigation and treatment.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:50 - Venous Admixture
1:15 - Congestive Heart Failure
1:35 - Fluid Accumulation
1:58 - Treatment
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#VenousAdmixture #bloodflow #gasexchange
31
views
Do THIS to Prevent AFib Before It's too Late ❗️
Atrial Fibrillation (AFib) is a significant risk factor for stroke and heart disease. Watch this video to learn how to minimize the risk of developing AFib and lead a heart-healthy life.
💥How to Prevent AFib [Full Guide] ➜ ➜ ➜ https://bit.ly/3NTzI0j
🟦 More Videos You Might Like:
▪ Flush Fat Out of Your Arteries ➜ https://youtu.be/JfQDVnSAtis
▪ Best Vitamins to Prevent a Heart Attack ➜ https://youtu.be/bT0fT6c2TUc
▪ Best Herbs to Clean Your Arteries ➜ https://youtu.be/5hQXG7nmd90
➡️ Eat a Healthy Diet
A healthy diet is the cornerstone of preventing many health conditions, including atrial fibrillation (AFib). Consuming a balanced diet rich in fruits, vegetables, whole grains, lean proteins, and healthy fats can help control blood pressure and cholesterol levels, which are key risk factors for AFib.
➡️ Exercise
Regular physical activity is another crucial factor in preventing AFib. Exercise helps in maintaining a healthy heart rate, managing weight, reducing stress, and controlling blood pressure. Moderate-intensity exercise, such as brisk walking, swimming, or biking, for at least 30 minutes a day, five days a week, can significantly lower your risk of developing AFib.
➡️ Maintain Your Body Weight
Being overweight or obese increases the risk of AFib. Excess weight can put a strain on your heart, leading to a higher risk of AFib and other heart-related conditions. Weight maintenance is achieved through a combination of healthy eating and regular physical activity.
➡️ Avoid Alcohol
Excessive alcohol consumption can trigger episodes of AFib, as it may increase your heart rate and lead to high blood pressure. It's recommended that women have no more than one drink per day and men have no more than two.
➡️ Quit Smoking
Smoking is one of the leading risk factors for many cardiovascular diseases, including atrial fibrillation (AFib). The chemicals in tobacco smoke can damage the structure and function of your heart and blood vessels, leading to a higher risk of AFib. Quitting smoking can significantly lower your risk.
➡️ Manage Your Diabetes
Diabetes, particularly when poorly managed, increases the risk of AFib. High blood sugar levels can lead to damage in the blood vessels and nerves that control the heart, increasing the chance of heart diseases.
(Watch the video for more)
💥How to Prevent AFib [Full Guide] ➜ ➜ ➜ https://bit.ly/3NTzI0j
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:41 - Eat a Healthy Diet
1:19 - Exercise
1:55 - Maintain Your Body Weight
2:22 - Avoid Alcohol
2:56 - Quit Smoking
3:32 - Manage Your Diabetes
4:00 - Manage Stress
4:35 - Get Quality Sleep
5:18 - Stay Hydrated
5:45 - Limit Caffeine
6:19 - Limit Sodium
6:46 - Cold Exposure
7:25 - Eat More Potassium
8:01 - Valsalva Maneuver
8:34 - Belly Breathing
9:02 - Acupuncture
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#afib #atrialfibrillation #heartattackprevention
177
views
Endotracheal Suctioning? (TMC Practice Question)
The video breaks down a sample TMC practice question about a patient who is on a ventilator and receives endotracheal suctioning. Do you know what to expect?
💥TMC Test Bank [Practice Questions] ➜ ➜ ➜ https://bit.ly/3QNqwLX
💥Daily Practice Questions [via Email] ➜ ➜ ➜ http://bit.ly/2NnXh3C
➡️ Question
A 70-year-old male patient is intubated and receiving mechanical ventilation in the volume-controlled A/C mode. After performing endotracheal suctioning, which of the following would indicate the effective clearance of retained secretions?
A. An increased tidal volume
B. A decreased inspiratory time
C. A decreased plateau pressure
D. A decreased peak pressure
In general, you should remember that retained secretions will increase the patient’s airway resistance and peak airway pressure during volume-controlled ventilation. So, taking that into consideration, if you were to clear the secretions via suctioning, that should decrease the patient’s peak airway pressure. On the other hand, if the patient had been receiving pressure-controlled ventilation, you would expect an increase in delivered volume once the secretions were cleared. That is the key tidbit that you needed to recognize in order to answer this question correctly. In other words, you needed to understand the difference between volume and pressure-controlled ventilation.
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:27 - Practice Question
0:59 - Explanation
1:44 - Correct Answer
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#respiratorytherapyzone #tmcexam #tmcpracticequestion
11
views
Tachypnea, Tracheal Deviation, and Hyperresonance? (TMC Practice Question)
The video breaks down a sample TMC practice question about a patient with tachypnea, tracheal deviation, and hyperresonance. Do you know what this means?
💥TMC Test Bank [Practice Questions] ➜ ➜ ➜ https://bit.ly/3QNqwLX
💥Daily Practice Questions [via Email] ➜ ➜ ➜ http://bit.ly/2NnXh3C
➡️ Question
An adult patient who is receiving mechanical ventilation suddenly started showing signs of tachypnea. Upon assessment, you noticed tracheal deviation to the right and decreased breath sounds and hyperresonance on the left side. Which of the following would you recommend?
A. Endotracheal suctioning
B. Flexible bronchoscopy
C. The insertion of a chest tube
D. Thoracentesis
For this question, you needed to be able to interpret the signs and symptoms that were given in the question. And by doing so, you could easily determine that all of the signs are consistent with a pneumothorax. Remember: Patients with a pneumothorax will typically show signs of tracheal deviation away from the affected side. They will also have decreased breath sounds and hyperresonance on the affected side. Therefore, to treat a pneumothorax, you should recommend the immediate insertion of a chest tube on the affected side.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:21 - Practice Question
0:53 - Explanation
1:29 - Correct Answer
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#respiratorytherapyzone #tmcexam #tmcpracticequestion
9
views
Eupnea (Medical Definition) | Quick Explainer Video
What is Eupnea? We created this video to cover the medical definition and provide a brief overview of this topic.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
➡️ Eupnea
Eupnea involves a complicated interplay between various body systems. In particular, it requires coordination between the respiratory, cardiovascular, and nervous systems. The rhythm and depth of eupneic breathing are determined by the body's need to remove carbon dioxide (CO2), a waste product of metabolism, and replace it with oxygen (O2). A normal resting respiratory rate in healthy adults ranges from 12 to 20 breaths per minute, although this may vary depending on the individual's age, fitness level, and overall health status.
➡️ How it Works
One fascinating aspect of eupnea is that it operates mostly under subconscious control, directed by the autonomic nervous system. The medulla oblongata, a part of the brain stem, plays a crucial role in this regulation. It responds to changes in blood levels of CO2, O2, and pH, signaled by chemoreceptors located in the carotid arteries and aorta. When CO2 levels rise, or O2 levels fall, the medulla initiates a response to increase the rate and depth of respiration in order to maintain homeostasis. The complexity of eupnea is underscored when it's disrupted, such as in disease states.
➡️ Dyspnea
Dyspnea, the sensation of breathlessness, is a common symptom of many medical conditions, including chronic obstructive pulmonary disease (COPD), asthma, pneumonia, and heart failure. These conditions alter the mechanics of breathing, the exchange of gases, or the neural control mechanisms that regulate respiration, leading to increased effort to breathe, and hence a departure from the state of eupnea. In addition, it is noteworthy that eupnea is not a static state. Our bodies adjust our breathing patterns to meet changing physiological demands. For instance, during physical exercise, the need for oxygen increases, resulting in a more rapid and deeper breathing pattern, which is referred to as hyperpnea. Similarly, emotional states like anxiety or fear can trigger hyperventilation, a state of over-breathing, while sleep results in a decrease in breathing rate and depth, often referred to as hypoventilation.
Eupnea, the state of normal, restful breathing, is a critical yet often overlooked aspect of our bodily functions. It ensures the optimal exchange of gases, supports metabolic processes and helps maintain the body's internal balance. Given the intricate mechanics and neural control involved, it also serves as a remarkable testament to the body's complexity and adaptability. Understanding the underlying principles of eupnea not only helps us appreciate this everyday miracle but also sheds light on a variety of health conditions when this process is interrupted.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:35 - Eupnea
0:54 - Normal Respiratory Rate
1:44 - Complexity
1:51 - Dyspnea
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#breathing #breathingpatterns #eupnea
28
views
Boost Your Lung Health with THESE Essential Oils! 🫁
This video takes a closer look at the best essential oils for breathing and lung support, including how they can be used to improve respiratory health.
💥Best Essential Oils for Breathing [Full Guide] ➜ ➜ ➜ https://bit.ly/2yTxLP5
🟦 Types of Essential Oils (affiliate links) for Breathing:
-- Black Seed Oil: https://amzn.to/3DOyKOc
-- Eucalyptus Oil: https://amzn.to/3DNcjJq
-- Bergamot Oil: https://amzn.to/3qlDbNA
-- Ginger Oil: https://amzn.to/3OLAdLt
-- Mullein Extract: https://amzn.to/43XYFOb
-- Turmeric Oil: https://amzn.to/43V6mEJ
-- Peppermint Oil: https://amzn.to/3KwdKQm
-- Elderberry Extract: https://amzn.to/440h9h7
-- Astragalus Extract: https://amzn.to/3qmqT7z
-- Rosemary Oil: https://amzn.to/3DNHzbm
-- Lavender Oil: https://amzn.to/3ONd7nZ
-- Cardamom Oil: https://amzn.to/44YwG2g
-- Oregano Oil: https://amzn.to/3rUGICK
-- Thyme Oil: https://amzn.to/47fqeFw
-- Nettle Leaf Extract: https://amzn.to/3rWCJ8J
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
🟦 Essential Oils and Breathing
Breathing is a fundamental part of our existence, and the health of our lungs is crucial for our overall well-being. As a registered respiratory therapist (RRT), helping patients breathe easier has been my primary focus since 2016. While there are many factors that can affect lung health, from pollution to genetics, one area that has been gaining attention in recent years is the use of essential oils. Essential oils are concentrated plant extracts that have been used for thousands of years for their medicinal properties. In this video, we’ll explore some of the best essential oils for breathing and lung support, including how they can be used to improve respiratory health. Whether you’re dealing with asthma, allergies, or just looking for ways to enhance your lung function, these essential oils may provide some relief and help you breathe easier.
💥Best Essential Oils for Breathing [Full Guide] ➜ ➜ ➜ https://bit.ly/2yTxLP5
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
—————
⏰TIMESTAMPS
0:00 - Intro
0:38 - Black Seed Oil
1:12 - Eucalyptus Oil
1:52 - Bergamot Oil
2:35 - Ginger Oil
3:13 - Mullein Extract
3:47 - Turmeric Oil
4:13 - Peppermint Oil
4:36 - Elderberry Extract
5:00 - Astragalus Extract
5:37 - Rosemary Oil
6:17 - Lavender Oil
6:49 - Cardamom Oil
7:13 - Oregano Oil
7:54 - Thyme Oil
8:40 - Nettle Leaf Oil
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#essentialoils #lunghealth #lungdetox
71
views
Decreased Lung Compliance? (TMC Practice Question)
The video breaks down a sample TMC practice question about what happens when a patient's lung compliance decreases. Can you guess the correct answer?
💥TMC Test Bank [Practice Questions] ➜ ➜ ➜ https://bit.ly/3QNqwLX
💥Daily Practice Questions [via Email] ➜ ➜ ➜ http://bit.ly/2NnXh3C
➡️ Question
A 63-year-old female patient is intubated and receiving mechanical ventilation in the pressure-controlled A/C mode. If the patient’s compliance were to decrease, which of the following would you expect to occur?
A. The delivered volume will decrease
B. The peak pressure will increase
C. The inspiratory time will increase
D. The PEEP level will decrease
To get this one correct, you needed to have a basic understanding of lung compliance. You also needed to recognize that the pressure level is preset because the ventilator is in a pressure-controlled mode. If there is a decrease in lung compliance when the ventilator is operating in the pressure control mode, the machine will continue delivering a constant pressure. But, since the lungs don’t expand as much when there is decreased compliance, it reaches the preset pressure limit much faster. This means that there will be a decrease in the delivered tidal volume. Also, in this case, the inspiratory time would decrease, and the PEEP levels would not be affected.
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:23 - Practice Question
0:51 - Explanation
1:40 - Correct Answer
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#respiratorytherapyzone #tmcexam #tmcpracticequestion
12
views
Pre and Post-Bronchodilator Test (TMC Practice Question)
The video breaks down a sample TMC practice question about administering a pre and post-bronchodilator test. Do you know what to look for?
💥TMC Test Bank [Practice Questions] ➜ ➜ ➜ https://bit.ly/3QNqwLX
💥Daily Practice Questions [via Email] ➜ ➜ ➜ http://bit.ly/2NnXh3C
➡️ Question
A pre and post-bronchodilator test was ordered on a 48-year-old female patient. The forced expiratory measurement that was obtained after the bronchodilator shows an increase in the patient’s FEV1 from 60% to 80% of the predicted value. This suggests which of the following?
A. Fixed airway obstruction
B. Reversible airway obstruction
C. Normal diffusion capacity
D. Restrictive process
The information given in the question suggests that the patient’s airway obstruction was somewhat relieved after the bronchodilator was given. We know this because their FEV1 increased from 60% to 80% of the predicted value. Was the increase enough to classify it as a reversible obstruction? Remember: If the patient's pre-to-post values increase by at least 12%, you know that the treatment was effective. So, in this case, there was a 20% increase, which means that; yes, the improvement was enough to interpret the patient’s condition as a reversible airway obstruction.
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:36 - Question
1:06 - Explanation
1:53 - Correct Answer
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#respiratorytherapyzone #tmcexam #tmcpracticequestion
18
views
Vallecula (Medical Definition) | Quick Explainer Video
What is Vallecula? We created this video to cover the medical definition and provide a brief overview of this topic.
💥Vallecula [Full Guide] ➜ ➜ ➜ http://bit.ly/3LzpRxm
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
➡️ Vallecula
The vallecula is a small, depression-like structure found within the oropharynx. The oropharynx is part of the pharynx, which is a muscular tube that connects the nasal and oral cavities to the larynx and esophagus. The vallecula is situated between the base of the tongue and the epiglottis, a flap-like structure that serves as a gatekeeper for the airways. The vallecula is divided into two distinct spaces known as the valleculae epiglotticae. These folds are created by mucus membrane-covered connective tissue and contain underlying minor salivary glands. Though hidden from the naked eye, the vallecula plays an essential role in the human body. Its location allows it to trap saliva and occasionally food, preventing the swallowing reflex from being constantly triggered, especially during sleep.
➡️ Function
The primary function of the vallecula is to facilitate the swallowing process. When food or liquid is ingested, the tongue pushes the bolus (i.e., chewed food mass) toward the back of the oral cavity. As it reaches the vallecula, the epiglottis folds down, sealing off the larynx and ensuring the bolus moves into the esophagus instead of the trachea. This mechanism prevents choking and aspiration, protecting the airway during swallowing.
➡️ Clinical Relevance
The vallecula is an important anatomical landmark for healthcare professionals, particularly in airway management and endotracheal intubation. During intubation, a tube is inserted through the mouth or nose and into the trachea to maintain a patent airway to facilitate mechanical ventilation. The vallecula serves as a guide, allowing practitioners to properly position the laryngoscope blade, visualize the vocal cords, and subsequently insert the endotracheal tube. In some cases, abnormalities or pathologies affecting the vallecula can lead to dysphagia (i.e., difficulty swallowing), aspiration, or other complications.
Conditions such as tumors, inflammation, infections, or congenital deformities can impact the structure and function of the vallecula, resulting in the need for medical intervention. Therefore, the early detection and appropriate treatment of these conditions can significantly improve patient outcomes and prevent further complications.
Moreover, the vallecula may be implicated in certain sleep disorders, such as obstructive sleep apnea (OSA). This occurs when the airway becomes partially or completely blocked during sleep, leading to disrupted breathing and reduced oxygen levels. In some individuals, an enlarged tongue base or abnormalities in the vallecula may contribute to airway obstruction, and surgical interventions targeting these structures may help alleviate symptoms in selected cases.
💥Vallecula [Full Guide] ➜ ➜ ➜ http://bit.ly/3LzpRxm
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:29 - Vallecula
0:36 - Oropharynx
1:28 - Function
2:00 - Clinical Relevance
3:05 - OSA
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#respiratorytherapy #respiratorytherapist #Vallecula
26
views
Cuff Pressure Assessment (TMC Practice Question)
The video breaks down a sample TMC practice question about making adjustments to a patient's cuff pressure. Do you know the normal range?
💥TMC Test Bank [Practice Questions] ➜ ➜ ➜ https://bit.ly/3QNqwLX
💥Daily Practice Questions [via Email] ➜ ➜ ➜ http://bit.ly/2NnXh3C
➡️ Question
A 50-year-old male patient is intubated with a size 8 endotracheal tube and is receiving volume-controlled A/C ventilation. Upon assessment, you note that the patient’s cuff pressure is measured at 38 cmH2O. Which of the following would you recommend?
A. Withdraw the tube 1–2 cm and reassess the patient’s breath sounds
B. Recommend reintubation with a smaller endotracheal tube
C. Lower the cuff pressure to less than 30 cmH2O
D. Recommend ventilation via a tracheostomy
To get this one correct, you needed to know the normal values for cuff pressure. And in this case, you needed to recognize that 38 cmH2O is way too high and could potentially be dangerous for the patient. Therefore, your first action should be to lower the cuff pressure to less than 30 cmH2O and then check to ensure there are no leaks. For the TMC Exam, you must remember that the normal range for cuff pressure is between 20–30 cmH2O. In this case, there is no indication to withdraw the tube, and using a smaller tube would only cause the patient’s peak pressure to increase, which is something that we do not want. Furthermore, there is nothing in the question that suggests a tracheostomy is indicated, so we can rule that one out as well.
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:27 - Practice Question
1:05 - Explanation
1:57 - Correct Answer
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#respiratorytherapyzone #tmcexam #tmcpracticequestion
9
views
Ventricular Tachycardia (V-tach) | Medical Explainer Video
What is Ventricular Tachycardia (V-tach)? We created this video to cover the medical definition and provide a brief overview of this topic.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
➡️ Ventricular Tachycardia
The rhythm disturbance in ventricular tachycardia can occur due to various reasons. It is often associated with underlying heart diseases like coronary artery disease, cardiomyopathy, heart valve disease, and congenital heart disease. Certain medications, high levels of adrenaline due to severe stress, electrolyte imbalances, or recreational drug use can also trigger V-tach. In rare cases, V-tach may occur in individuals without apparent heart disease.
➡️ Types
Ventricular tachycardia may be classified as sustained or non-sustained. Sustained V-tach lasts for more than 30 seconds or requires intervention to terminate due to severe symptoms. Non-sustained V-tach stops spontaneously within 30 seconds and is typically less symptomatic.
➡️ Symptoms
The symptoms associated with V-tach can range from palpitations, lightheadedness, and shortness of breath, to severe manifestations such as loss of consciousness or cardiac arrest, especially in the case of sustained V-tach. However, it's essential to note that not all individuals with V-tach exhibit noticeable symptoms. The condition may be detected incidentally during routine health checkups or heart examinations for other reasons. Electrocardiogram (ECG), Holter monitor, event monitor, and implantable loop recorder are some diagnostic tools used to detect and analyze the nature of the abnormal heart rhythm. Management of ventricular tachycardia is crucial given its potential life-threatening nature.
➡️ Treatment
Treatment options primarily focus on restoring the normal heart rhythm, controlling the rate of rapid heartbeats when an episode occurs, preventing future episodes, and minimizing complications. Antiarrhythmic medications, implantable cardioverter-defibrillator (ICD) placement, cardiac ablation, and in severe cases, surgery may also be employed. Ventricular tachycardia is a serious cardiac condition that requires timely recognition and appropriate management to prevent major cardiovascular complications and improve survival. Regular follow-ups with a cardiologist are necessary for patients diagnosed with V-tach to ensure optimal heart health.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
1:04 - Ventricular tachycardia
1:10 - Sustained V-tach
1:18 - Non-sustained V-tach
1:26 - Symptoms
1:58 - ECG
2:17 - Treatment
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#respiratorytherapy #respiratorytherapist #VentricularTachycardia
51
views
Fever (Medical Definition) | Quick Explainer Video
What is Fever? We created this video to cover the medical definition and provide a brief overview of this topic.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
➡️ Fever
The human body operates within a very tightly controlled range of temperatures, typically around 97.7 to 99.5 degrees Fahrenheit. Any change from this narrow range can disrupt the body's various metabolic processes. Fever usually occurs when the body's thermostat, located in the hypothalamus, gets reset to a higher temperature due to various factors. This increased set point triggers processes such as muscle contraction (shivering) and increased metabolism to produce more heat and maintain the higher temperature.
➡️ Symptoms
Fever is often associated with other symptoms such as headache, sweating, chills, muscle aches, weakness, and loss of appetite. The fever itself is not a disease but is usually a symptom of an underlying condition. As such, treatment usually involves addressing the underlying cause. However, in situations where the fever is causing discomfort or is dangerously high, medications such as acetaminophen or ibuprofen may be used to lower the body temperature. While fever often indicates a common illness like a cold or flu, it can also be a symptom of more serious conditions such as pneumonia, meningitis, or sepsis.
A persistent fever could also indicate an ongoing bacterial or viral infection, an autoimmune disease, or even certain types of cancer. In children, fever can often cause anxiety for parents, but it is important to remember that fever is the body's natural response to infection. However, extremely high fever, especially when accompanied by other symptoms like difficulty breathing, severe headache, or a stiff neck, can be a sign of a potentially serious condition and should prompt immediate medical attention.
➡️ Benefits
A fever can be beneficial as well. The increase in body temperature can speed up the activity of the immune system, making it more efficient at fighting off infections. In some cases, a fever may be intentionally induced as a form of treatment. This approach, known as pyrotherapy, was once used in the treatment of certain diseases, such as syphilis, before the advent of antibiotics.
Fever is a complex response of the body to a variety of conditions, most commonly infections. While it can be a cause for concern, especially if it is high or persistent, it is typically a beneficial sign that the body is actively fighting off an illness. Its management should focus not only on the fever itself but, more importantly, on identifying and treating its underlying cause.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
1:05 - Other Symptoms
1:49 - Ongoing Infection
2:26 - Benefits
2:55 - Complex Response
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#respiratorytherapy #respiratorytherapist #fever
40
views
Vital Capacity (VC) | Medical Explainer Video
What is Vital Capacity? We created this video to cover the medical definition and provide a brief overview of this topic.
💥Pulmonary Function Testing [Full Guide] ➜ ➜ ➜ https://bit.ly/2A8ZuvQ
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
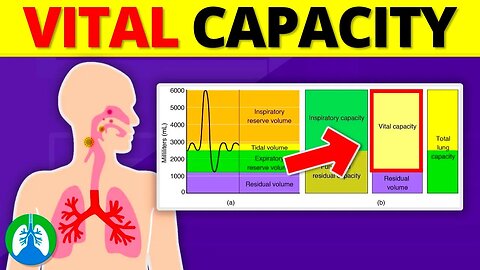
➡️ Vital Capacity
Vital capacity is a key measurement in pulmonary function testing, reflecting the maximum volume of air a person can forcibly exhale after a maximum inspiration. It is often measured in conjunction with other pulmonary function tests to assess a patient's respiratory health or to monitor the progression of diseases like asthma or chronic obstructive pulmonary disease (COPD).
➡️ Vital Capacity Volumes
-- Tidal volume (VT): The amount of air inhaled or exhaled during normal breathing.
-- Inspiratory reserve volume (IRV): The maximum amount of air that can be inhaled after a normal inhalation.
-- Expiratory reserve volume (ERV): The maximum amount of air that can be exhaled after a normal exhalation.
The sum of these three volumes equals the vital capacity. The actual values can vary depending on a number of factors, including a person's age, sex, height, and overall health. For example, taller individuals usually possess a larger vital capacity due to greater lung size, while certain health conditions, such as COPD, can significantly decrease it.
➡️ Spirometry
Vital capacity is measured using a device called a spirometer. During a spirometry test, the patient takes the deepest breath they can and then exhales as much as they can into the device. The spirometer records the total amount of air exhaled, which represents the person's vital capacity. In the field of respiratory care, vital capacity is used for various purposes. It can be a part of preoperative assessment, evaluating whether patients are fit for surgeries, especially those requiring general anesthesia. For people with respiratory diseases, it serves as an important metric to monitor disease progression and response to therapy.
Moreover, in occupational health, it assists in determining fitness for jobs that require significant physical effort, particularly those needing effective respiratory function. In essence, vital capacity is not only a measure of respiratory function, but it is also a vital tool in the early detection of restrictive or obstructive lung diseases. It supports the development of therapeutic strategies and the monitoring of treatment efficacy. Thus, understanding and assessing vital capacity plays an indispensable role in maintaining respiratory health and overall well-being.
💥Pulmonary Function Testing [Full Guide] ➜ ➜ ➜ https://bit.ly/2A8ZuvQ
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:29 - Vital Capacity
0:51 - Composition
0:56 - Tidal volume (VT)
1:01 - Inspiratory reserve volume (IRV)
1:09 - Expiratory reserve volume (ERV)
1:47 - Vital Capacity Measured
2:38 - Occupational Health
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#pulmonaryfunctiontesting #vitalcapacity #respiratorytherapyschool
15
views
Bubble Humidifier Making a Whistling Noise? (TMC Practice Question)
The video breaks down a sample TMC practice question about a bubble humidifier that is making a whistling noise. What is the primary cause?
💥TMC Test Bank [Practice Questions] ➜ ➜ ➜ https://bit.ly/3QNqwLX
💥Daily Practice Questions [via Email] ➜ ➜ ➜ http://bit.ly/2NnXh3C
➡️ Question
During the assessment of a 52-year-old female patient who is receiving oxygen via nasal cannula at 4 L/min, you hear the bubble humidifier making a whistling noise. What is the most likely cause of this finding?
A. There is an obstruction in the delivery tube
B. The patient’s ventilation has increased
C. There is a clogged system diffuser
D. The flowmeter pressure is set too high
If you’ve ever accidentally stepped on the tubing of a bubble humidifier while being used, you will automatically recognize that the correct answer is A. The relief valve of a bubble humidifier was designed to sound whenever the pressure in the reservoir container exceeds the valve’s threshold pressure, resulting in a loud, whistling noise. And, of course, the most common reason for this to occur is when there is a downstream obstruction to outflow.
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:23 - Practice Question
0:55 - Explanation
1:25 - Correct Answer
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#respiratorytherapyzone #tmcexam #tmcpracticequestion
19
views
Ventricular Fibrillation (V-fib) | Medical Explainer Video
What is Ventricular Fibrillation (V-fib)? We created this video to cover the medical definition and provide a brief overview of this topic.
💥EKG Interpretation [Full Guide] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
➡️Ventricular Fibrillation (V-fib)
Ventricular fibrillation is triggered when a problem in the heart's electrical system causes disorganized electrical signals to be sent across the ventricles. Instead of a coordinated, rhythmic contraction, the ventricular muscle fibers twitch randomly and out of sync. This results in a fast and irregular heart rhythm, which can be fatal if not treated immediately.
V-fib is considered a medical emergency because it can lead to sudden cardiac arrest and death. It is the most frequent cause of sudden cardiac death, with individuals often having no warning signs. If V-fib occurs, the individual will collapse within seconds and won't have a pulse.
➡️ Several factors increase the risk of developing V-fib, including:
- Previous heart attack
- History of heart disease
- Specific changes in heart structure
- Certain heart medications
- Stimulant or drug misuse
Other conditions such as hypoxemia, sepsis, hypothermia, or severe electrolyte imbalances can also predispose an individual to this arrhythmia. Ventricular fibrillation is confirmed with an electrocardiogram (ECG), which provides a recording of the heart's electrical activity. Emergency treatment aims to restore the heart's normal rhythm and involves cardiopulmonary resuscitation (CPR), defibrillation, and administration of certain medications. Defibrillation is required for this arrhythmia and involves sending an unsynchronized shock to the patient's heart. Remember that defibrillation is always recommended for life-threatening arrhythmias, including:
For those at a high risk of V-fib, preventative measures might include medication to control the heart rhythm or a device implant, like an implantable cardioverter-defibrillator (ICD), which continuously monitors the heart rhythm and delivers electric shocks if necessary to control arrhythmias. Ventricular fibrillation is a severe, life-threatening cardiac condition resulting from disorganized electrical activity in the heart's ventricles. It requires immediate medical attention, and if left untreated, it often leads to sudden cardiac death. Nonetheless, with rapid response and proper medical care, many people survive V-fib and can live healthy lives with appropriate treatment and management.
💥EKG Interpretation [Full Guide] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:34 - Ventricular fibrillation
0:59 - Considered Medical Emergency
1:20 - Several Factors
1:47 - ECG
2:16 - Ventricular fibrillation (V-fib)
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#respiratorytherapy #respiratorytherapist #ventricularfibrillation
93
views
Top Early Warning Signs of COPD *MUST KNOW* ⚠️
What are the early warning signs of COPD? What symptoms should you look for? Watch this video to find out!
💥COPD Early Warning Signs [Full Guide] ➜ ➜ ➜ https://bit.ly/3mQaFC1
💥Asthma Early Warning Sings [Full Guide] ➜ ➜ ➜ https://bit.ly/3N6Bb4P
➡️ Shortness of Breath
One of the earliest and most common warning signs of COPD is shortness of breath (i.e., dyspnea). This can occur during everyday activities, such as climbing stairs, walking, or getting dressed. As the disease progresses, shortness of breath may occur even at rest, making it increasingly challenging to carry out daily tasks.
➡️ Coughing Up Sputum
COPD can cause an increase in mucus production, leading to the frequent need to clear the throat and cough up secretions.
➡️ Wheezing
Wheezing is a high-pitched, whistling sound that usually occurs during exhalation. It is caused by narrowing or obstruction of the airways, which is common in COPD as the lungs become inflamed and the airways constrict.
➡️ Chest Tightness
People with COPD may experience a sensation of chest tightness or pressure, making it difficult to take a deep breath. This feeling is often the result of inflamed and constricted airways or the buildup of mucus in the lungs.
➡️ Fatigue or General Weakness
This can be due to decreased oxygen levels in the blood, which can affect overall energy levels and the body's ability to perform everyday activities.
➡️ Recurring Lung Infections
People with COPD are more susceptible to lung infections, such as pneumonia or bronchitis. These recurring infections can further damage the lungs and worsen COPD symptoms.
➡️ Swollen Ankles From Fluid Build-Up
Swelling in the ankles, feet, or legs, known as peripheral edema, can be a sign of COPD. This occurs when the disease begins to affect the heart's ability to pump blood effectively, leading to fluid build-up in the lower extremities.
➡️ Chronic Cough
Often referred to as a "smoker's cough," this symptom can be dry or accompanied by mucus production. The cough is usually worse in the morning and may be triggered by environmental irritants like smoke, dust, or cold air.
➡️ Difficulty Taking a Deep Breath
COPD can make it challenging to take a deep breath due to inflammation, mucus buildup, and narrowing of the airways. This difficulty can result in decreased oxygen intake, leading to other symptoms such as fatigue and shortness of breath.
💥COPD Early Warning Signs [Full Guide] ➜ ➜ ➜ https://bit.ly/3mQaFC1
💥Asthma Early Warning Sings [Full Guide] ➜ ➜ ➜ https://bit.ly/3N6Bb4P
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:41 - Shortness of Breath
1:08 - Coughing Up Sputum
1:22 - Wheezing
1:40 - Chest Tightness
2:00 - Fatigue or General Weakness
2:16 - Recurring Lung Infections
2:32 - Swollen Ankles From Fluid Build-Up
2:53 - Chronic Cough
3:12 - Difficulty Taking a Deep Breath
3:35 - Cyanosis
3:55 - Barrel Chest
4:24 - Rapid Breathing
4:38 - Reduced Appetite and Weight Loss
5:00 - Pale, Sweaty Face
5:17 - Insomnia
5:33 - Hypoxemia
6:00 - Fever
6:22 - Difficulty Speaking Due to a Lack of Air
6:43 - Feelings of Confusion
7:01 - Feelings of Anxiety and Panic
7:21 - Posture Changes
7:46 - Exercise Intolerance
8:10 - Itching of the Chin or Neck
8:26 - Dizziness
8:48 - Dry Mouth
9:05 - Decrease in Peak Flow Reading
9:30 - Increased Need for Inhaler Use
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#COPD #COPDwarningsigns #copdtreatment
177
views
Breathing Asynchronously with the Ventilator (TMC Practice Question)
The video breaks down a sample TMC practice question about a patient who is breathing asynchronously with the mechanical ventilator. Do you know the correct answer?
💥TMC Test Bank [Practice Questions] ➜ ➜ ➜ https://bit.ly/3QNqwLX
💥Daily Practice Questions [via Email] ➜ ➜ ➜ http://bit.ly/2NnXh3C
➡️ Question:
A 58-year-old female patient is intubated and appears to be breathing asynchronously with the ventilator. Her breath sounds are absent on the left side, and the trachea is shifted to the left. The patient has a dull percussion note on the left side as well. Which of the following is the most likely explanation for these findings?
A. A tracheoesophageal fistula has developed
B. A tension pneumothorax has developed on the left side
C. The endotracheal tube is in the right mainstem bronchus
D. The patient is experiencing diffuse bronchospasm
To get this one correct, you needed to be able to interpret the information that was provided in the question. It states that the patient has a dull percussion note on the left side, a tracheal shift toward the left side, and absent breath sounds on the left side. Therefore, you needed to recognize that these are all signs of atelectasis. So, now you have to think, "what could possibly be the cause of this atelectasis?" And in this case, the endotracheal tube has likely slipped into the right mainstem bronchus, which has resulted in left-sided atelectasis. Diffuse bronchospasm would cause bilateral wheezing, and a left-sided pneumothorax would cause a hyperresonant percussion note, not a dull percussion note.
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:34 - Practice Question
1:12 - Explanation
2:06 - Correct Answer
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#respiratorytherapyzone #tmcexam #tmcpracticequestion
26
views
Drink THIS Tea for Natural Lung Cleanse and Detox 🍵
What are the best types of tea to drink that can detox and cleanse your lungs and respiratory system? Watch this video to find out!
💥Best Teas for Lungs [Full Guide] ➜ ➜ ➜ http://bit.ly/2plcfO1
💥How to Detox Your Lungs [Full Guide] ➜ ➜ ➜ http://bit.ly/2Mi722t
➡️ Tea for Lungs
Tea has long been known for its various health benefits, from boosting the immune system to aiding digestion. But did you know that certain types of tea can also provide support for lung health? With the increasing levels of air pollution and the prevalence of respiratory illnesses, it’s essential to consider ways to keep our lungs healthy. In this video, we’ll explore some of the best types of tea that can support lung health, including their unique properties and how they may help to alleviate symptoms of respiratory issues. Whether you’re looking for a preventative measure or a natural remedy to support your respiratory system, there’s likely a tea out there that can help.
➡️ Best Types of Tea for Easier Breathing
1. Mullein leaf tea
2. Eucalyptus tea
3. Nettle leaf tea
4. Thyme tea
5. Peppermint tea
6. Green tea
7. Ginger tea
8. Turmeric tea
9. Ginseng tea
10. Elderberry tea
11. Horehound tea
12. Oregano tea
13. Licorice tea
14. Astragalus tea
15. Earl Grey tea
16. Rosemary tea
17. Lavender tea
18. Cardamom tea
19. Marshmallow leaf tea
20. Schisandra tea
21. Yarrow tea
💥Best Teas for Lungs [Full Guide] ➜ ➜ ➜ http://bit.ly/2plcfO1
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:46 - Mullein Leaf Tea
1:30 - Eucalyptus Tea
2:15 - Nettle Leaf Tea
2:59 - Thyme Tea
3:48 - Peppermint Tea
4:30 - Green Tea
5:09 - Ginger Tea
5:51 - Turmeric Tea
6:31 - Ginseng Tea
7:06 - Elderberry Tea
7:45 - Horehound Tea
8:28 - Oregano Tea
9:14 - Licorice Tea
9:47 - Astragalus Tea
10:26 - Earl Grey Tea
11:05 - Rosemary Tea
11:49 - Lavender Tea
12:46 - Cardamom Tea
13:33 - Marshmallow Leaf Tea
14:11 - Schisandra Tea
14:58 - Yarrow Tea
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#lungdetox #lungcleanse #lungtea
107
views
Treating Fever and a Productive Cough (TMC Practice Question)
The video breaks down a sample TMC practice question about treating a patient with signs of fever and a productive cough. What would you recommend?
💥TMC Test Bank [Practice Questions] ➜ ➜ ➜ https://bit.ly/3QNqwLX
💥Daily Practice Questions [via Email] ➜ ➜ ➜ http://bit.ly/2NnXh3C
➡️ Question
A 39-year-old male patient was admitted to the emergency department with a fever and SpO2 of 87% on room air. Upon auscultation, rhonchi is heard, and the patient has a productive cough. Which of the following would you recommend?
A. Intubate and provide mechanical ventilation with 40% oxygen
B. Provide noninvasive positive pressure ventilation using a full face mask
C. Implement postural drainage and percussion with directed coughing
D. Provide oxygen therapy and obtain a sputum sample for culture and sensitivity
To get this one correct, you needed to recognize that the patient has some type of infection (e.g., pneumonia). You know this because the question states that the patient is hypoxemic, has a fever, and has rhonchi on auscultation. So, in this case, you should obtain a sputum sample for culture and sensitivity to identify the type of organism that is present. Additionally, oxygen therapy would be indicated to treat the patient's hypoxemia. Intubation and NPPV would not be indicated in this case, and postural drainage and percussion would also not be recommended.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:30 - Practice Question
1:11 - Explanation
1:50 - Correct Answer
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#respiratorytherapyzone #tmcexam #tmcpracticequestion
12
views
❣️THESE are the Best Vitamins to Prevent a Heart Attack
What are the best vitamins to take to prevent a heart attack and improve your cardiovascular health? Watch this video to find out!
💥Heart Attack Vitamins [Full Guide] ➜ ➜ ➜ https://bit.ly/43ZVNRN
➡️ Vitamin D
Vitamin D is a fat-soluble vitamin that is essential for many functions in the body, including cardiovascular health. It helps regulate the amount of calcium and phosphorus in the body, which are important minerals for maintaining strong bones and teeth, and also helps regulate blood pressure and the immune system.
➡️ Vitamin B9
Vitamin B9, also known as folate, is a vitamin that is essential for many functions in the body, including cardiovascular health. Folate plays a role in producing red blood cells, converting homocysteine into methionine, and maintaining DNA and RNA synthesis.
➡️ Omega-3 Fatty Acids
Omega-3 fatty acids are a type of polyunsaturated fatty acid that is essential for cardiovascular health. They are known for their anti-inflammatory properties, which help regulate blood lipid levels, such as cholesterol and triglycerides.
➡️ Magnesium
Magnesium is a mineral that is essential for the normal functioning of the human body. It is involved in over 300 metabolic reactions, including the regulation of heart rhythm and blood pressure.
➡️ Inositol
Inositol is a type of carbohydrate that is found in small amounts in certain foods, including whole grains, fruits, and nuts. It is also available in supplement form. Studies have shown that inositol may have potential benefits for the heart, including improving insulin sensitivity and reducing oxidative stress.
➡️ Fiber
Fiber is a type of carbohydrate that is not digested by the body and is found in plant-based foods such as fruits, vegetables, whole grains, and legumes. There are two main types of fiber: soluble fiber and insoluble fiber. Both types of fiber have been shown to have beneficial effects on the cardiovascular system.
➡️ L-Carnitine
L-carnitine is an amino acid-like substance that is found in the body and can also be obtained from certain foods. It plays a critical role in the production of energy in the body by transporting long-chain fatty acids into the cells’ mitochondria for oxidation and energy production.
➡️ Garlic
Garlic is a plant in the Allium family that is widely used for its strong flavor and potential health benefits. Not to mention, it has been used for centuries for its medicinal properties, including improving cardiac health.
➡️ Green Tea
Green tea is a type of tea made from Camellia sinensis leaves and is known for providing several positive health benefits. Green tea is rich in antioxidants, particularly catechins, which are believed to contribute to a healthier heart.
➡️ Coenzyme Q10
Coenzyme Q10, or CoQ10 for short, is a naturally occurring substance that is found in every cell in the body and plays a critical role in energy production. It is also an antioxidant that helps protect cells from damage.
💥Heart Attack Vitamins [Full Guide] ➜ ➜ ➜ https://bit.ly/43ZVNRN
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:44 - Vitamin D
1:31 - Vitamin B9
2:23 - Omega-3 Fatty Acids
3:11 - Magnesium
3:55 - Inositol
4:35 - Fiber
5:31 - L-Carnitine
6:21 - Garlic
7:23 - Green Tea
8:08 - Coenzyme Q10
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#heartattack #heartvitamins #heartattackprevention
79
views
Inhaled Nitric Oxide (iNO) in Newborns *EXPLAINED*
What is Inhaled Nitric Oxide (iNO)? We created this video to cover the medical definition and provide a brief overview of this topic.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
💥Medical Gas Therapy [Full Guide] ➜ ➜ ➜ https://bit.ly/2VjWLqR
➡️ Inhaled nitric oxide (iNO) is a selective pulmonary vasodilator that has been studied and utilized for a variety of respiratory conditions.
-- Persistent Pulmonary Hypertension of the Newborn (PPHN)
INO has been approved by the FDA for treating PPHN in neonates. It helps to reduce the need for extracorporeal membrane oxygenation (ECMO) by improving oxygenation and reducing pulmonary vascular resistance in affected infants.
-- Acute Respiratory Distress Syndrome (ARDS)
Although not FDA-approved for this indication, iNO has been used off-label for treating ARDS in both adults and children. It may help to improve oxygenation and reduce the need for mechanical ventilation in these patients.
-- Pulmonary Hypertension
INO has been investigated as a potential treatment for various forms of pulmonary hypertension, including chronic thromboembolic pulmonary hypertension (CTEPH) and pulmonary arterial hypertension.
Studies have shown that INO may improve exercise capacity and hemodynamics in these patients. INO is not routinely used in the management of respiratory failure associated with prematurity. INO can be administered in newborns with mechanical ventilation by using a specially designed system that is capable of precision drug dosing. The recommended dose for INO is 20 ppm.
When a desired outcome has been achieved, the INO dose is gradually titrated by 50% increments to reach a final dose of 1 ppm. Then the drug is discontinued. The patient may experience a rebound effect and withdrawal symptoms, which can be mitigated by increasing the delivered FiO2. INO should be accessible in every hospital with a level III intensive care nursery, and it should also be integrated into high-risk transport teams. Non-ECMO centers should have a treatment failure plan that takes into consideration the distance to the nearest ECMO center. Inhaled nitric oxide (iNO) is an important gas for treating newborns who require mechanical ventilation for hypoxemic respiratory failure.
💥Respiratory Therapy Definitions [Glossary] ➜ ➜ ➜ https://bit.ly/3g6s4Pj
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:24 - Inhaled Nitric Oxide (iNO)
0:35 - Persistent Pulmonary Hypertension of the Newborn (PPHN)
1:01 - Acute Respiratory Distress Syndrome (ARDS)
1:23 - Pulmonary Hypertension
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#respiratorytherapy #respiratorytherapist #respiratorytherapyschool
43
views
Diagnosing and Assessing a Patient (TMC Practice Question)
The video breaks down a sample TMC practice question about assessing and diagnosing a patient. Do you know the correct answer?
💥TMC Test Bank [Practice Questions] ➜ ➜ ➜ https://bit.ly/3QNqwLX
💥Daily Practice Questions [via Email] ➜ ➜ ➜ http://bit.ly/2NnXh3C
➡️ Question:
During the assessment of a 64-year-old female patient, you note the following signs: dyspnea, hypotension, and a tracheal shift to the right. The patient has absent breath sounds, reduced chest expansion, and a hyperresonant percussion note, all on the left side. These findings suggest which of the following?
A. Pleural effusion on the left side
B. Pneumothorax on the left side
C. Atelectasis on the left side
D. Consolidation on the left side
To get this one correct, you needed to interpret ALL information provided in the question. This is a common question format that you'll see on the TMC Exam. The question states that the patient has reduced chest expansion, a hyperresonant percussion note, and absent breath sounds on the left side. It also points out a tracheal shift to the right. All of these suggest that the patient has a pneumothorax on the left side.
Remember: The trachea will shift away from the affected side when a pneumothorax is present. Therefore, you can rule out left-sided atelectasis because, if that were the case, the trachea would shift to that side. Pleural effusion and consolidation would cause a dull percussion note, not a hyperresonant note. So, we can also rule those two out as well.
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:25 - Practice Question
1:00 - Explanation
1:54 - Correct Answer
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#respiratorytherapyzone #tmcexam #tmcpracticequestion
19
views
Top Early Warning Signs of Asthma *MUST KNOW* ⚠️
What are the early warning signs of asthma? What symptoms should you look for? Watch this video to find out!
💥Asthma Early Warning Sings [Full Guide] ➜ ➜ ➜ https://bit.ly/3N6Bb4P
➡️ Wheezing
Wheezing is a high-pitched whistling sound that occurs when air flows through narrowed airways. This symptom is common in asthma due to inflammation and constriction of the bronchial tubes, making it difficult to breathe.
➡️ Persistent Coughing
A persistent cough, especially one that worsens at night or during exercise, can be an early sign of asthma. This occurs as the body tries to clear excess mucus or irritants from the airways.
➡️ Chest Tightness
Asthma sufferers often experience a feeling of tightness, pressure, or discomfort in the chest due to inflamed and constricted airways, which makes it harder for the lungs to fully expand.
➡️ Hypoxemia
Hypoxemia refers to low oxygen levels in the blood. In asthma, this can occur when the lungs struggle to transfer oxygen from inhaled air to the bloodstream due to airway obstruction and inflammation.
➡️ Tachycardia
Tachycardia is an abnormally rapid heart rate, which can result from the body's effort to compensate for reduced oxygen levels in the bloodstream during an asthma attack.
➡️ Shortness of Breath
Difficulty breathing or feeling out of breath, particularly during physical activity, is a common early warning sign of asthma. This happens due to the narrowing of the airways and increased mucus production.
➡️ Cyanosis
Cyanosis is a bluish discoloration of the skin and mucous membranes, often seen around the lips and fingernail beds. This can occur in severe asthma cases when oxygen levels in the blood become critically low.
➡️ Fatigue
People with asthma may feel fatigued or weak due to the persistent struggle to breathe, which requires more energy and can lead to exhaustion.
➡️ Rapid Breathing
Rapid or shallow breathing can be a sign of asthma, as the body tries to compensate for the decreased airflow through the constricted airways.
➡️ Difficulty Sleeping
Asthma symptoms, such as coughing, wheezing, and shortness of breath, can worsen at night, making it difficult for individuals to sleep comfortably. This is known as nocturnal asthma and can be a significant indicator of the condition.
💥Asthma Early Warning Sings [Full Guide] ➜ ➜ ➜ https://bit.ly/3N6Bb4P
—————
📘 FREE STUFF
▪ Free Cheat Sheets 👉 https://bit.ly/3IKenWk
▪ TMC Practice Exam 👉 http://bit.ly/2XlwASL
📗 PASS THE TMC EXAM
▪ TMC Test Bank 👉 https://bit.ly/3QNqwLX
▪ TMC Exam Hacks 👉 https://bit.ly/3iLmVS2
▪ Daily TMC Practice Questions 👉 http://bit.ly/2NnXh3C
▪ TMC Bundle (Save $) 👉 https://bit.ly/3CWhdUn
📕 MORE FROM RTZ
▪ Test Bank (Free) 👉 http://bit.ly/2Kp73ln
▪ Glossary 👉 https://bit.ly/3g6s4Pj
▪ About Us 👉 http://bit.ly/2Xgk5YH
▪ Testimonials 👉 http://bit.ly/2x7b5Gl
🌐FOLLOW US
▪ Instagram 👉 http://bit.ly/2FhF0jV
▪ Twitter 👉 http://bit.ly/2ZsS6T1
▪ Facebook 👉 http://bit.ly/2MSEejt
▪ Pinterest 👉 http://bit.ly/2ZwVLPw
▪ Rumble 👉 https://bit.ly/3p7IS0H
▪ LinkedIn 👉 https://bit.ly/41uO2lx
🚑MEDICAL DISCLAIMER
This content is for educational and informational purposes only. It is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Please consult with a physician with any questions that you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you watch in this video. We strive for 100% accuracy, but errors may occur, and medications, protocols, and treatment methods may change over time.
💡AFFILIATE DISCLAIMER
This description contains affiliate links. If you decide to purchase a product through one of them, we receive a small commission at no cost to you.
—————
⏰TIMESTAMPS
0:00 - Intro
0:41 - Wheezing
0:58 - Persistent Coughing
1:15 - Chest Tightness
1:30 - Hypoxemia
1:46 - Tachycardia
2:00 - Shortness of Breath
2:22 - Cyanosis
2:42 - Fatigue
2:53 - Rapid Breathing
3:08 - Difficulty Sleeping
3:25 - Exercise Intolerance
3:46 - Increased Mucus Production
4:04 - Frequent Upper Respiratory Tract Infections
4:25 - Difficulty Speaking Due to Lack of Air
4:42 - Pale, Sweaty Face
4:57 - Feelings of Anxiety and Panic
5:14 - Feelings of Confusion
5:34 - Itching of the Chin or Neck
5:49 - Nasal Congestion
6:01 - Sore Throat
6:17 - Clammy Skin
6:35 - Posture Changes
6:49 - Decrease in Peak Flow Reading
7:14 - Restlessness
7:28 - Dizziness
7:40 - Changes in Speech Patterns
7:55 - Dry Mouth
8:11 - Dark Bags Under Your Eyes
8:25 - Increased Need for Inhaler Use
—————
🖼CREDIT FOR MUSIC/GRAPHICS:
▪ Music licensed from Audiojungle.net/
▪ Graphics: Canva.com, Freevector.com, Vecteezy.com, and Pngtree.com
#asthma #asthmaproblems #asthmaawareness
88
views